Digestive System
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
DIGESTIVE SYSTEM
On the basis of the embryonic origin, the alimentary canal of vertebrates can be divided into three parts –
(A) Fore gut / Stomodaeum : Ectodermal. It includes buccal cavity / oral cavity.
(B) Mid gut / Mesodaeum : Endodermal. It includes pharynx, oesophagus, stomach, small intestine, and large intestine.
(C) Hind gut / Proctodaeum : Ectodermal. It includes anal canal and anus.
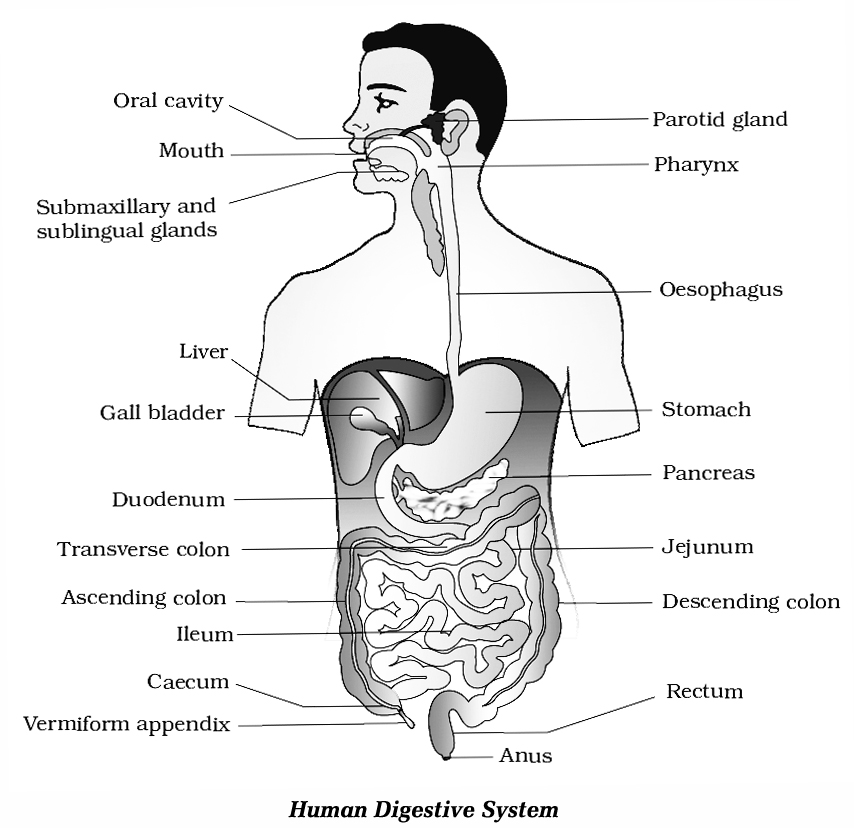
Digestive system of man consists of alimentary canal and some accessory digestive organs.
The Alimentary Canal:
It is a coiled muscular tube about 6 -9 metres long extending from mouth to anus.
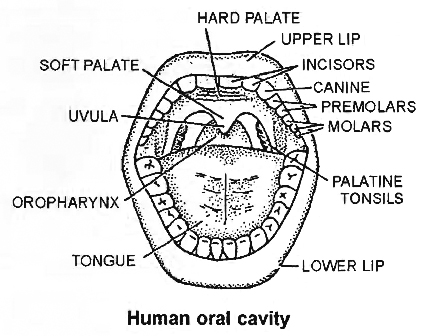
Mouth:
The mouth is an opening bounded by upper and lower lip.
Lips are attached on the inner side with the gums by thin transparent fold called Labial frenulum.
The space between lips and teeth is called vestibule.
The roof of buccal cavity is palate consisting of hard palate (maxilla, premaxilla and palatine bones) anteriorly and soft palate posteriorly.
Mucus epithelium has thick transverse folds called palatine rugae.
Terminal part of soft palate hangs in the throat called uvula. On sides of uvula tonsils are present which are made of lymphatic tissue.
The floor of buccal cavity is occupied by a muscular tongue attached at base by a fold called lingual frenulum.
Teeth present on upper and lower jaws are
(i) Incisors: for cutting, have one root.
(ii) Canines: for tearing, have one root.
(iii) Premolars: for crushing, grinding and chewing, in upper premolar 2 roots and lower premolar 1 root.
(iv) Molars: for chewing, in upper molar 3 roots and lower molar 2 roots.
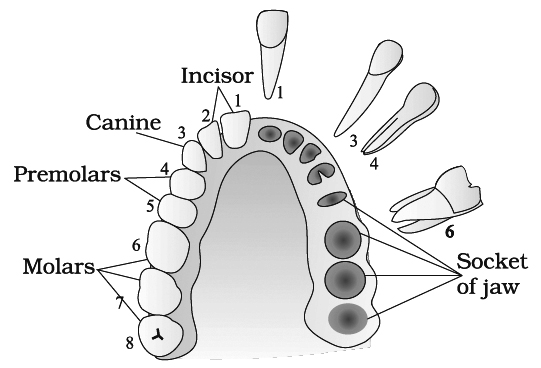
one side and the sockets on the other side
Dental formulae
In man, 20 teeth grow twice during life time i.e., diphyodont![]() ; (premolars and last molars absent In primary dentition) and 12 teeth appear only once i.e., Monophyodont.
; (premolars and last molars absent In primary dentition) and 12 teeth appear only once i.e., Monophyodont.![]()
Child =![]()
17 yr. old =![]()
Adult =![]()
Tongue
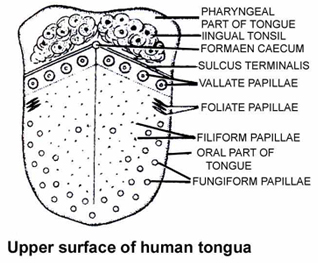
The tongue is a voluntary muscular and glandular structure which occupies the floor of the mouth.
It is attached to the floor of the mouth by a fold called the frenulum of the tongue.
An inverted V-shaped furrow called the sulcus terminalis divides the upper surface of the tongue into anterior oral part and posterior pharyngeal part.
The apex of the sulcus terminalis projects backwards and is marked by a small median pit, named the foramen caecum.
The foramen caecum is an embryological remnant and marks the site of the upper end of the thyroglossal duct. Oral part of the tongue has papillae on its surface.
These are :
(i) Filiform papillae : smallest, most abundant and have no taste buds.
(ii) Fungiform papillae : appear as red dots on tongue and contain taste buds.
(iii) Foliate papillae: absent in man.
(iv) Circumvallate papillae: largest in size and knob like, also contain taste buds.
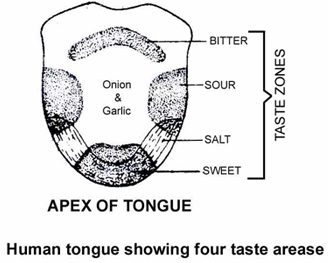
The different areas of tongue are demarcated as follows:
Tip – sweet
Tip and sides – salt
Sides – sour
Base – bitter
Sweat glands of dogs are present on tongue (panting of dog).
Salivary Glands
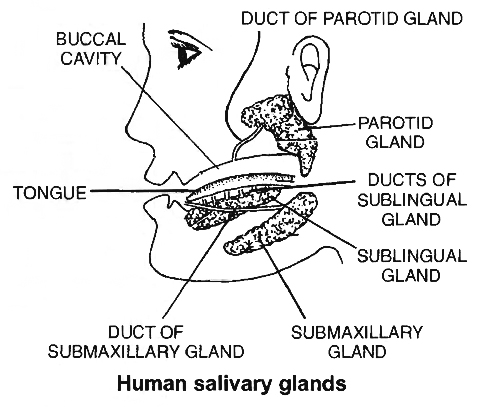
Four pairs of salivary glands open in the mouth cavity:
(i) Parotid: Largest -present below and in front of ears -Stenson's duct.
(ii) Submaxillary: Medium sized -present at the angles of jaw lower -Wharton's duct
(iii) Sublingual : Smallest -located below the tongue - Rivinus duct.
(iv) Infra orbital : Absent in man, otherwise present below eyes e.g. , in rabbit.
Daily Secretion of saliva is 1.5 litres, (pH of saliva is 6.7) and has salivary amylase (ptyalin), maltase and lysozyme.
Salivary glands are stimulated to secrete saliva by parasympathetic innervation while sympathetic nerves causes reduced secretion leading to drying of mouth.
Cl– are required for activation of salivary amylase. Mumps is viral infection of salivary glands (mainly Parotid).
Pharynx opens through gullet into the oesophagus and through glottis into the larynx.
An elastic cartilage plate, epiglottis, covers the glottis at the time of swallowing. Food mixed with saliva in buccal' cavity-Bolus.
Oesophagus
It is a long and thin tube, 25 cm long that pierces the diaphragm and enters the abdominal cavity.
Oesophagus is characterised by :
(i) Absence of visceral peritoneum. Its outermost fibrous (non-coelomic) covering is called tunica adventitia.
(ii) Absence of digestive glands. It has mucus-secreting goblet cells.
(iii) Presence of mucous membrane formed of non-keratinised stratified squamous epithelium some cells of which are ciliated.
(iv) Presence of voluntary (upper 1/3rd) and involuntary muscle fibres (lower 2/3rd).
Stomach
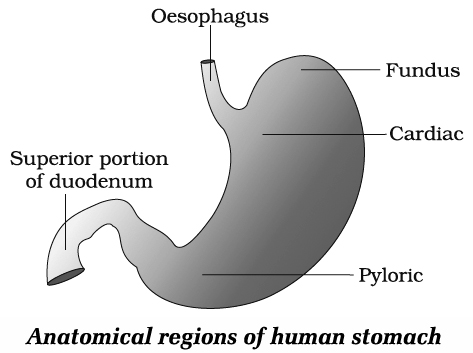
Stomach is oval and pouch like organ, divisible into cardiac, fundic, main body and pyloric parts.
Cardiac sphincter is present at the opening of oesophagus into stomach and prevents the regurgitation of food into oesophagus.
The pyloric part opens into small intestine and opening is guarded by pyloric sphincter.
The wall of stomach has three layers of muscles, outermost longitudinal layer, middle circular layer and innermost of oblique layer.
Mucosa has folds called rugae and cardiac, fundic and pyloric glands.
Only fundic glands secrete gastric juice.
These contain neck cells (secrete mucus and present in all three types of glands), oxyntic or parietal cells (secrete HCl and Castle's intrinsic factor for absorption of B12).
HCl of gastric juice converts Fe3+ into Fe2+ which makes the absorption of iron possible.
Non-secretion of HCl (achlorhydria) or gastrectomy can lead to iron-deficiency anaemia.
The peptic cells or chief cells or zymogenic cells release large quantity of pepsinogen and other enzymes.
Small Intestine
First part of small intestine is duodenum. It is 25 cm long, U or C-shaped in humans and receives the opening of hepatopancreatic duct (Bile duct + Pancreatic duct).
A small swelling is present at the opening of hepatopancreatic duct and is called 'Ampulla of Vater' or Hepatopancreatic ampulla and the opening is regulated by sphincter of oddi.
Other parts of small intestine are jejunum and ileum.
The wall of intestine has thin layers of longitudinal and circular muscles.
Mucosa has folds called plicae circulare (folds of Kerkrings or Valvulae conniventes) and villi towards lumen of the intestine.
Epithelial cells lining the villi have microvilli which further increase the absorptive area.
Intestinal glands or Crypts of Leiberkuhn have epithelial cells (secrete mucus), Paneth cells (secrete digestive enzymes) and argentaffin cells (probably secrete hormones).
In duodenum, Brunner's glands are also present (located in submucosa) which secrete mucus.
Diffused patches of lymphoid tissues are present throughout the small intestine and are aggregated in ileum to form Peyer's patches.
Large Intestine
It is about 1.5 m long and consists of three parts -Caecum, Colon and Rectum.
A blind pouch of caecum is vermiform appendix.
These parts help in digestion of cellulose in herbivores.
Wall of colon has sac like haustra.
Histologically, wall of colon has three bands of longitudinal muscles called taeniae coli.
Another characteristic of colon surface is the presence of small fat filled projections called epiploic appendages.
The colon is divisible into ascending, transverse, descending and sigmoid colon.
Ascending colon is the smallest part and lacks mesentry.
Last part of rectum is anal canal having a strong sphincter. It opens outside by anus.
DIGESTIVE GLANDS
Liver
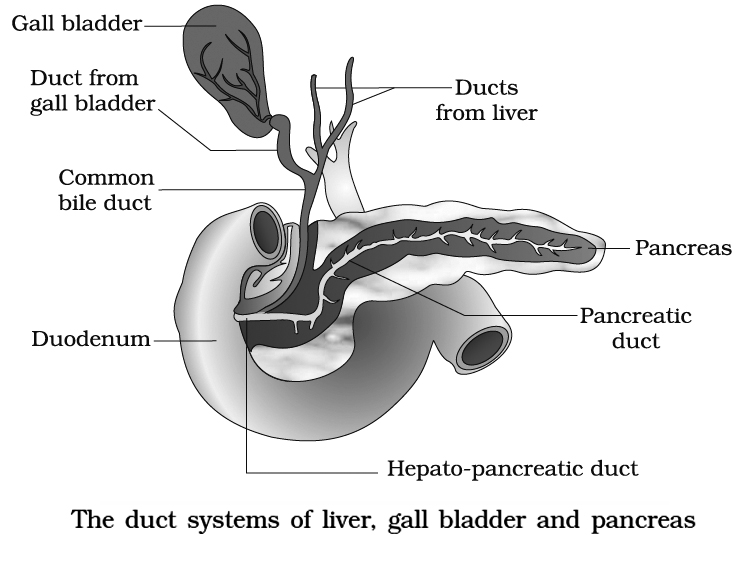
Largest digestive gland. It lies in the upper right side of the abdominal cavity just below diaphragm.
The liver is divided into two main lobes-right and left.
Between the right and left lobes, falciform ligament is present.
The right lobe is differentiated further into right lobe proper, a quadrate lobe and caudate lobe.
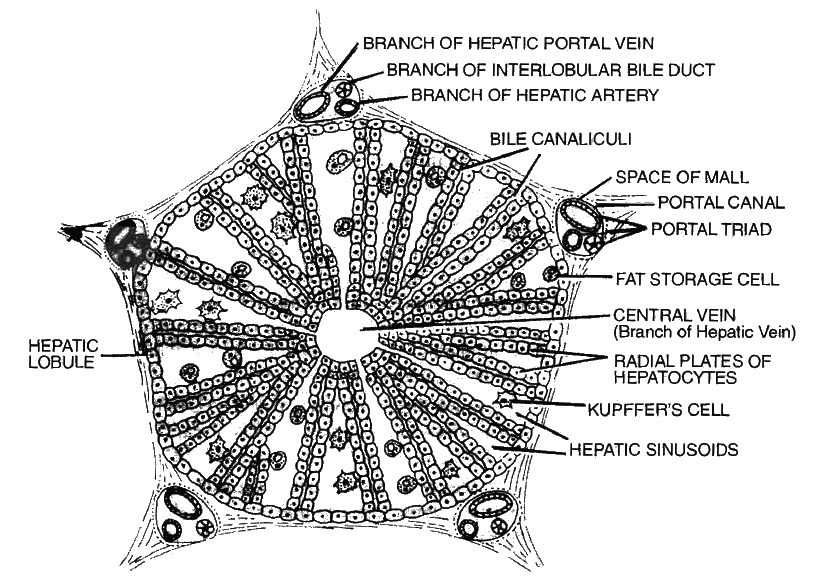
Liver is surrounded by Glisson's capsule, its trabeculae divide liver lobes into hexagonal lobules.
Polyhedral hepatocytes are arranged in cords around a central venule.
Portal triads contain hepatic artery, portal venule, bile ductule and lymphatics.
Blood sinusoids are present.
Kupffer cells are present in sinusoids and are phagocytic.
Gall bladder is situated on the inferior surface of right lobe. It is 8 cm long and 2 cm wide.
Bile is secreted by hepatocytes into the bile canaliculi, a series of narrow spaces between adjacent liver cells.
The canaliculil drain via bile ductules into bile ducts, which run in portal tracts; the bile duct themselves discharge into the right and left hepatic ducts which unite to form the common hepatic duct at the hilum of the liver.
Gall bladder has a capacity of 30 to 50 ml. It consists of smooth muscles lined by columnar epithelium.
It fills and empties via cystic duct which joins the common hepatic duct to form the bile duct; this in turn empties into the duodenum through the ampulla of Vater (hepatopancreatic ampulla).
At the point of its entry into the duodenum, the bile duct and adjacent pancreatic duct join each other.
The sphincter of Boyden surrounds the opening of bile duct.
Sphincter of oddi surrounds the ampulla of Vater.
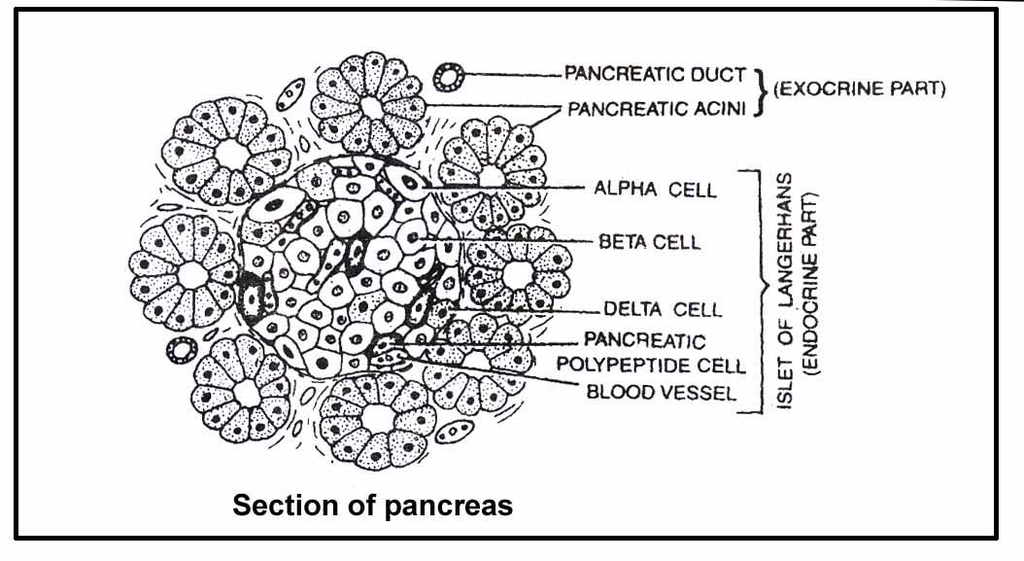
Pancreas
It is a racemosely branched gland, situated between stomach and duodenum.
Pancreas consists of acini (which secrete digestive enzymes) and islets of Langerhans (which secrete insulin and glucagon hormones).
Pancreas has two ducts within it.
The first is duct of Santorini which is accessory or nonfunctional, opening directly into duodenum and the other is duct of Wirsung which is functional and combines with bile duct to form common hepatopancreatic duct.
mechanism of food digestion
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
Mechanism of Food DIGESTION
Digestion of Carbohydrates :
The diet of most of the animals including man consists of carbohydrates.
Depending upon the complexity, carbohydrates are of three types : polysaccharides, disaccharides and monosaccharides.
During the process of digestion, both poly and disaccharides are broken down to monosaccharides and in this form they can be absorbed into the body.
Some of these complex carbohydrates are starch and cellulose present in cereal grains, potato, fruits and tubers; sucrose present in cane sugar; lactose present in milk etc.
Enzymes that act on carbohydrates are collectively known as carbohydrases.
Pancreatic juice and intestinal juice also contain carbohydrate digesting enzymes.
Pancreatic juice contains pancreatic amylase that acts on starch to digest it into maltose, isomaltose and dextrin.
The secretions of the brush border cells constitute the intestinal juice or succus entericus.
This juice contains a variety of enzymes like disaccharidases (e.g., maltase), dipeptidases, lipases, nucleosidases etc.
Starch![]() Maltose + Isomaltose + Dextrin
Maltose + Isomaltose + Dextrin
Maltose + Isomaltose + Dextrin![]() Glucose
Glucose
Sucrose![]() Glucose + Fructose
Glucose + Fructose
Lactose![]() Glucose + Galactose
Glucose + Galactose
Digestion of Proteins:
Proteins are complex organic compounds made up of smaller units called amino acids. So in the process of digestion, all proteins are broken down to amino acids.
Enzymes that hydrolyse proteins are collectively known as proteases or peptidases.
Many of these enzymes are secreted in their inactive form or proenzymes as their active form would hydrolyse cellular and extracellular proteins of the organism itself.
Inactive enzymes are converted to their active form only at the site of action.
Saliva as such does not contain any protein digesting enzyme, but it can denature the uncooked natural proteins like the ones present in raw egg, unboiled milk or uncooked germinating seeds.
However, this is not a process of hydrolysis as in digestion.
Action of Gastric Juice:
The gastric glands of stomach produce a light coloured, thin and transparent gastric juice.
It contains water, hydrochloric acid (0.3%) and inactivated enzymes prorennin and pepsinogen.
The presence of HCl makes the medium highly acidic (pH = 1 or 2) so that pepsin can act on proteins to convert them into peptones and proteoses.
However, there is no pepsin in invertebrates.
Both prorennin and pepsinogen are converted to their active forms in the presence of HCl.
Pepsin and rennin can also do the same function once they are formed.
HCl also helps to kill bacteria and other harmful organisms that may be present along with the food.
Rennin acts on the casein protein of milk and converts it into paracasein which in the presence of calcium ions forms calcium paracaseinate (curdling of milk).
The function of rennin is then taken over by pepsin and other milk-coagulating enzymes. Pepsin then acts on it.
These reactions are summarized below:
Prorennin (inactive)![]() Rennin (active)
Rennin (active)
Pepsinogen (inactive)![]() Pepsin (active)
Pepsin (active)
Milk Casein![]() Paracasein
Paracasein
Paracasein + Ca++![]()
![]()
Calcium paracaseinate![]() Peptones and proteoses
Peptones and proteoses
Action of Pancreatic and Intestinal Juice:
Both pancreatic juice and intestinal juice (succus entericus) are poured into small intestine.
Pancreatic juice contains trypsinogen, chymotrypsinogen, procarboxypeptidases, lipases, amylases or amylopsin, DNAases and RNAases.
All these enzymes of pancreatic juice can act only in the alkaline medium.
This change in the medium of food, from acidic to alkaline, is done by the bile juice.
Therefore, bile juice acts on the food before the action of pancreatic juice.
All these actions are given below :
Trypsinogen (inactive)![]() Trypsin (active)
Trypsin (active)
Peptones and proteoses![]() Peptides
Peptides
Chymotrypsinogen (inactive) is activated to chymotrypsin by trypsin itself.
Chymotrypsin is another important milk coagulating enzyme and can hydrolyse casein into paracasein which then coagulates to form calcium paracaseinate.
However unlike rennin, it acts in the alkaline medium.
Chymotrypsin can act on other proteins also.
Digestion of Fats:
Fat digestion starts only when the food reaches the stomach.
Some amount of gastric lipase is present.
Gastric lipase is of little importance except in pancreatic insufficiency.
Most of the fat digestion begins in the duodenum, pancreatic lipase being one of the most important enzymes involved.
Bile juice contains bile salts that break down the bigger molecules of fat globules into smaller droplets by reducing the surface tension of fat droplets.
This process is known as emulsification of fats.
Lipase is the chief enzyme that acts on emulsified fats.
It is present both in the pancreatic juice and intestinal juice.
Pancreatic lipase (steapsin) is the principal enzyme involved in fat digestion.
Lipase converts emulsified fats into diglyceride and monoglycerides releaSing fatty acids at each step.
At the end of digestion, all fats are converted into fatty acids, glycerol and monoglycerides.
Absorption of Digested Products
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
Absorption of digested products
Absorption is the process by which the end products of digestion pass through the intestinal mucosa into the blood or lymph.
It is carried out by passive, active or facilitated transport mechanisms.
The passage of various substances into the blood depends upon the concentration gradients.
However, some of the substances like fructose and some amino acids are absorbed with the help of the carrier proteins.
This mechanism is called the facilitated transport.
Transport of water depends upon the osmotic gradient.
Active transport occurs against the concentration gradient and hence requires energy.
Various nutrients like amino acids, monosaccharides like glucose, electrolytes like Na+ are absorbed into the blood by this mechanism.
Fatty acids and glycerol being insoluble, cannot be absorbed into the blood.
They are first incorporated into small droplets called micelles which move into the intestinal mucosa.
They are re-formed into very small protein coated fat globules called the chylomicrons which are transported into the lymph vessels (Iacteals) in the villi.
These lymph vessels ultimately release the absorbed substances into the blood stream.
Absorption of substances takes place in different parts of the alimentary canal, like mouth, stomach, small intestine and large intestine.
However, maximum absorption occurs in the small intestine. A summary of absorption (sites of absorption and substances absorbed) is given in table.
Table: The Summary of Absorption in Different Parts of Digestive System
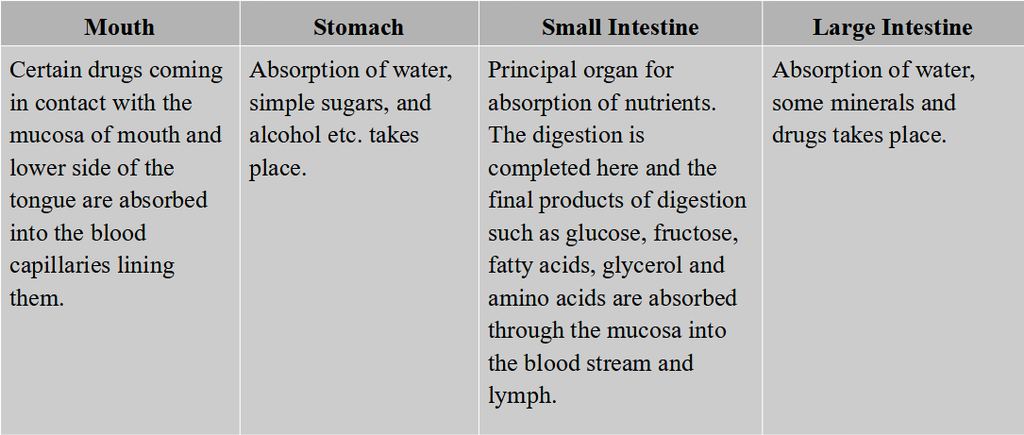
The absorbed substances finally reach the tissues which utilise them for their activities. This process is called assimilation'
The digestive wastes, solidified into coherent faeces in the rectum initiate a neural reflex causing an urge or desire for its removal.
The egestion of faeces to the outside through the anal opening (defaecation) is a voluntary process and is carried out by a mass peristaltic movement.
Disorders of Digestive System
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
Disorders of Digestive System
The inflammation of the intestinal tract is the most common ailment due to bacterial or viral infections. The infections are also caused by the parasites of the intestine like tape worm, round worm, thread worm, hook worm, pin worm, etc.
Jaundice: The liver is affected, skin and eyes turn yellow due to the deposit of bile pigments.
Vomiting : It is the ejection of stomach contents through the mouth. This reflex action is controlled by the vomit centre in the medulla. A feeling of nausea precedes vomiting.
Diarrhoea: The abnormal frequency of bowel movement and increased liquidity of the faecal discharge is known as diarrhoea. It reduces the absorption of food.
Constipation: In constipation, the faeces are retained within the rectum as the bowel movements occur irregularly.
Indigestion: In this condition, the food is not properly digested leading to a feeling of fullness. The causes of indigestion are inadequate enzyme secretion, anxiety, food poisoning, over eating and spicy food.
NUTRITIONAL REQUIREMENTS OF HUMANS
Energy Yielding Nutrients
Carbohydrates are used primarily as sources of chemical energy, to be either metabolised immediately as glucose or stored as glycogen.
The synthesis of glycogen is called glycogenesis.
The liver can store enough glycogen to maintain blood glucose level for several hours. Under acute starved conditions, the liver cells begin to convert fatty acids and the glycerol (digestive products of fat molecules) into glucose.
Such production of new glucose is known as gluconeogenesis. Proteins are used as structural components of tissues, as channels, transporters, regulatory molecules and enzymes.
Proteins can also be utilised as energy sources, when broken down to amino acids.
Out of the 20 amino acids identified so far as the constituents of proteins, 8 (10 in children) cannot be synthesised in human body.
These must be provided in the diet from outside are designated as essential amino acids.
Lipid (fat) molecules are especially suitable as concentrated energy reserves.
The fat cell of adipose tissues are often called the fat depot of body.
Triglycerides are used as fuel.
Human body is able to synthesise most of the lipids in enough quantity, except three polyunsaturated fats, such as linoleic, linolenic and arachidonic acids.
These essential fatty acids must be provided to the human body through diets.
Minerals and Vitamins
Both minerals and vitamins occur as small molecules and mostly, do not require digestion.
Minerals are ingested as salts dissolved in water or as part of organic compounds (food).
Still, a few of the minerals are absorbed with the aid of digestive Juices (like bile) and gastric juices.
Of the twenty-one essential minerals required by man, some are important for maintaining fluid balance whereas others help to regulate metabolism by acting as a component of enzymes.
Vitamins are essential for normal metabolism, growth and sound health.
Humans can synthesise vitamin A (retinol) with the help of plant pigment, carotene, which is available in yellow and green leafy vegetables.
Vitamin A forms retinal pigment of human eyes, such as rhodopsin of rod cells and iodopsin of cone cells.
Humans can also synthesise vitamin D (calciferol) in their skin in presence of ultra-violet rays. Although most animals can synthesise vitamin C from glucose, humans cannot; hence, they require it in their diet.
Nutritional Deficiencies and Disorders
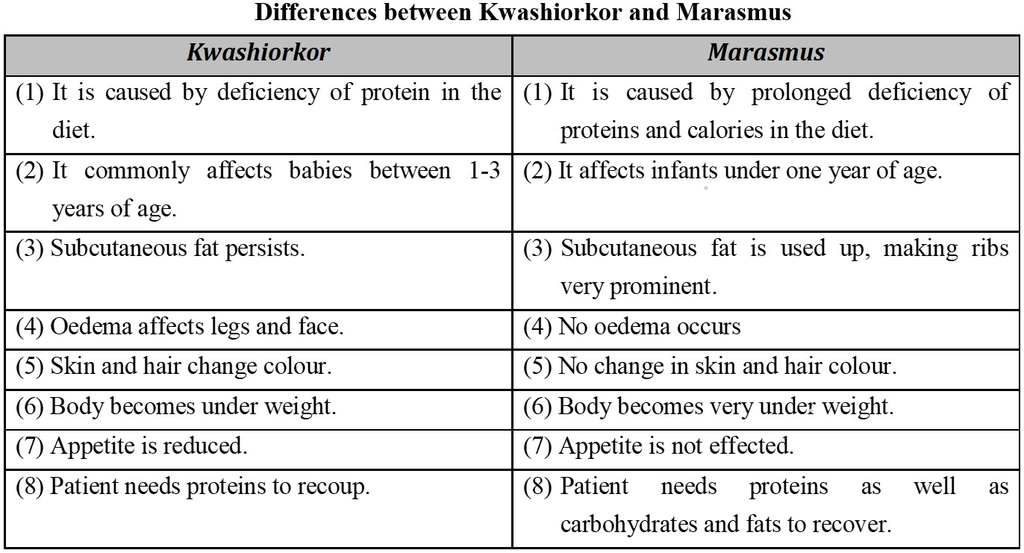
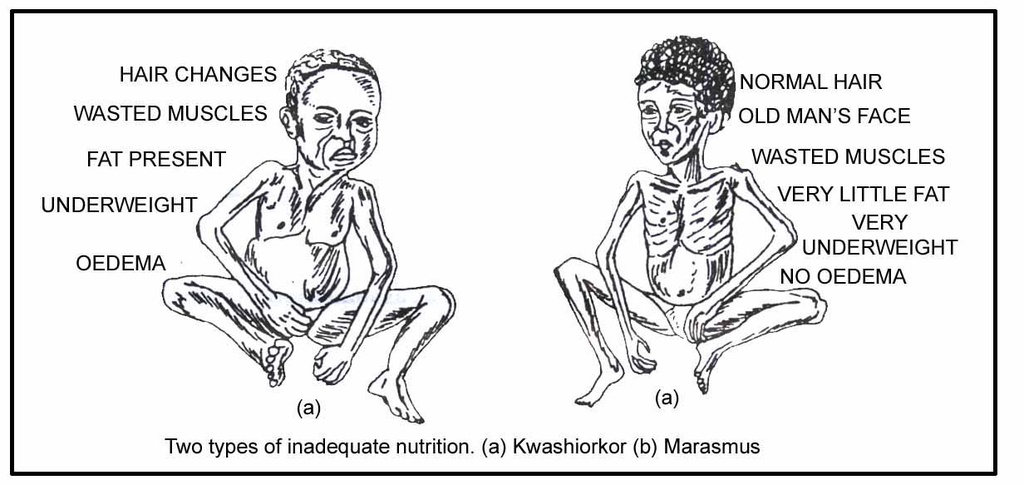
Deficiencies of nutrients, like vitamins, minerals and proteins, in the food are related to specific disorders, diseases and abnormalities in humans.
Impairment of health due to improper intake of food or nutrients results in malnutrition.
Malnutrition is a term which covers problems of both undernutrition and overnutrition.
An individual or a group of individuals, may be undernourished due to non-availability of food, and hence, deficiency of minimum required food and nutrients.
In this situation of undernutrition, the intake of food is too insufficient to meet the needs for metabolic energy.
Consequently, the individual shall have to make up the shortfall by metabolising some molecules of its own body.
Excess intake of food and nutrients may cause a great deal of harm to the body.
The excess nutrients are stored as increased body mass. Such a situation is attributep as overnutrition.
Excess intake of saturated fats, like butter, ghee, vegetable oils, red meat, eggs, etc., often leads to hypercholesterolemia, a condition in which blood cholesterol content becomes abnormally high, ultimately leading to cardiac disorder.
Deposition of cholesterol on the walls of blood vessels stiffens the blood vessels and increases blood pressure.
Besides, excessive intake of calories (sugar, honey, ghee etc.) may produce overweight and obesity (excessive accumulation of fat in tissues), which is the most common form of overnutrition.
Very high intakes of minerals and fat-soluble vitamins (obtained from food sources alone) can be toxic.
This is because they are stored in the body.
With the exception of folic acid (women of child-bearing age), people who have well-balanced diet that supply enough energy, do not usually need to take dietary supplements.
But, if they do decide to take supplements, then they should follow the advice on the label to reduce the risk of an overdose.
Respiratory Organs
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
Respiration organs
The process of exchange of O2 from the atmosphere with CO2 produced by the cells is called breathing, commonly known as respiration.

Human Respiratory System
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
HUMAN RESPIRATORY SYSTEM
The respiratory system of man consists of the following organs :
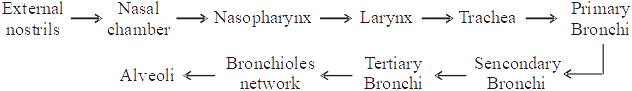
1. Nasal Cavity:
The nasal cavity is the first part of the respiratory system.
It opens to the exterior through nostrils.
Nasal cavity is divided into nasal chambers by the nasal septum. Each nasal chamber can be differentiated into three regions.
(i) Vestibular: First part starting from nostril, has oil glands and hair to prevent entry of large dust particles.
(ii) Respiratory part: Highly vascular and involved in conditioning of air as the air gets warmed and moist. Arising from the wall of each nasal chamber, there are 3 shallow bony ridges called nasal conchae. These are individually named as superior, middle and inferior. (Superior lies within the olfactory part; middle and inferior lie in the respiratory part). The conchae are covered with mucus membrane and greatly increase the surface of the nasal chambers.
(iii) Olfactory part: It is the upper part, lined by olfactory epithelium for smell.
2. Pharynx:
From the nasal cavity, the air enters the pharynx.
It serves as a common passage for both air and food.
The opening into the wind pipe or trachea is a narrow slit the glottis.The glottis is protected against the entrance of food by a triangular flap of tissue, the epiglottis.
3. Human Larynx:
Until puberty, there is little difference in the size of the larynx ('voice box') in male and female.
The larynx opens into the or opharynx by a slit like aperture, the glottis.
The larynx is composed of irregularly shaped cartilages attached to each other by ligaments and membranes.
The main cartilages are-
(i) Thyroid cartilage is the most prominent, C-shaped, incomplete dorsally, called Adam's apple as it is apple shaped and more prominent in male.
(ii) Cricoid cartilage lies below the thyroid cartila'ge, and its shape is like a signet ring.
(iii) Arytenoid cartilages are two roughly pyramid shaped cartilages forming posterior wall of the larynx.
(iv) Corniculate - These are two conical nodules of elastic fibro-cartilage which lie at the apices of arytenoid cartilages,
(v) Cuneiform - These are two small, elongated, club shaped nodules of elastic fibro-cartilage which lie above and anterior to corniculate cartilages. These connect epiglottis to arytenoid cartilage.
(vi) Epiglottis is a single leaf shaped cartilage which projects into the pharynx,
Thus a total of 9 cartilages -3 paired (iii, iv, v) and 3 unpaired (i, ii, vi).
The thyrohyoid membrane is a broad, flat membrane attached to the hyoid bone above and to the thyroid cartilage below.
Inside the larynx are present two pairs of vocal cords, one pair of false vocal cords which have little to do with sound production and the second inner pair or true vocal cords.
When air is forced through the larynx, it causes vibration of the true vocal cords and sound is produced.
The pitch of a sound is determined by the tension on the vocal cords-the greater the tension, the higher the pitch.

4. Trachea:
The trachea is a tube about 12 cm long with C shaped (dorsally incomplete) rings of hyaline cartilage in its walls.
These rings of cartilage make the wall non-collapsible.
It is internally lined by pseudostratified ciliated columnar epithelium.
Cilia beat to push out the mucus.
5. Bronchi:
The walls of the bronchi are likewise supported by cartilaginous rings.
Each bronohus divides and redivides into smaller and smaller bronchioles.
Epithelium gradually changes from pseudostratified ciliated columnar epithelium in the bronchi to ciliated simple cuboidal epithelium in the terminal bronchiole.
Incomplete rings of cartilage are gradually replaced by plates of cartilage that finally disappear in a distal bronchiole.
Terminal bronchiole is further subdivided into respiratory bronchioles. Respiratory bronchioles open into alveolar ducts ® atria ® alveolar sacs ® alveoli. From respiratory bronchioles onward the wall is very thin and is made up of simple squamous epithelium.
6. Lungs:
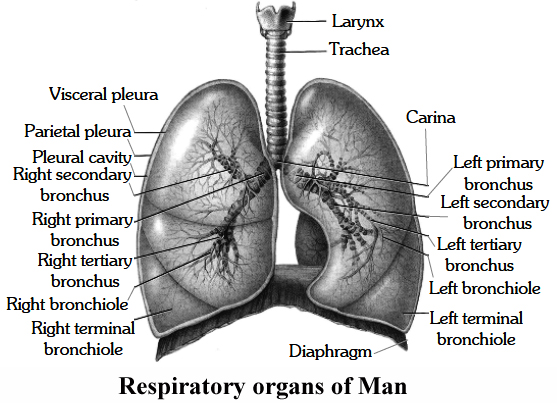
The lungs occupy the greater part of the thoracic cavity.
Surrounding each lung is a double walled sac within the walls of which lies, the pleural cavity.
The right lung is divided into three lobes and left into two.
Inside the lung each bronchus divides into numerous bronchioles, each of which terminates into an elongated saccule, the alveolar duct, which bears on its surface air sacs or alveoli.
The number of alveoli in the human lungs has been estimated to be approximately Respiratory organs of man 300 million.
The lungs are covered by a thin double layer of simple squamous epithelium called the pleura.
The outer or parietal pleuron remains attached to the wall of thoracic cavity.
The space between the two pleural membranes contains pleural fluid for reducing friction and makes the movement of lung easy.
Inflammation of the pleura causes a disease called 'pleurisy'.
Lungs are pink at birth.
They become dark grey and mottled in adults due to deposition of carbonaceous materials.
Darkening increases in smokers and persons exposed to pollutants.
The right lung is shorter by about 2.5 cm due to raised position of diaphragm on the right side to accomodate liver.
The left lung is longer. It is, however, narrower than the right lung because it contains a cardiac notch for accomodating asymmetrically placed heart. Left lung is divisible by an oblique fissure into two lobes, left superior and left inferior.
Right lung has two fissures, horizontal and oblique. They divide the right lung into 3 lobes -right superior, right middle and right inferior. The lobes are divided internally into segments and segments into lobules.
There are 8 segments in the left lung and 10 segments in the right lung. On the average an adult right lung weighs 625 g, while the left lung weighs 565 g.
Mechanism of Breathing
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
MECHANISM OF BREATHING
Respiratory movements in man are carried out with the help of intercostal muscles and diaphragm.
There are two phases of each breathing movement, inspiration and expiration.
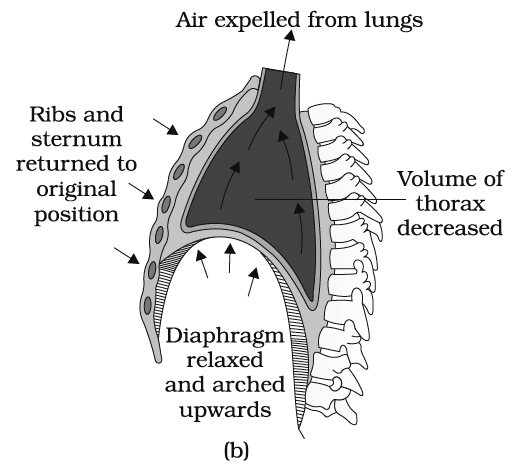
Mechanism of breathing showing: (a) inspiration, (b) expiration
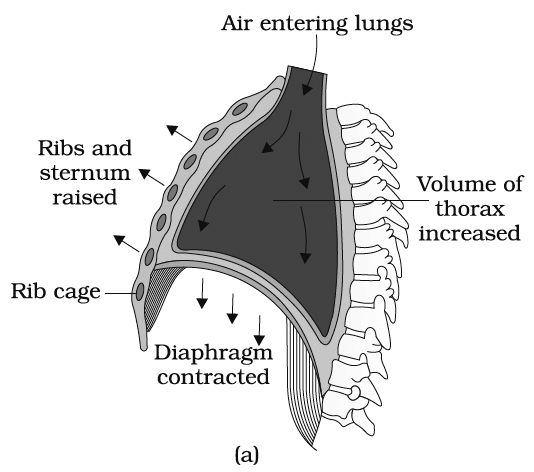
(1) Inspiration (Inhalation).
It involves intake of fresh air in the alveoli of the lungs. It includes an active process and consumes the mechanical energy.
There are two types of inspiratory muscles:
(a) Phrenic muscles: These muscles extend from diaphragm to ribs and vertebral column.
(b) External intercostal muscles. These are 11 pairs of muscles present between 12 pairs of ribs dorsoventrally and laterally. When phrenic muscles contract, the diaphragm is flattened whereas when extemal intercostal muscles contract, the ribs are pulled forward, upward and outward. The thoracic cavity increases in all directions which results in increase in volume and decrease in pressure. So, air moves into the lungs.
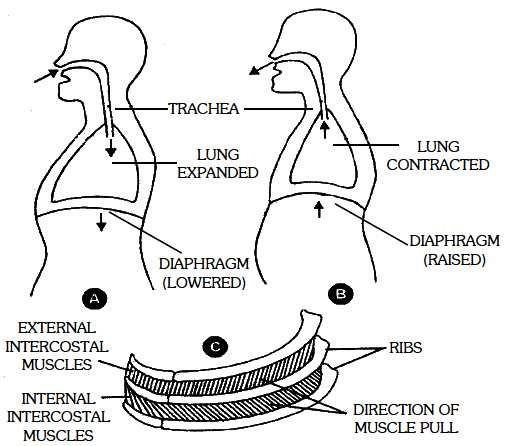
(B) during expiration, (C) at rest
(2) Expiration.
It involves the expelling of air of high pCO2 out of the body.
During rest, the expiration is a passive process and simply involves the relaxation of the inspiratory muscles (phrenic and external intercostal muscles).
These decrease the volume of thoracic cavity. But during forceful expiration, two expiratory muscles also help in expiration:
(a) Abdominal muscles. These extend from the ribs to the abdominal organs. When these contract, the abdominal visceral organs are pulled upward towards the diaphragm. So the diaphragm becomes more convex and thoracic cavity decreases anteroposteriorly.
(b) Internal intercostal muscles. These are also 11 pairs of muscles present between the ribs. When these contract, ribs are pulled backward, downward and inward, so thoracic cavity decreases dorsoventrally and laterally. Due to the above changes larger amount of air is passed out.
Pulmonary Volumes
(i) Tidal volume (TV): The volume of air inspired or expired involuntarily in each normal breath. It is about 500 ml of air in average young adult man.
(ii) Inspiratory reserve volume (IRV) : The maximum volume of air which a person can inhale over and above tidal volume by deepest possible voluntary inspiration. It is about 2500-3000 ml.
(iii) Expiratory reserve volume (ERV) : The volume of air which can be expired over and above the tidal volume with maximum effort. It is about 1000-1100 ml (according to NCERT).
(iv) Residual volume (RV) : The volume of air left in the lungs even after maximum forceful expiration. It is about 1100-1200 ml (according to NCERT).
Pulmonary Capacities
The combination of two or more pulmonary volumes. These include:
(i) Inspiratory capacity (IC) : Tidal volume + Inspiratory reserve volume. It is about 3000 -3500 ml.
(ii) Functional Residual Capacity (FRC) : Expiratory reserve volume + Residual volume. It is about 2500 ml.
(iii) Vital capacity (VC) : Inspiratory reserve volume + Tidal volume + Expiratory reserve volume. It varies from 3500 ml to 4500 ml depending upon age, sex and height of person.
(iv) Total lung capacity (TLC) : It is tidal volume + inspiratory reserve volume + Residual volume + Expiratory reserve volume. It is about 5800 ml.
With the exception of FRC and RV and TLC, all other lung values and lung capacities can be measured with the help of a simple spirometer.
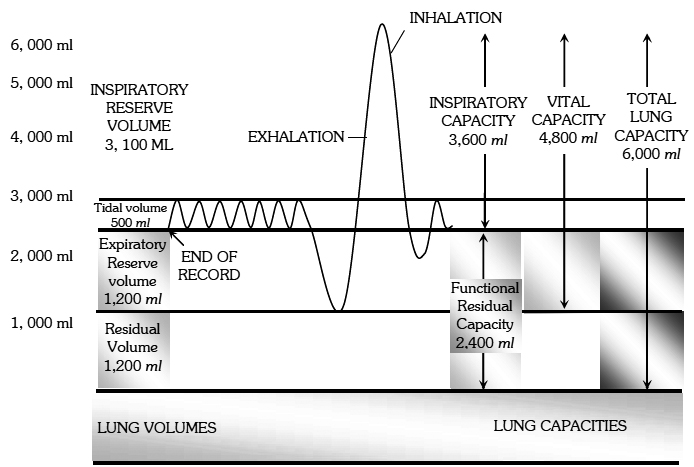
Various pulmonary air volumes
All pulmonary volumes and capacities are about 20% to 25% less in women than in men, more in athletic people than asthmatics.
Exchange of Gases
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
Exchange of Gases
Alveoli are the primary sites of exchange of gases.
Exchange of gases also occur between blood and tissues.
O2 and CO2 are exchanged in these sites by simple diffusion mainly based on pressure/ concentration gradient.
Solubility of the gases as well as the thickness of the membranes involved in diffusion are also some important factors that can affect the rate of diffusion.
Inspired air in the alveoli remains in close contact with blood.
The partition between the two include.
1. Alveolar epithelium
2. Alveolar epithelial basement membrane
3. Thin interstitial space
4. Capillary basement membrane
5. Capillary endothelial membrane
This whole part is called respiratory membrane and cumulatively form a membrane of 0.5 mm thickness.
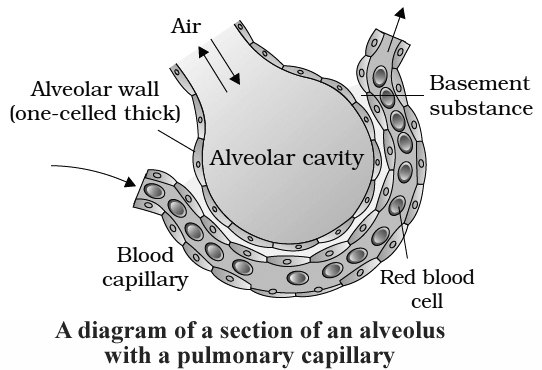
The limit of exchange between alveoli and pulmonary blood is diffusing capacity.
It is defined as volume of gas that diffuses through respiratory membrane in one minute for a
particle pressure difference of 1 mm Hg.
Solubility of the gases in lipids also affects diffusing capacity.
Diffusing capacity of CO2 is 20 times more than that of oxygen and the diffusing capacity of O2 is about double than that of nitrogen.
Surfactant:
A surface active agent -lecithin secreted by type II alveolar epithelial cells, reduces surface tension between the alveolar fluid and air.
It prevents collapsing of lung alveoli.
The exchange of gases between the alveoli and blood in the lungs, and the blood and the tissues is the result of difference in partial pressure of the respiratory gases, that is, oxygen and carbon dioxide.
External Respiration or Exchange at Alveoli Level
Partial pressure of O2 in the atmospheric air is 159 mm of Hg and that of CO2 is 0.3 mm of Hg.
Partial pressure of oxygen pO2 in alveolar air is 104 mm Hg and it is only 40 mm Hg in the arterial capillaries of the lungs.
Therefore, oxygen from the alveolar air rapidly diffuses into the blood capillaries due to its higher pO2.
In the expired air, it changes to 116 mm of Hg.
Similarly the pCO2 in the blood reaching the alveolar capillaries is 45 mm Hg whereas pCO2 in alveolar air is 40 mm Hg.
Therefore, CO2 rapidly leaves the blood capillaries and reaches the alveoli.
The pCO2 level in expired air is 32 mm Hg.
Internal Respiration or Exchange at Tissues Level
The gaseous exchange between the blood and body tissues is also due to the differential partial pressures. The pO2 and pCO2 of the arterial blood reaching the tissues is 95 mm Hg and 40 mm Hg respectively. The pO2 and pCO2 of tissues is 20 mm Hg and 52 mm Hg respectively. Therefore, oxygen quickly leaves the blood and enters the cells whereas CO2 produced in the tissues leaves the cells and enters the blood.
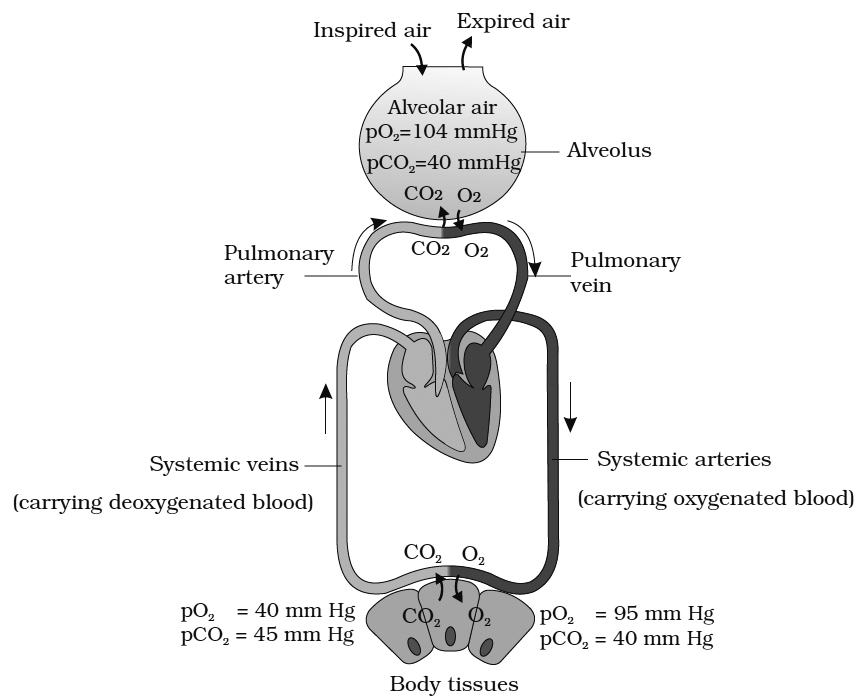
FACTORS THAT DECREASE OXYGENATION
1. Low blood volume
2. Anaemia
3. Low Hb
4. Poor blood flow
5. Pulmonary diseases
Transport of Gases
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
Transport of Gases
Oxygen Transport
Each decilitre of blood carries 19.8 ml of 02 of which 5 ml diffuses into tissues.
3% is transported dissolved in plasma and 97% is carried by the RBCs. Four Fe2+ ions of each haemoglobin can bind with 4 molecules of O2 and it is carried as oxyhaemoglobin.
Oxyhaemoglobin dissociates near tissues due to increase in acidity and decrease in pH. It can also be caused due to high temperature.
In a normal person, the haemoglobin level is about 15 per 100 ml.
The capacity of 1 g of haemoglobin to combine with O2 is 1.34 ml.
Therefore, arterial blood carries about 20 ml of O2/100 ml of blood.
Under normal condition, the O2 level falls to about 14.4 ml/100 ml in the venules.
It indicates that under normal condition, approximately 5 ml oxygen is transported by blood.
Under strenous conditions or during exercise, the O2 level falls to about 4.4 ml/100 ml i.e., approximately 15 ml of O2 is transported by Hb during exercise.
Bohr's Effect:
The relationship between the pO2 and percent saturation of haemoglobin when represented on a graph is termed as oxygen-haemoglobin dissociation curve and is sigmoid in shape. A rise in pCO2 or fall in pH decreases oxygen affinity of haemoglobin, raising the P50 value. This is called Bohr's effect (P50 value is the value of pO2 at which haemoglobin is 50% saturated with oxygen to form oxyhaemoglobin). Conversely a fall in pCO2 and rise in pH increases oxygen affinity of haemoglobin and shifts the curve to left. Foetal haemoglobin has a higher affinity for O2 because it binds BPG less strongly. Therefore, oxygen haemoglobin dissociation curve for foetal haemoglobin will appear on the left side.
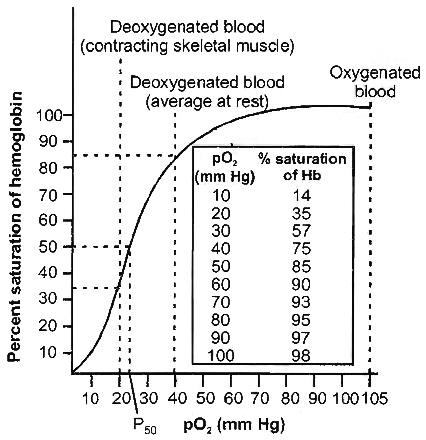
temperature showing the relationship between haemoglobin saturation and pO2
Myoglobin present in the muscles also has more affinity for O2. But since it has only one Fe2+ group, the curve obtained will be hyperbolic, not sigmoid.
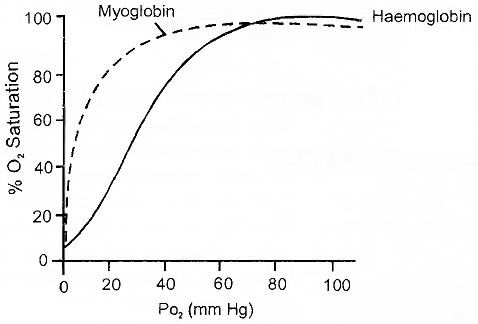
Dissociation curve for haemoglobin and myoglobin at 37°C, pCO2 40 mmHg and pH 7.
Concept Builder
1. Carbon Monoxide Poisoning:
If a person sleeps in a closed room with a lamp burning the absence of sufficient amount of oxygen causes an incomplete combustion of carbon and produces carbon monoxide in the room.
As the person inhales carbon monoxide, it diffuses from the alveolar air to the blood and binds to haemoglobin forming carboxyhaemoglobin.
The later is a relatively stable compound and cannot bind with oxygen.
So, the amount of haemoglobin available for oxygen transport is reduced.
The resulting deficiency of oxygen causes headache, dizziness, nausea and even death.
Carbon monoxide combines with haemoglobin at the same point on haemoglobin molecule as does oxygen.
It binds with haemoglobin 250 times faster than oxygen.
2. SARS (Severe Acute Respiratory Syndrome):
The first patient of SARS was reported on February 26, 2003 in China.
The causative agent is human Corona virus.
It is a new member of influenza virus family which is considered as a mutant form of influenza virus.
Carbon Dioxide Transport
CO2 is transported in three ways :
1. In dissolved State: About 7% of CO2 is transported after getting dissolved in plasma. The pCO2 in the arterial blood is 40 mm of Hg and in the venous blood, it is 45 mm of Hg. About 0.3 ml of extra CO2 is carried per 100 ml of blood in this form.
2. As Bicarbonate: Nearly 70% of CO2 is transported from tissues to lungs in this form. CO2 diffuses from tissues into the blood and enters RBCs. It combines with water to form H2CO3 which dissociates into H+ and HCO3–. Being catalysed by carbonic anhydrase, it is a very fast step.
![]()
H+ combine with hemoglobin replacing its association with K+ and form hemoglobinic acid.
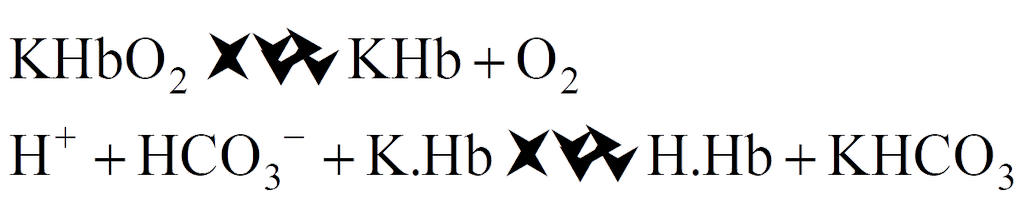
Due to it, the level of HCO3– increases in RBCs, which start coming out of it along the concentration gradient. To maintain ionic balance, Cl– move in from plasma into RBCs.
In the plasma HCO3– combine with Na+ or K+ to form NaHCO3 or KHCO3.
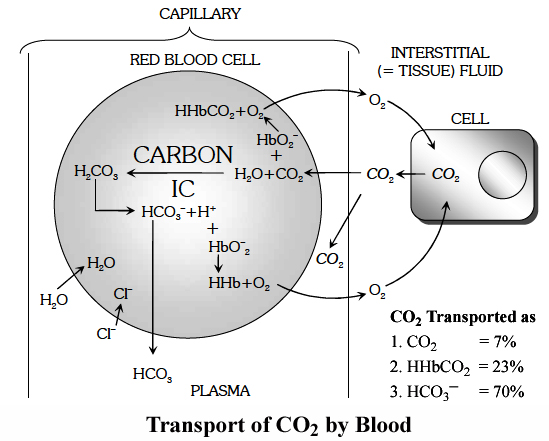
3. As Carbamino-Hb : About 20-25% of CO2 is transported in this mode. CO2 combines with NH2 group of Hb and forms carbamino-Hb. This combination of CO2 and Hb is a reversible reaction.
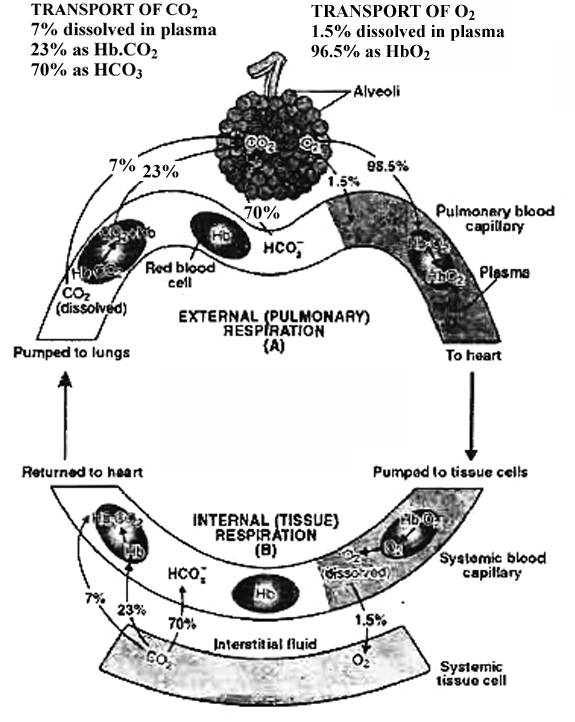
Release of CO2 in the alveoli of lung:
In the pulmonary capillaries, CO2 starts diffusing out into alveoli.
Carbamino-Hb spits into CO2 and Hb. As Hb of RBC takes up O2, it releases H+ in RBC.
The H+ start combining with the available HCO3– in RBC to form H2CO3 which splits into H2O + CO2 and CO2 starts diffusing out (Reverse of the reactions).
As a result HCO3– from plasma starts moving in along concentration gradient and for ionic balance; Cl– start moving out.
This way CO2 is released into lungs.
Hamburger's Phenomenon:
HCO3-ions diffuse out into plasma and Cl– ions enter into the RBCs at the level of tissues (intemal respiration). This is known as "chloride shift" or "Hamburger phenomenon". At the level of external respiration or alveoli, Cl– move out as HCO3– move in this is called reverse of chloride shift.
Haldane's Effect
It is related to the transport of CO2 in the blood. It is based on the simple fact that oxyhaemoglobin behaves as strong acid and releases an excess of H+ ions which bind with bicarbonate (HCO3–) ions to form H2CO3 which dissociates into H2O and CO2.
Secondly, due to the increased acidity, CO2 loses the power to combine with haemoglobin and form carbamino-haemoglobin.
Effect of oxyhaemoglobin formation or dissociation on CO2 transport is called Haldane's effect
Regulation of Respiration
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
Regulation of Respiration
Respiration may be defined as the process in which oxygen is taken inside the body from the environment for the oxidation of food to release energy and the carbon dioxide so produced during oxidation is expelled out of the body.
The process of oxidation of food is very complex.
It involves a series of complex biochemical reactions and the released energy is stored in the form of ATP molecules.
However, for simplicity sake, the multistep reaction can be briefly expressed as follows:
![]()
Types of Respiration
1. Direct and Indirect Respiration
(a) Direct Respiration:
There is direct exchange of gases between the carbon dioxide of the body cells and oxygen of water and there is no blood for the transport of gases.
Exchange of gases occurs on the principle of diffusion.
It is found in unicellular organisms like aerobic bacteria and protists (e.g. Amoeba) and metazoans like sponges, coelenterates (e.g. Hydra), flatworms, roundworms and insects.
(b) Indirect Respiration:
There is no direct contact between the body cells and the surrounding air or water the source of oxygen is called respiratory medium.
It is found in larger and complex forms of animals.
These organisms have some specialised organs; gills (most of crustaceans, molluscs, insect larvae, all fishes and amphibians); lungs (snails, amphibians, all reptiles, birds and mammals).
In this the transportation of oxygen and carbondioxide between the respiratory organs and the body cells is brought about by the blood of the Circulatory system.
2. All physical and chemical reactions in which atmospheric air oxidises food in the body cells resulting in production of energy and liberation of CO2 are included in respiration.
It is of following types:
(a) Anaerobic respiration:
It occurs when nutrients are oxidised without using O2 (also called fermentation).
In yeast, glucose forms ethyl alcohol and CO2, In bacteria and muscles, glucose is converted into lactic acid.
Endoparasites also respire anaerobically.
Anaerobic respiration is low energy yielding process.
In mature RBCs also anaerobic respiration occurs due to loss of mitochondria along with other cell organelles.
(b) Aerobic respiration:
Cells utilize O2 for oxidising nutrients.
O2 is used either from atmospheric air or from water.
It involves:
(i) External respiration: gaseous exchange between blood and air (or water) of O2 and CO2,
(ii) Transport of gases to the tissues.
(iii) Internal respiration : gas.eous exchange between blood and tissues.
(iv) Cellular respiration : oxidation of nutrients in the cells and liberation of energy.
Phases of Aerobic Respiration.
(i) External Respiration (Breathing or ventilation).
It is the exchange of oxygen of surrounding gaseous or liquid medium and carbon dioxide of blood through a liquid medium by diffusion across the body surface or the respiratory surface. It is purely a physical process which depends upon the principle of diffusion and no energy is produced.
(ii) Internal Respiration.
It is the exchange of oxygen of blood and carbon dioxide of the body cells through tissue fluid at the cellular level. Internal respiration involves the energy production and is a physico-chemical process.
(iii) Cellular Respiration:
It is utilisation of O2 by cells for energy production and resultant release of CO2,
Disorders of Respiratory System
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
Disorders of Respiratory System
Asthma is a difficulty in breathing causing wheezing due to inflammation of bronchi and bronchioles.
Emphysema is a chronic disorder in which alveolar walls are damaged due to which respiratory surface is decreased.
One of the major causes of this is cigarette smoking.
Occupational respiratory disorders:
In certain industries, especially those involving grinding or stone-breaking, so much dust is produced that the defense mechanism of the body cannot fully cope with the situation.
Long exposure can give rise to inflammation leading to fibrosis (proliferation of fibrous tissues) and thus causing serious lung damage.
Workers in such industries should wear protective masks.
Blood
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
BLOOD
Blood is a fluid connective tissue.
Its cells are quite distinct from other connective tissue cells both in structure and functions.
The extracellular material in blood is a fluid devoid of fibres.
Fluids outside the cells are generally called Extracellular Fluids (ECF).
Blood is heavier than water.
The extracellular material in blood is a straw-coloured, slightly alkaline (pH =7.4) aqueous fluid called plasma.
Constituents, having characteristic forms, float in the plasma.
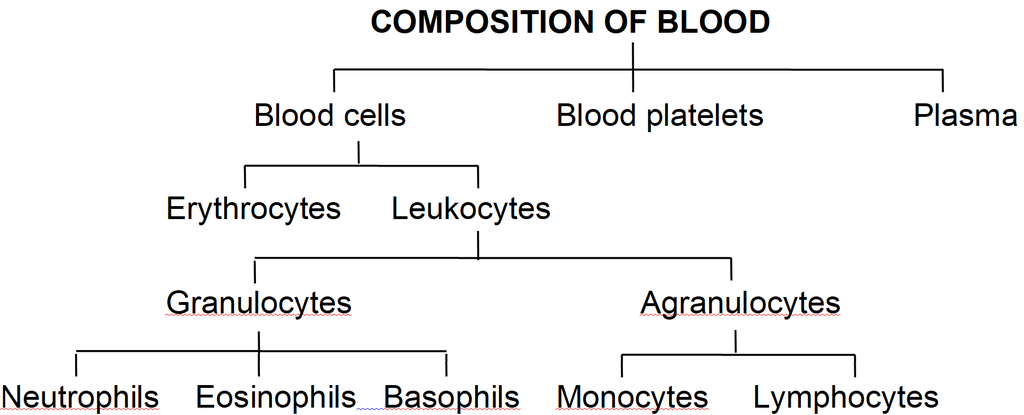
They are collectively called the Formed Elements of blood.
They include the blood cells and blood platelets.
Blood cells are of two types-Erythrocytes and Leukocytes.
Blood circulates within blood vessels in higher animals.
But other extracellular fluids such as cerebrospinal fluid, interstitial fluid, lymph and aqueous humour occur outside blood vessels.
PLASMA
Plasma contains three major classes of plasma proteins viz. serum albumin, serum globulins and fibrinogen.
Plasma proteins serve as a source of proteins for tissue cells.
Tissue cells may utilise plasma proteins for forming their cellular proteins.
Additionally, albumin and globulins retain water in blood plasma by their osmotic effects.
A fall in plasma proteins leads to movement of excessive volumes of water from blood to tissues.
That is why hands and feet get swollen with accumulated fluid (oedema) in persons suffering from dietary deficiency of proteins.
Albumins and globulins also transport many substances such as thyroxine and Fe3+ in combination with them.
One class of globulins, called immunoglobulins, act as Antibodies.
Plasma proteins also maintain the blood pH by neutralising strong acids and bases.
Thus, they act as Acid-Base-Buffers.
It is slightly alkaline non-living inter-cellular substance which constitutes about 60% part of the blood.
It is a pale yellow but transparent and clear fluid.
Composition of Plasma. Plasma forms 55-60% by volume of blood.
1.Water-Water alone forms about 90% to 92% of the plasma. Solids form about 8% of the plasma.
2.Mineral Salts -These are chlorides, bicarbonates, sulphates and phosphates of sodium, potassium, calcium, iron and magnesium. All salts constitute about 0.9% of plasma. Buffer of the blood is sodium bicarbonate.
3.Nutrients - These include glucose, fatty acids, phospholipids, cho'lesterol, fats, aminoacids, nucleosides, etc. Mineral salts have been mentioned above.
4.Plasma proteins -They constitute about 7 to 8% of plasma. These mainly include albumin 4.4% , globulin 1.5 to 2%, prothrombin and fibrinogen both 0.3%.
5.Defence proteins - Immunoglobulins which act as antibodies and some other substances, such as lysozyme and properdin (a large protein) are always found in the plasma. They destroy bacteria, viruses and toxic substances that may enter into the blood from outside.
6.Excretory substances - These include ammonia, urea, uric acid, creatinine, etc.
7.Dissolved gases - Water of blood plasma contains oxygen, carbon dioxide and nitrogen in dissolved form.
8.Anticoagulant - Blood plasma contains a conjugated polysaccharide, heparin which prevents coagulation of blood inside blood vessels.
9.Hormones - These are secreted and released in blood by endocrine glands.
10.Vitamins and Enzymes-Different kinds of vitamins and enzymes are present in the blood plasma.
Functions of Blood plasma-
These can be summarised as under (i) transport, (ii) retention of fluid in blood, (iii) maintenance of blood pH, (iv) body immunity, (v) prevention of blood loss, (vi) conducting heat to skin for dissipation and (vii) uniform distribution of heat all over the body.
Blood Glucose
Glucose is mainly absorbed in the small intestine.
Glucose is also absorbed in the stomach.
After absorption glucose reaches the blood.
Excess of glucose is converted into glycogen by insulin hormone in the liver and muscles.
Whenever it is required, glycogen is changed back into glucose by glucagon hormone.
Usually blood glucose level is about 80-100 mg per 100 ml of blood, 12 hours after a normal meal.
But its concentration rises soon after a carbohydrate rich diet.
If blood glucose level exceeds 180 mg per 100 ml, it starts appearing in urine.
This condition is called glucosuria.
Fasting glucose is 70 -110 mg/dl. Glucose PP1 is 110 -140 mg/dl.
If it is higher, it causes diabetes mellitus (hyperglycemia).
If it is less, it causes hypoglycemia (less amount of glucose in blood).
Blood Cholesterol
Usually cholesterol is considered a harmful substance. But it is quite useful in limited amount.
Cholesterol is used in the synthesis of biomembranes, vitamin D, bile salts and steroid hormones.
Its normal amount is 80 -180 mg in 100 ml of blood plasma.
Cholesterol comes in the blood plasma either by intestinal absorption of fats or by the synthesis from the liver or by both.
Saturated fats such as ghee and butter increase cholesterol level in the blood.
Increased blood cholesterol may lead to its deposition in the internal wall of the blood vessels like arteries and veins which causes high blood pressure and heart problems.
Functions of Plasma Proteins
1. Prevention of blood loss - Fibrinogen and prothrombin playa role in blood clotting.
2. Retention of fluid in the blood - Albumin helps in osmotic balance.
3. Body immunity - Certain globulins called immunoglobulins (glycoproteins) act as antibodies in blood and tissue fluid. Antibodies belong to a class of proteins called as immunoglobulins.
4. Maintenance of pH - Plasma proteins serve as acid-base buffers. It means they maintain pH of the blood by neutralizing acids and bases.
5. Transport of certain materials - Thyroxine (hormone) is bound to albumin or specific globulin for transport in the plasma.
6. Distribution of heat - Plasma proteins help in uniform distribution of heat all over the body.
7. Enzymes - Some proteins acting as enzymes also occur in the plasma.
BLOOD CELLS
(i) Erythrocytes:
Erythrocytes (red blood corpuscles or RBC) are the most numerous of the formed elements of blood.
Their most important characteristic feature is the presence of hemoglobin, the red oxygen carrying pigment.
The total number of erythrocytes per microlitre (1 µl = 1mm3 =10–6) of blood is known as the Total Count of RBC.
It averages 5 millions and 4.5 millions in adult man and adult woman respectively.
The total count would be low in anaemia and after profuse bleeding.
On the contrary, the abnormal rise in the total count of RBC is called Polycythemia.
Anaemia is caused due to the deficiency of folic acid, vitamin B12 and haemoglobin.
The size and shape of erythrocytes vary in different classes of animals.
In fishes, amphibians, reptiles and birds, erythrocytes are usually nucleated, oval and biconvex. But in mammals they are non nucleated, biconcave and circular.
Only camel and llama possess oval red blood corpuscles.
Human erythrocytes measure 7-8 µm (1µm =10–6 m) in diameter and 2 µm thickness near the rim.
Old and damaged erythrocytes are phagocytosed and destroyed by macrophages.
The pigment part (porphyrin) of hemoglobin is then catabolised to the yellow pigment Bilirubin which is excreted in the bile.
The pale yellow colour of plasma is largely due to bilirubin.
If a sample of blood is rendered non-coagulable by adding potassium or sodium oxalate and then centrifuged at a high speed in a graduated centrifuge tube (hematocrit tube), the centrifugal force rapidly sediments the erythrocytes tothe bottom of the tube.
They become packed into a solid, red, bottom layer while plasma forms a clear, fiuid upper layer.
On the upper surface of the erythrocyte layer, leukocytes form a thin, buff-coloured layer.
From the graduations on the tube, the relative volume of erythrocytes may be read as a percentage of the total blood volume. This is called the Hematocrit Value or Packed Cell Volume.
It normally forms 45 percent of the blood volume.
RBC of mammals are circular, biconcave, non-nucleated except family camelidae. e.g. camel, which has non-nucleated and oval RBC. Largest RBCs are found in amphibia.
Smallest RBCs are found in mammals.
In mammals smallest RBCs are found in 'Musk Deer', Tragulus javanicus (1.5 µm).
In mammals, largest RBCs are found in elephant. (9.4 µJ).
Graveyard of RBC is spleen.
Life Span
Life span of RBC in man =120 days
Life span of RBC in frog = 100 days
Life span of RBC of rabbit = 80 days
Radioactive chromium method (Cr51) is used for estimation of life span of RBC.
Count of RBC
In embryo = 8.5 million/mm3
In Man = 5 to 5.5 million/mm3
In Woman = 4.5 million/mm3
Daily destruction of RBC = 1%
ESR (Erythrocyte sedimentation rate) : It is measured by Wintrobe's method. It is rate of settling down of RBC.
It is also estimated by Westergen's method.
ESR is very useful in diagnosing various diseases including tuberculosis, ESR in men is 0-5 mm/hour and in women it is 0-7 mm/hr in Westergen method.
Haemocytometer: It is instrument for counting the number of both WBCs and RBCs.
Rouleaux: In resting and slow flowing blood, the RBCs aggregate to form rouleaux (the RBCs are piled on top of each other). Fibrinogen favours rouleaux formation.
Bone marrow: It is the main site for formation of RBC. Volume of bone marrow at the time of birth is 70 ml. In adult volume of bone marrow is 4,000 ml.
Structure of RBC of man: Biconcave non-nucleated bounded by Donnan's membrane (plasma membrane of RBC). Haemoglobin is filled in RBC which is respiratory pigment.
Normal Range of Hb
Infants 16.5 ± 3.0 g/dl (dl = deciliter)
Children 3 months 11.0 ± 1.5 g/dl
Children 3 to 6 years 12.0 ± 1.0 g/dl
Children 10 to 12 years 13.0 ± 1.5 g/dl
Men 15.5 ± 2.5 g/dl
Women 14.0 ± 2.5 g/dl
Structure of Haemoglobin:
Each molecule of haemoglobin contains 4 molecules of haem and 1 molecule of globin.
These are attached by co-ordinate bonds.
Haem is protoporphyrin compound and has 4 pyrrole groups jointed together to form ring structure.
In Hb, Fe is present in (Fe++) Ferrous form.
Haem is 5% & Globin is 95%. Globin is made of 4 polypeptide chains.
(ii) Leukocytes:
Leukocytes (white blood corpuscles or WBC) are devoid of hemoglobin and are consequently colourless.
Leukocytes are nucleated blood cells.
They are of two major classes : granulocytes (with cytoplasmic granules) and agranulocytes (without granules).
Granulocytes are of three types, viz. neutrophils, eosinophils and basophils, each with lobed nucleus.
Agranulocytesare of two types, viz. lymphocytes and monocytes.
Neutrophils and monocytes protect the body against microbes by phagocytosing them.
Lymphocytes secrete antibodies in the blood to destroy microbes and their toxins.
The number of leukocytes per microlitre (1 µl = 1 mm3 = 10–6) of blood is called the Total Count of WBC.
It is 6000-8000/mm3 of blood normally.
It may rise abnormally in acute infections (e.g., pneumonia), inflammations (e.g. appendicitis) and malignancies (e.g., leukemia).
In some conditions such as folic acid deficiency, the total count falls abnormally (leukopenia).
The total count of WBC is also of diagnostic value in many diseases.
Monocytes have kidney shaped nucleus.
The process by which monocytes and neutrophils squeeze out through thin capillary walls is Diapedesis.
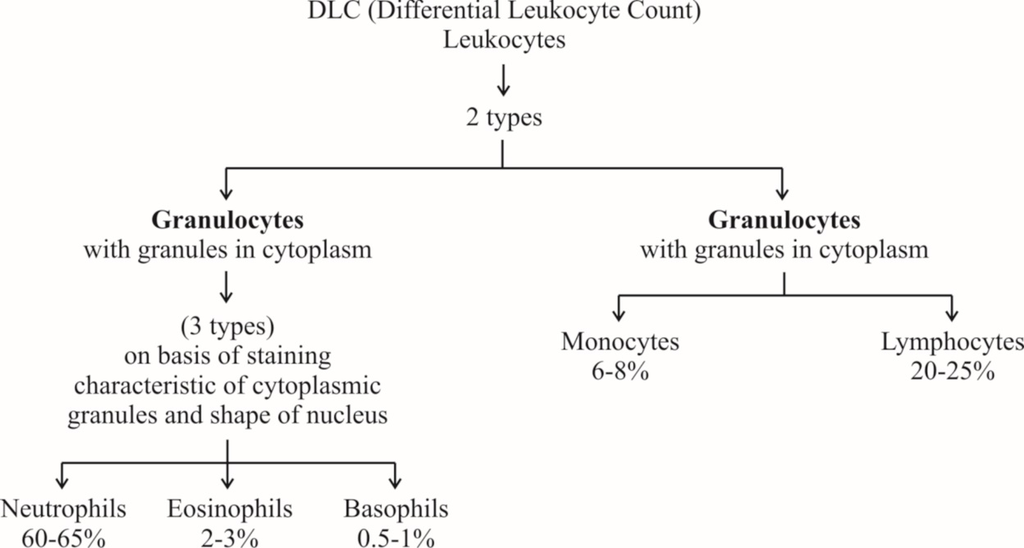
(a) Neutrophils: They are maximum in number, stain equally with both basic and acidic dyes and have many lobed nucleus, granules are in abundance in cytoplasm and help in phagocytosis.
(b) Eosinophils: They have bilobed nucleus, stain with acidic stains. Their number increases during allergic reactions (Eosinophilia).
(c) Basophils: They stain with basic dyes. Their nucleus is 'S' shaped. Coarse granules are few in the cytoplasm. Basophils release heparin and histamine in the blood and have a function similar to the mast cells.
(d) Lymphocytes have large and rounded nucleus. The cytoplasm forms a thin peripheral film. They have their stem cells in the bone marrow and are differentiated in the bone marrow or in the thymus. Lymphocytes are of two types, B-lymphocytes and T-lymphocytes.
B-lymphocytes produce antibodies against antigens and they mature in the bone marrow.
(e) Monocytes are the largest leucocytes (12-15 µm). The nucleus is kidney shaped. They are produced from bone marrow monoblast cells. They help in phagocytosis.
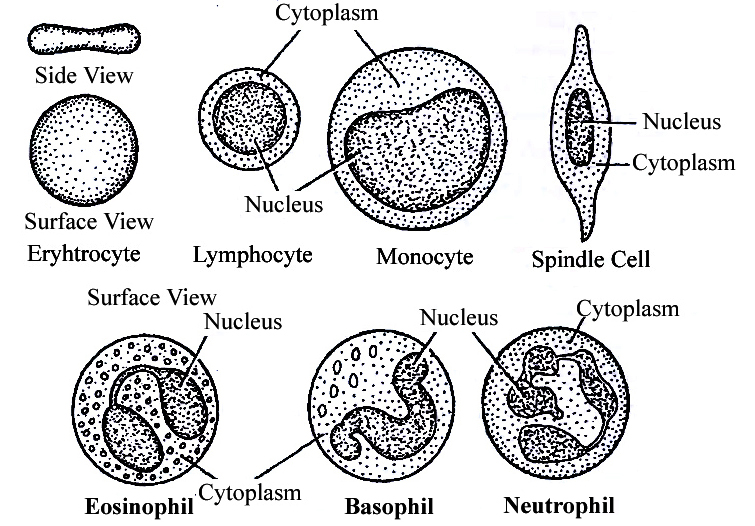
Table: Differences between different types of Leucocytes
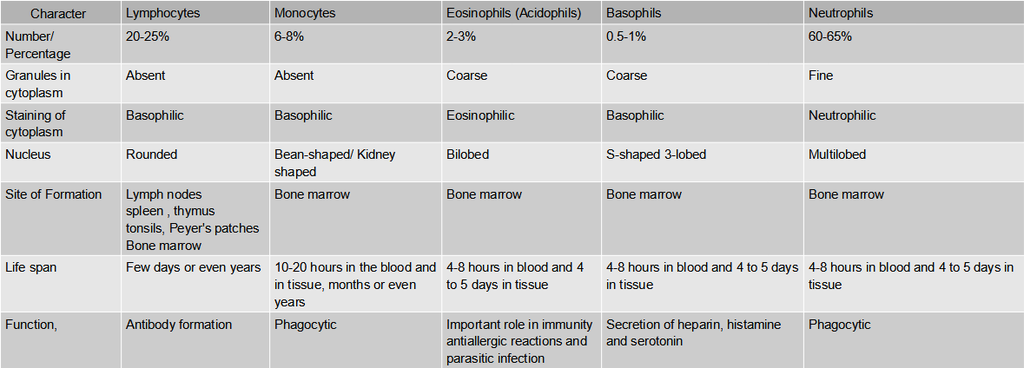
(iii) Blood platelets:
Also called thrombocytes, blood platelets are non-nucleated, round or oval, biconvex disc-like bodies.
They are 2-3 micrometres in diameter and their number normally varies from 0.15 to 0.35 million/mm3 or 150000 -350000 platelets/mm3.
They bud off from the cytoplasm of very large Megakaryocytes of the bone marrow.
Their normal life-span is about a week.
When a blood vessel is injured, platelets get clumped at the injured spot and release certain chemicals called Platelet Factors.
These promote blood coagulation.
Thrombocytopenia is decrease in platelet count and Purpura is a group of bleeding diseases due to thrombocytopenia.
BLOOD COAGULATION
When blood oozes out of a cut, it sets into gel within a few minutes. This is called coagulation.
Coagulation is brought about by hydrolysis of soluble fibrinogen of plasma to insoluble fibrin.
This is catalysed by an enzyme called thrombin.
Fibrin precipitates as a network of fibres.
This network traps many blood cells, particularly RBCs, to form a red solid mass called the Blood Clot.
The clot seals the wound in the vessel to stop the bleeding.
The straw coloured fluid left after clotting of blood, is called Serum.
The serum cannot be coagulated as it lacks fibrinogen.
Thrombin occurs in normal blood as an inactive globulin called Prothrombin.
It must be activated to thrombin before blood coagulation can occur.
In case of injury to a blood vessel, coagulation promoting substances called Thromboplastins are released into the blood from clumped platelets and damaged tissues.
Thromboplastins help in the formation of the enzyme Prothrombinase.
This enzyme hydrolyses prothrombin to thrombin to initiate coagulation.
Ca2+ ions are essential for both activation and action of thrombin.
Blood normally contains an anticoagulant, Heparin which prevents activation of prothrombin, Heparin is released from mast-cell granules.
Blood also contains Antithrombin which inhibits any thrombin formed accidentally.
Blood drawn from a blood vessel can be kept uncoagulated by adding a pinch of oxalate (sodium or potassium oxalate) to it.
Oxalate precipitates Ca2+ and consequently prevents coagulation.
Chilling of blood also delays coagulation because lesser temperature depresses the action of coagulation promoting enzymes.
ABO Blood cloting factor:
Karl Landsteiner reported for the first time ABO blood groups in human beings.
A. B and O blood groups were discovered by Landsteiner (1900) while AS blood group was found out by de Castello and Steini (1902).
Agglutinogens (antigens) are present on the surface of red blood corpuscles and agglutinins (antibodies) are found in the blood plasma. Both antigens and antibodies are proteins.
When two different type of blood are mixed, the red blood corpuscles form a clump.
The clumping of red blood corpuscles is called agglutination.
Clotting Factors:
13 factors help in blood clotting.
These factors are mainly produced in liver.
Vitamin K is required in the synthesis of these clotting factors.
These factors are represented in Roman number.
I – Fibrinogen
II – Prothrombin
III – Thromboplastin
IV – Ca+2 (cofactor in each step of blood clotting)
V – Proaccelerin
VI – Accelerin (Rejected)
VII – Proconvertein
VIII – AHG Anti Haemophelic Globin (Absent in Haemophilia-A)
IX – Christmas factor
X – Stuart factor
XI – PTA (Plasma Thormboplastin Anticedent)
XII – Hagman factor
XIII – FSF Factors (Fibrin stabilizing factor) (Laki Lor and factor).
Other natural anticoagulants are
Hirudin – found in leech.
Anophelin – found in female Anophelese.
Lampredin – found in Peteromyzon (Lamprey)
Cumerin – obtain from plants
Warfarin – obtain from plants
To collect blood in bottle in blood bank artificial anticoagulants are used like
Sodium citrate
Sodium oxalate
EDTA (Ethylene diamine tetra acetic acid)
These chemicals act as Calcium binding units and remove Ca+2 ions from blood.
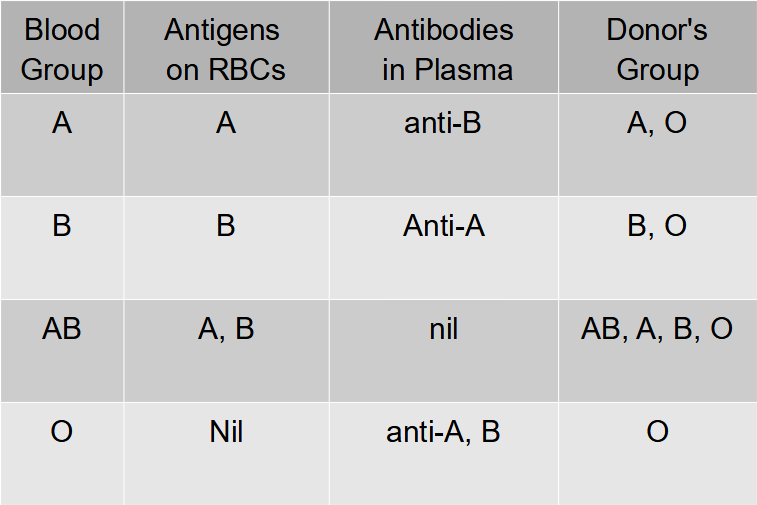
Blood group
Agglutination is due to the interaction of antigens and antibodies.
There are two kinds of antigens that are named A and B.
There are also two kinds of antibodies which are called a and b.
The antigen A and antibody a are incompatible (antagonistic) and cause self clumping and cannot exist together.
Similarly, the antigen B and antibody b are incompatible and cause self clumping and cannot exist together.
Thus, A and b can exist together and B and a can exist together.
The corpuscle factors A and B can occur together if their antagonistic plasma factors a and b are not present.
The plasma factors a and b can occur together if their antagonistic corpuscle factors A and B are absent.
Rh Factor
Another-antigen, the Rh antigen similar to one present in Rhesus monkeys (hence Rh), is also observed on the surface of RBCs of majority (nearly 80 per cent) of humans.
In India % ratio of Rh is
Rh+ – 97%
Rh– – 3%
In World
Rh+ – 80%
Rh– – 20%
Such individuals are called Rh Positive (Rh+ve) and those in whom this antigen is absent are called Rh negative (Rh-ve).
An Rh-ve person, if exposed to Rh+ve blood, will form specific antibodies against the Rh antigens.
Therefore, Rh group should also be matched before transfusions.
A special case of Rh incompatibility (mismatching) has been observed between the Rh-ve blood of a pregnant mother with Rh+ve blood of the foetus.
Rh antigens of the foetus do not get exposed to the Rh-ve blood of the mother in the first pregnancy as the two bloods are well separated by the placenta.
However, during the delivery of the first child, there is a possibility of exposure of the maternal blood to small amounts of the Rh+ve blood from the foetus.
In such cases, the mother starts preparing antibodies against Rh antigen in her blood. In case of her subsequent pregnancies, the Rh antibodies from the mother (Rh-ve) can leak into the blood of the foetus (Rh + ve) and destroy the foetal RBCs.
This could be fatal to the foetus or could cause severe anaemia and jaundice to the baby.
This condition is called erythroblastosis foetalis.
This can be avoided by administering anti-Rh antibodies to the mother immediately after the delivery of the first child.
Lymph (Tissue Fluid)
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
LYMPHATIC SYSTEM
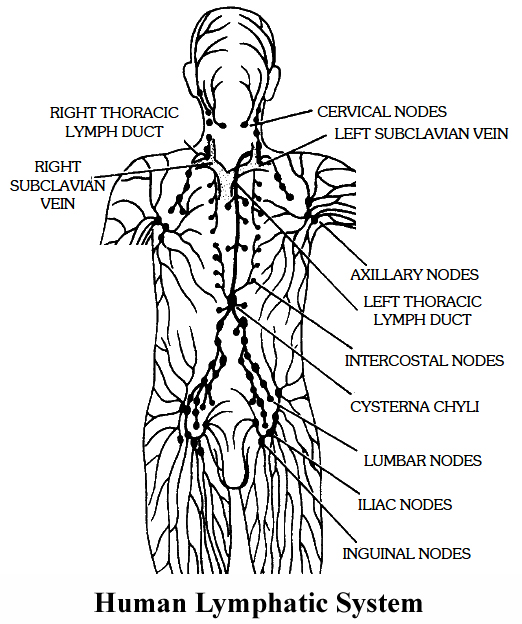
It comprises of lymph, lymphatic capillaries, lymphatic vessels, lymphatic ducts and 'lymphatic nodes.
1. Lymphatic capillaries: They lie close to the blood capillaries but end blindly. They have extremely thin walls. They are composed of a single layer of endothelial cells.
2. Lymphatic vessels : The lymphatic capillaries unite to form larger lymphatic vessels. They are composed of an outer coat of fibrous tissue, middle coat of muscular tissue and an inner lining of endothelial cells. The lymphatic vessels have numerous valves. The lymph vessels of intestinal regions absorb the digested fats. They are milky in appearance and are called lacteals (Iaetos : milk).
3. Thoracic duct: The lymphatic vessel of left side begins at the cisterna chyli , present at the level of (anterior to) the first and second lumbar vertebrae. It discharges its lymph into the left subclavian vein.
4. Right lymphatic duct: The lymphatic vessels of the right side of the thorax, head and neck unite to form the right lymphatic duct. It discharges its lymph into the right subclavian vein .
5. Lymphatic nodes: The lymphatic vessels bear lymph nodes at intervals and are abundant in the neck, armpit and groin. The lymph is filtered through lymph nodes which contain phagocytic white blood corpuscles and macro phages which eat harmful microorganisms and foreign particles from the lymph. Lymph nodes also add lymphocytes and antibodies.
Lymph Movement: The lymph flows slowly and moves from lymphatic vessels, lymphatic ducts to the venous system. Blocking of lymph flow causes oedema.
Lymphoid Organs : The organs which secrete lymph are called lymphoid organs. Besides the lymph nodes, tonsils, thymus gland, Peyer's patches, liver and spleen are the other lymphoid organs that secrete lymph.
Functions of Lymph
1. Lymph acts as a "middle man" which transports various proteins, hormones, etc., to the body cells and brings carbon dioxide and other metabolic wastes, from the body cells and finally pours the same into the venous system.
2. Lymph nodes produce lymphocytes. Lymph takes lymphocytes and antibodies from the lymph nodes to the blood.
3. It absorbs and transports fat and fat soluble vitamins from the intestine. Lymph capillaries present in the intestinal villi are called lacteals which are associated with absorption and transportation of fat and fat soluble vitamins.
4. It brings plasma protein macromolecules synthesized in the liver cells and hormones produced, in the endocrine glands to the blood. These molecules can not pass into the narrow blood capillaries but can diffuse into the lymphatic capillaries.
5. Lymph maintains the volume of the blood. As soon as the volume of the blood reduces in the blood vascular system, the lymph rushes from the lymphatic system to the blood vascular system.
Circulatory Pathways
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
BLOOD VESSELS AND COURSE OF CIRCULATION OF BLOOD
Arterioles:
Arterioles are small arteries that deliver blood to capillaries. Arterioles also have smooth muscles on their walls.
Contraction and relaxation of these muscles alter the diameter of arterioles and thereby respectively reduce and increase the blood flow through them.
Capillaries:
Capillaries were discovered by Malpighi in 1661.
Capillaries are the smallest blood vessels in the body.
Capillary has no muscular wall.
Its wall is made of a single layer of flat endothelial cells and is consequently very permeable to water and small solutes, but not to proteins and other macromolecules.
The diameter of lumen of capillaries is from 7.5 µm to 75 µm. Only about 5 to 7% of the total volume of blood is contained in the capillaries.
Venules:
Venules are small vessels that continue from capillaries and merge to form veins. They drain blood from capillaries into veins.
Veins:
Veins have less elastic tissue and smooth muscle than arteries.
One major difference between an artery and vein is that vein has a thin muscular wall.
Veins contain valves to prevent backflow of blood.
Valves are necessary in veins but not in arteries because pressure in veins is low to push the blood.
Weak valves can lead to varicose veins or haemorrhoids.
All veins carry deoxygenated blood except pulmonary veins.
Pulmonary veins carry oxygenated blood from lungs back to heart.
Blood vessels that carry blood from lungs to heart are called pulmonary veins.
Wall of veins is collapsible (non collapsible in arteries).
Lumen of vein is wider and narrow than arteries.
Most veins are located close to skin (deep in body in case of arteries).
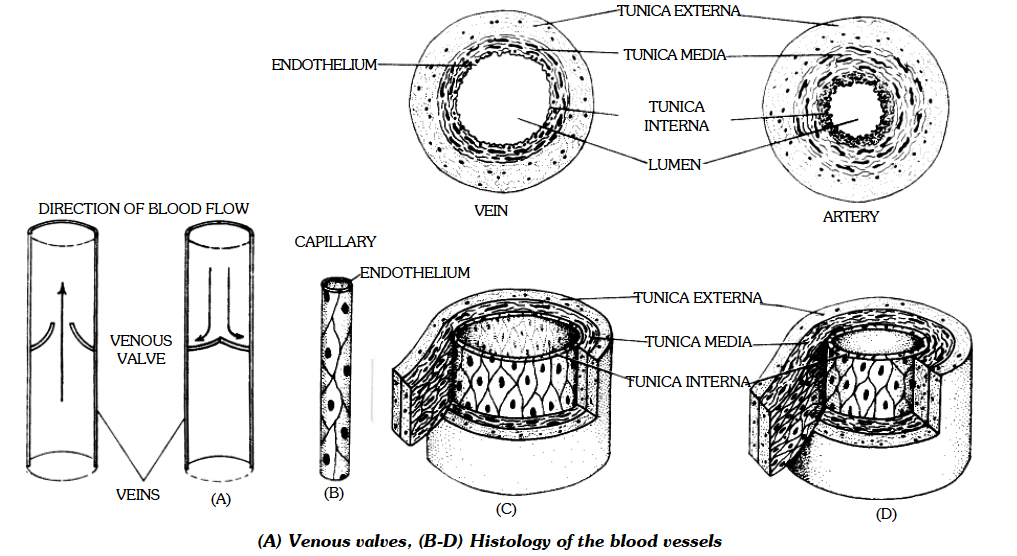
Vasa Vasorum : Blood vessels which supply blood to blood vessel are 'vasa vasorum'.
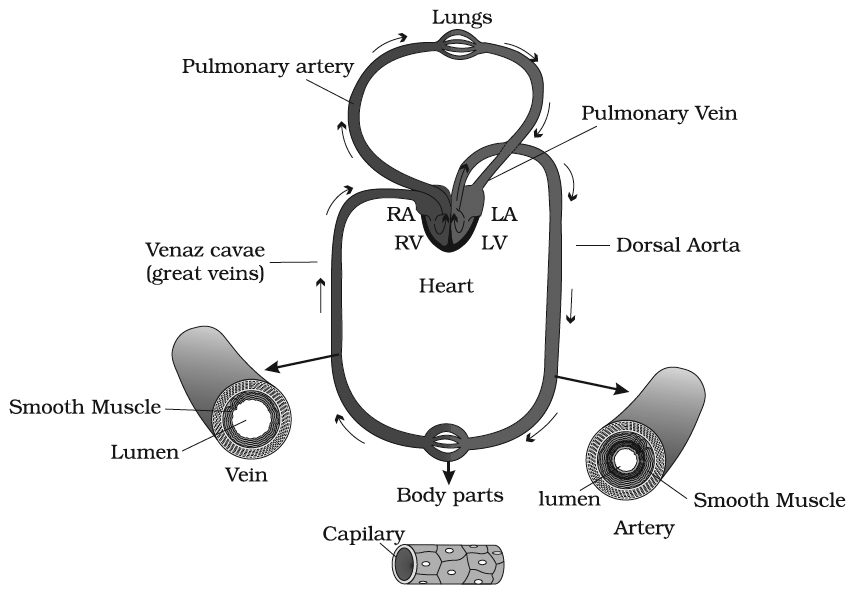
Course of Circulation of Blood
There are three types of circulation :
(a) Pulmonary circulation: from heart to the lungs and back.
(b) Systemic circulation: when blood is passed to different parts of the body.
(c) Portal circulation

Regulation of Cardiac Activity
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
Heart Beat: Regulation
Normal activities of the heart are regulated intrinsically, i.e., auto regulated by specialised muscles (nodal tissue), hence the heart is called myogenic.
A special neural centre in the medulla oblangata can moderate the cardiac function through autonomic nervous system (ANS).
Neural signals through the sympathetic nerves (part of ANS) can increase the rate of heart beat, the strength of ventricular contraction and thereby the cardiac output.
On the other hand, parasympathetic neural signals (another component of ANS) decrease the rate of heart beat, speed of conduction of action potential and thereby the cardiac output.
This happens because these nerves release chemicals (hormones) when stimulated. Adrenal medullary hormones can also increase the cardiac output.
(i) High levels of potassium and sodium ions decrease heart rate and strength of contraction.
(ii) An excess of calcium ions increases heart rate.
(iii) Increased body temperature during fever increases heart rate.
(iv) Strong emotions such as fear, anger and anxiety increase heart rate, resulting in increased blood pressure.
(v) Mental states such as depression and grief decrease heart rate.
(vi) The heart beat is somewhat faster in females.
(vii) The heart beat is fastest at birth, moderately fast in youth, average in adulthood and above average in old age.
Heart Sounds
These are caused due to sudden closure of the valves of heart. There are mainly two sounds.
(i) First Sound : Occurs at the onset of ventricular systole and is caused due to the sudden closure of AV valves and the ejection of blood from the ventricles. It is dull and pronounced as L -U -B.
(ii) Second Sound : Occurs at the onset of ventricular diastole and is caused by sudden closure of the semilunar valves of the aorta and pulmonary artery.
It is short and sharp like the word D -U -P.
The sequence of both these sounds is like this : first sound ® second sound ® pause; first sound ® second sound ® pause; so on. Sometimes if damage occurs as in rheumatic fever, blood may leak out through the valrves and a characteristic sound mur-mur is produced.
Pulse Rate
The blood is pumped from the ventricles of the heart into the aorta to be distributed to all the parts of the body.
This happens during the ventricular systole and is repeated after every 0.8 seconds.
The blood from aorta then goes to other arteries of the body.
This causes a rhythmic contraction of the aorta and its main arteries and is felt as regular jerks or pulse in them.
It can be felt in the regions where arteries are present superficially like wrist, neck and temples.
The pulse rate is, therefore, same as that of heart beat rate.
Electrocardiogram (ECG)
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
ECG (ELECTROCARDIOGRAM)
Electric changes of the cardiac chambers follow a specific sequence.
These changes can be recorded with the help of an apparatus-electrocardiograph.
The record is called ECG.
It is represented as PQRST; where P = depolarisation of atria; QRS = depolarisation of ventricles and T = repolarisation of ventricles.
Defects in cardiac function or structure are recorded in the ECG.
For the purpose of recording, metal electrodes or leads are attached in each arm and leg with the help of straps after cleaning and putting a special jelly, which improves electrical conduction.
An additional electrode is placed on the chest with the help of a rubber suction cup.
Then, the electrocardiograph is switched on.
The electrical current of the heart is detected and amplified by the machine and is transmitted to the recording pen that draws a wavy line, called the deflection waves (electrocardiogram).
A normal electrocardiogram is composed of a P wave, a QRS complex and a T wave.
The QRS complex has three separate Q, Rand S waves.
The P wave is a small upward wave that indicates the depolarisation of the atria or the spread of impulse from the sinus node throughout the atria.
The second wave, i.e., the QRS complex, begins after a fraction of a second of the P wave.
It begins as a small downward deflection (Q) and continues as large upright (R) and triangular wave, ending as downward wave (S) at the base.
This is the expression of the ventricular depolarisation.
The potential generated by the recovery of ventricle from the depolarisation state is called the repolarisation wave.
In electrocardiography, P-Q interval (also called PR interval) is the time taken by the impulse to travel through atria, AV node and the rest of the conducting tissues.
During rheumatic fever and in arteriosclerotic heart disease (i.e., the formation of plaques and calcification), the P-Q interval lengthens.
This is due to the inflammation of atria and atrioventricular node.
The normal PR interval lasts for 0.16 second.
The enlarged Q and R waves are the indication of myocardial infarction.
The ST intervai is the representation of time between the end of the spread of impulse through ventricles and its repolarisation.
The S-T segment is elevated in acute myocardial infarction and depressed in a condition when the heart muscles receive insufficient oxygen.
The ventricular repolarisation is represented as T wave.
When the heart muscles receive insufficient oxygen, then the T wave is flattened.
Disorders of Circulatory System
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
Disorders of Circulatory System
High Blood Pressure (Hypertension):
Hypertension is the term for blood pressure that is higher than normal (120/80).
In this measurement, 120 mm Hg (millimetres of mercury pressure) is the systolic, or pumping, pressure and 80 mm Hg is the diastolic, or resting, pressure.
If repeated checks of blood pressure of an individual is 140/90 (140 over 90) or higher, it shows hypertension.
High blood pressure leads to heart diseases and also affects vital organs like brain and kidney.
Coronary Artery Disease (CAD):
Coronary Artery Disease, often referred to as atherosclerosis, affects the vessels that supply blood to the heart muscle.
It is caused by deposits of calcium, fat, cholesterol and fibrous tissues, which makes the lumen of arteries narrower.
Angina:
It is also called 'angina pectoris'.
A symptom of acute chest pain appears when no enough oxygen is reaching the heart muscle.
Angina can occur in men and women of any age but it is more common among the middle-aged and elderly.
It occurs due to conditions that affect the blood flow.
Heart Failure:
Heart failure means the state of heart when it is not pumping blood effectively enough to meet the needs of the body.
It is sometimes called congestive heart failure because congestion of the lungs is one of the main symptoms of this disease.
Heart failure is not the same as cardiac arrest (when the heart stops beating) or a heart attack (when the heart muscle is suddenly damaged by an inadequate blood supply).
Concept Builder
1. Lowest level of glucose is in hepatic vein.
2. Highest levels of amino acids are present In hepatic vein.
3. Highest level of urea is in hepatic vein and towest in renal vein.
4. Largest vein in human body-Inferior vena cava.
5. Largest Artery-Aorta.
6. Smallest blood vessel in the body-Blood capillary.
7. The giraffe's blood pressure may be the highest of all animals because it has to pump the blood to the head through long neck.
8. One species of Antarctic fish is the only fish known to have white blood. It has no red pigment in its blood.
9. Frog has two pairs of lymph hearts to pump lymph back into veins.
10. Thrombopenia: Decrease in biood platelet count.
11. Erythropoietin: Hormone secreted by the juxta-glomerular cells of the kidneys.
12. Circulatory shunts in foetus.
Foetus bypasses pulmonary system through two shunts-foramen ova Ie (opening in interatrial septum) and ductus arteriosus (connection between dorsal aorta and pulmonary arCh). Shunts are sealed after birth.
13. Lung fish has 3 chambered heart: two auricles and one ventricle.
14. Crocodiles, alligators and gavialis have four chambered heart (two auricles and two ventricles).
15. The heart of fish is called venous heart because it receives and pumps deoxygenated blood.
16. In human heart, auricles are called atria (Sing. atrium).
17. Nereis and Amphioxus do not have heart. Heart of prawn contains oxygenated blood.
18. There is single blood circulation in fish heart. Hearts of amphibians, reptiles, birds and mammals have double blood circulation. Foramen of Panizzae is present in between two systemic arches (they arise from the heart) of the heart of lizard and crocodiles. Average human heart is about 12 cm. Average weight of human heart-male 300g, female 250 g. The opening of the coronary sinus into the right atrium is guarded by Thebesian valve. The opening of inferior vena cava into the fight atrium has I:ustachian valve. Fossa ovalis is a depression on the interatrial septum.
19. Coronary angiography : When the contrast medium dye is injected in coronary arteries (arteries of heart) and pictures are taken, it is known as coronary angiography.
20. Excess calcium ions cause increased heart beat.
21. RBCs fail to mature if there is a deficiency of vitamin B12 and folic acid.
22. Papillary muscles are found in heart of mammals.
23. Keber's organs or pericardial glands discharge excretory products into the pericardial cavity in the fresh water mussel.
24. A "Blue baby" is the name given to an abnormal human baby who has a hole in the auricular or ventricular septum so that oxygenated and deoxygenated blood mixing take place.
25. An insect larva has red blood. The larva of genus Chironomusis called 'Blood worm'. The red colour of this larva is due to haemoglobin, which has the power of attracting and storing oxygen and giving it off to the tissues as they require it. Such larva are able to live in burrows constructed by it in the mud.
26. Vasa Vasorum are blood vessels which supply blood to the blood vessels itself.
27. Blue Whale has the largest heart.
28. Cardiomegaly is heart enlargement.
29. Angiology: Study of blood vascular and lymphatic systems.
30. Venoms of Bee and Cobra contain lecithinases which when injected into the blood stream by sting or bite break down lecithins and produce lysolecithins which in turn cause rupturing of RBC cell-membrane (cell-lysis).
31. Marey's law: Heart rate is inversely related to the systemic B.P.
Human Excretory System
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
HUMAN EXCRETORY SYSTEM
1. In humans, the excretory system consists of a pair of kidneys, one pair of ureters, a urinary bladder and a urethra.
Kidneys: Kidneys are reddish brown, bean shaped structures situated between the level of last thoracic and 3rd Lumbar vertebra close to the dorsal inner wall of the abdominal cavity. Each kidney measures about 10 -12 cm long, 5 -7 cm in width and 2 -3 cm thick. It weighs about 120 -170 g in adults. Left kidney is little higher than the right one because of more space being occupied by the liver on right side.
2. Towards the centre of the inner concave surface of the kidney is a notch called hilum through which ureter, blood vessel and nerve enters. Inner to the hilum is a broad funnel shaped space called the renal pelvis.
Kidney is covered by 3 protective layers which are as foillows :
1. Renal Capsule: It is innermost, tough protective cover made up of white fibrous connective tissue, with few elastic fibres and few muscles.
2. Adipose Capsule: It is the middle cover involving adipose tissue and acts as shock absorber.
3. Renal Fascia: It is the outermost fibrous cover linking it with the abdominal wall.
As the kidneys are fused with the body wall on the dorsal side, peritoneal cover is present only on the ventral side. This arrangement is called Retroperitoneal arrangement.
Internal Structure of Kidney
A longitudinal section of the kidney shows two functional layers, outer renal cortex and inner renal medulla.
(a) Renal Cortex: It is the outer part which is dark in colour and granular in nature.
(b) Renal Medulla : It is the inner part which is lighter in colour and striated in nature. Medulla has 8 -18 conical renal pyramids. They actually represent multilobular condition of foetal kidney.
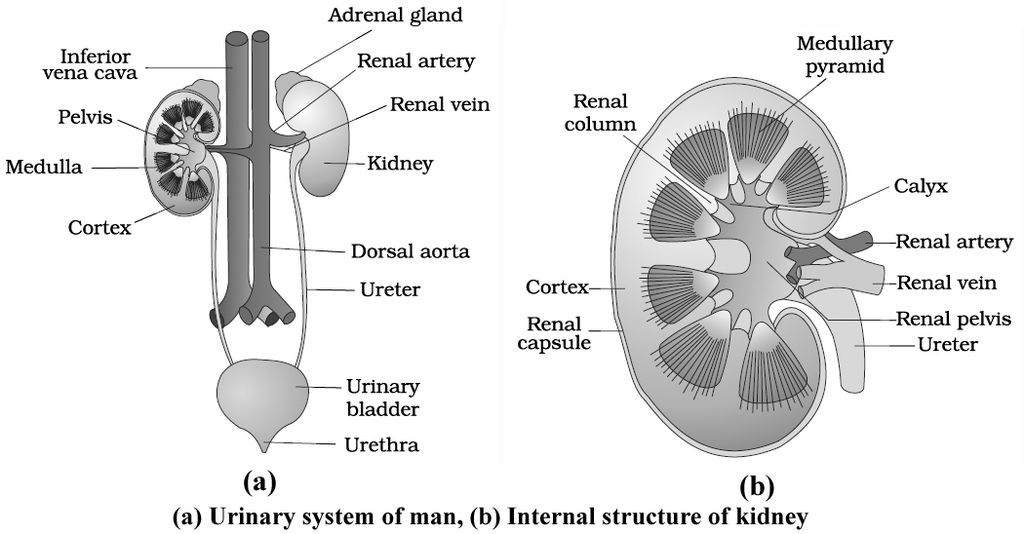
Each renal pyramid has a broad base towards the cortical side. Apex is pointed and is called renal papilla.
1-3 renal papillae project into a activity called minor calyx, which join up and form major calyces.
Cortex projects into medulla in the regions in between the pyramids and calyces, called renal columns of Bertini.
Interstitial fluid of medulla region has a higher osmotic concentration equal to some 1200 mosm/lt. due to higher quantity of two solutes, NaCl and urea.
Cortical region close to medulla is called juxtamedullary area.
The major calyces open into a broad funnel-shaped structure called renal pelvis placed inner to hilum.
It is lined by transitional epithelium.
It leads into ureter.
Structural and functional units of kidney are called nephrons or uriniferous tubules.
There are about 1 million nephrons in each kidney.
The number of uriniferous tubules decreases with age.
Ureters:
They are a pair of fine whitish distensible muscular tubes of 25 -30 cm length, about 3 mm in diameter.
Ureters develop from hilum part of the kidneys, descend along the abdominal wall, bend obliquely inwards and upwards to open in to urinary bladder in the region of trigone by oblique slits, one on each side.
Wall of ureter has 3 coats -extemal adventitia, middle muscular and inner mucosa, Muscular coat has three layers of smooth muscle fibres -outer longitudinal, middle circular and inner longitudinal.
Ureters are always undergoing peristalsis which helps in passing urine from kidney to urinary bladder.
Urinary Bladder:
It is a median pyriform sac which varies in shape, size and position according to the amount of urine contained in it.
The fully distended bladder becomes ovoid in outline.
Bladder has three parts -apex, fundus or body and neck. Body has a triangular area called trigone.
It has openings of ureters and an internal urethral orifice.
Neck region possesses two sphincters, involuntary internal sphincter and voluntary external sphincter.
Neck leads into urethra.
Wall of urinary bladder consists of three coats -outer adventitia, middle muscular and inner mucosa.
The muscle present in the middle muscular coat is also called detrusor muscle because it takes part in detrusion or pushing down of urine.
Muscular coat has involuntary circular muscles in the middle and involuntary longitudinal muscles on its either side.
Mucosa has loose connective tissue towards the side of muscular layer and transitional epithelium or urothelium towards lumen.
Adventitia is formed of soft connective tissue.
During the micturition, both the sphincters undergo relaxation.
Cerebral cortex direct the sphincter to relax and person undergoes urination.
Wall of urinary bladder is innervated by both sympathetic and parasympathetic nervous system.
Urethra:
It is present only in mammals. It starts from the neck of the urinary bladder and opens outside the body.
In female, it is short (2-4 cm), straight and concerned with the release of urine through an aperture called urethral orifice or urinary aperture present in the vulva in front of the vaginal aperture.
However, in male, it is quite long (20 cm), passes through the ejaculatory duct, prostate gland, cowper's glands and penis.
It is concerned with the release of urine as well as semen (sperms + glandular secretion) through an aperture called urinogenital aperture at the tip of the penis.
Blood Supply to Kidney
A renal artery enters each kidney and divides into many afferent arterioles which enter the Bowman's capsules and sub-divide to form glomerulus.
The glomerular capillaries rejoin to form efferent arteriole.
Efferent arteriole is narrower than afferent arteriole.
This raises blood pressure inside glomerulus.
Efferent arteriole further forms numerous peritubular capillaries in the cortex region around the proximal and distal convoluted tubules of the nephron.
It further forms vasa recta around the loop of Henle.
Blood from the vasa recta is released into the renal venule from where it escapes into renal vein.
Urine Formation
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
URINE FORMATION
Nephric excretion involves the formation of urine. Urine formation occurs in three steps -glomerular filtration, tubular reabsorption and tubular secretion.
1. Glomerular Filtration (Ultrafiltration):
Blood present in the glomerular 'capillaries is separated from the capsular space of Bowman's capsule by
(i) Endothelial covering of blood vessels.
(ii) Basement membrane of blood vessel.
(iii) Basement membrane of visceral layer
(iv) Visceral layer or inner wall of Bowman's capsule.
Therefore, the actual barrier between blood and capsular space consists of two basement membranes which are, however, permeable to small sized molecules.
Development of Filtration Pressure:
Blood flows through glomerular capillaries under a pressure.
The pressure is due to two reasons:
(i) Wider diameter of afferent arteriole as compared to diameter of efferent arteriole.
(ii) Natural arterial pressure caused by pumping activity of heart. Blood pressure in glomerular blood is about 60 mm Hg, this is called glomerular hydrostatic pressure (GHP). Osmotic concentration of proteinaceous content of glomerular blood is equivalent to 30 mm Hg, this is called blood colloidal osmotic pressure (BCOP). Pressure of interstitial fluid and pressure of renal filtrate is collectively called capsular hydrostatic pressure (CHP =20 mmHg). The pressure being exerted on glomerular blood for undergoing filtration is called glomerular filtration pressure (GFP). It is about 10 mm Hg.
or, GFP = GHP -(BCOP + CHP)
= 60 – (30 + 20) = 10 mmHg
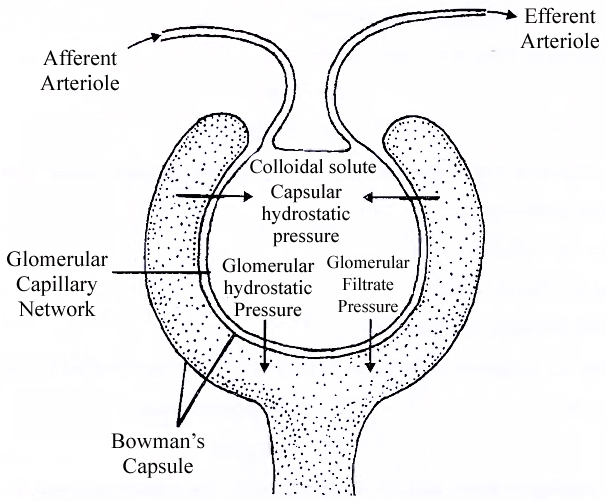
Ultrafiltration:
As there is net higher hydrostatic pressure of 10 mm Hg in the lumen of glomerular capillaries as compared to lumen of Bowman's Capsule, the filterable components of blood are passed out of the glomerular capillaries.
They pass through endothelial fenestrations, basement membranes and filtration slits of podocytes to enter the lumen of Bowman's capsule.
The phenomenon is called nephric or glomerular filtration.
About 1100-1200 ml of blood is put to filtration in the two kidneys every minute which constitutes roughly 1/5th of the blood pumped out by each ventricle of the heart in a minute.
It produces a glomerular or nephric filtrate of about 125 ml/min or 180 Uday.
The rate of filtration is called glomerular filtration rate or GFR.
Nephric filtrate consists of water, various electrolytes (Na+, K+, Ca2+, Mg2+, K+, PO43–), glucose, amino acids, hormones, vitamins, urea, creatinine, uric acid etc.
It is alkaline like blood but excludes large sized particles and structures like fats, proteins, platelets, leucocytes and erythrocytes.
Separation of small volume solutes from large volume solutes and components due to filtration through small sized pores or slits by the application of pressure is called ultrafiltration.
Autoregulation of Glomerular Filtration:
There are three methods by which renal blood flow and glomerular filtration rate (GFR) are automatically regulated.
(a) Myogenic Autoregulation:
A rise in blood pressure should normally increase blood flow through glomeruli.
However, stretching of the vascular wall increases passage of Ca2+ ions from extracellular fluid into the cells resulting in their contraction.
Contraction checks overstretching of vascular walls and raises vascular resistance so that rate of blood flow and GFR are brought down to normal.
(b) Juxtaglomerular Apparatus (JGA):
The apparatus becomes active when there is decrease in renal blood pressure or decrease in glomerular filtration rate (GFR).
It promotes release of renin from Juxta-glomerular cells.
Renin converts protein angiotensinogen into peptide angiotensin.
Angiotensin is a hormone that raises glomerular blood pressure through constricting efferent arterioles resulting in restoring GFR.
It also brings about release of aldosterone.
(c) Neural Control:
Blood vessels of the kidney are innervated by nerve fibres of the sympathetic nervous system.
When activated, the nerve fibres bring about constriction of renal arteries and cause decrease in renal blood flow as well as glomerular filtration rate.
Functions of the Tubules
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
Functions of the Tubules
Types of Nephron
A kidney has two types of nephrons-cortical and juxtamedullary. They are held together with the help of connective tissue
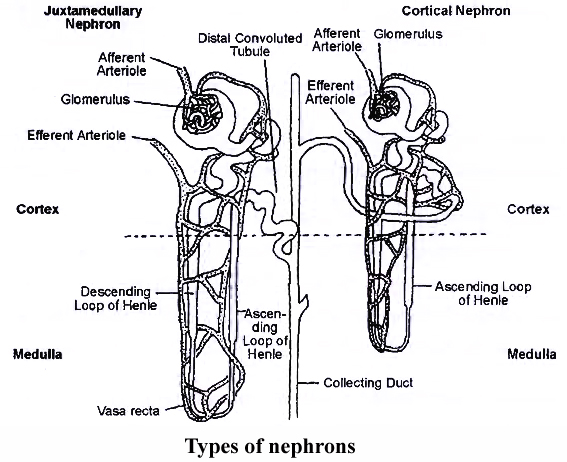
(a) Cortical Nephrons:
They constitute about 85%, of the total nephrons.
Cortical nephrons are smaller in size with major part lying in the cortex.
The tubule is much coiled.
Loop of Henle is short and extends into medulla to a short distance.
Vasa recta are absent or highly reduced.
Glomeruli lie in the outer cortex.
(b) Juxtamedullary Nephrons:
They are approximately 15% of the total and are present at the junction of cortex and medulla region of kidney.
They have large size, less coiling and a long loop of Henle.
Glomeruli occur in the inner cortex.
The long loops of Henle placed deep in the medulla.
Vasa recta occur over the loops of Henle.
Juxtamedullary nephrons become active during shortage of water.
They increase water reabsorption and, therefore, control the volume of plasma.
The system usually works under stress conditions.
Structure of Nephron (Renal Tubule, Uriniferous Tubule)
Nephron or uriniferous tubule is the structural and functional unit of kidney.
It is about 3 cm long and 20-60 mm in diameter. Each nephron consists of two parts -Glomerulus and renal tubule (Bowman's capsule, PCT, Henle's loop and DCT)
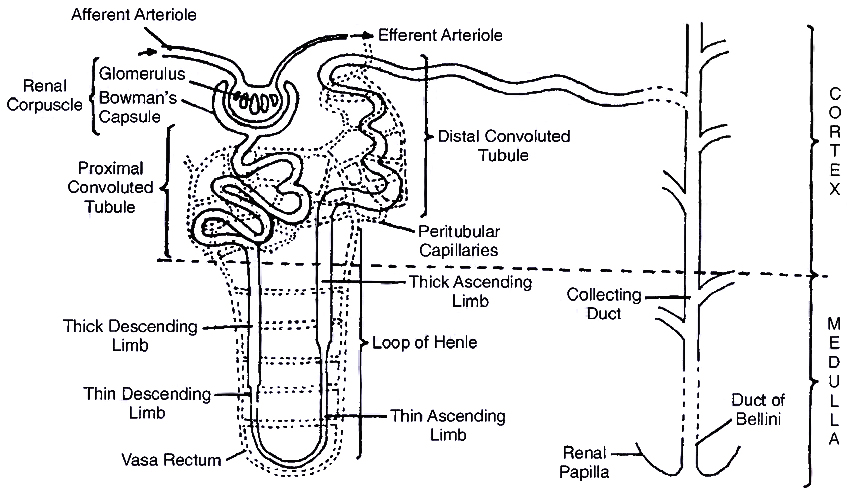
1. Bowman's Capsule:
It is blind double walled cup-shaped structure. The two walls of Bowman's capsule are inner visceral and outer parietal. Both are single layered and are supported over basement membrane.
(i) Visceral Layer (Inner Wall):
It consists of flat squamous epithelial cells on the periphery and specialised podocytes in the remaining part.
A podocyte has a number of interdigitated evaginations called pedicels or feet.
The pedicels rest over the basement membrane.
They enclose slit pores or filtration slits.
The diameter of these slits is about 25 nm.
Pedicels also possess contractile filaments which help in passage of filtrate through the filtration slits.
(ii) Parietal Layer (Outer Wall):
It consists of flat squamous epithelium.
The space between the two layers of Bowman's capsule is called lumen or capsular space.
Glomerulus:
It is a tuft of capillaries formed by fine blood vessels lying in the Bowman's capsule.
Glomerulus receives blood from an afferent arteriole.
Blood is taken away from the glomerulus by an efferent arteriole.
The latter has a narrower diameter than that of afferent arteriole.
Blood vessels of glomerulus are similar to those of blood capillaries in being covered by a single layer of endothelial cells.
However, they are 100-500 times more permeable with fenestrations or pores having a size of 50-100 nm.
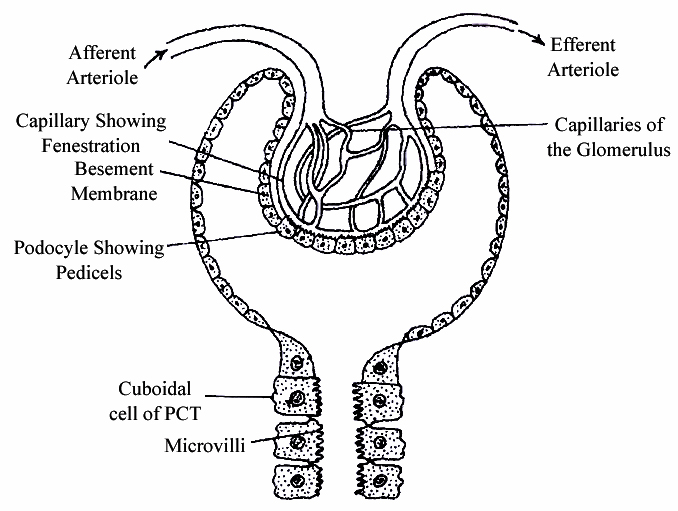
Malpighian body (renal corpuscle) : The complex formed by glomerulus, connective tissue and Bowman's capsule is called Malphighian body or renal corpuscle.
2. Proximal Convoluted Tubule (PCT):
Lower part of Bowman's capsule leads into proximal convoluted tubule.
The latter is present in the cortex.
It is twisted and surrounded by peritubular blood capillaries.
PCT is lined by cuboidal epithelium having brush borders with long microvilli for increasing absorptive area.
The cells contain abundant mitochondria and food reserve for providing energy to perform active absorption and secretion.
3. Loop of Henle:
Loop of Henle is made of two parallel limbs joined by curved base.
There is a descending limb and an ascending limb.
(i) Descending Limb:
Thick segment constitutes about four-fifth of the descending limb.
It lies both inside cortex and medulla.
The cells lining it are cuboidal.
They have sparse microvilli and fewer mitochondria indicating that active absorption and secretion are absent.
Thin segment is narrow part of descending limb.
It lies in the medulla and is lined by flat epithelial cells having sparse microvilli and few mitochondria.
Thin segment gets curved to become part of ascending limb.
(ii) Ascending Limb:
Ascending limb consists of thin segment in the proximal part and thick segment afterwards.
Thin segment is lined by flat epithelial cells which allow passive diffusion of some solutes (e.g., Na+, Cl–) depending upon their concentration gradient.
Thick segment of ascending limb is wider and lined by cuboidal cells having microvilli as well as mitochondria.
Thick ascending segment is involved in active secretion of NaCl in the medulla.
Vasa Recta : Loop of Henle is covered by a stair case of network of blood capillaries arising from efferent glomerular arteriole called vasa recta. It forms a counter-current system with the loop of Henle having ascending branch in the area of descending limb and descending branch in the area of ascending limb.
4. Distal Convoluted Tubule (OCT):
Distal convoluted tubule is highly coiled part of nephron and lies close to Malpighian body.
The epithelial lining of the distal convoluted tubule consists of cuboidal cells having sparse microvilli and deep mitochondria.
Distal convoluted tubule is covered by peritubular blood capillaries.
The last part of distal nephron is nearly straight, called connecting or junctional tubule and open into collecting duct.
Collecting Ducts:
Each nephron opens into a wider collecting tubule in the area of cortex.
Collecting tubules are lined by specialized cuboidal epithelium with very few microvilli.
They open into still wider collecting ducts.
Collecting ducts enter medulla and form ducts of Bellini.
The ducts run through renal pyramids.
Mechanism of Concentration of the Filter
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
Mechanism of Concentration of the Filter
KIDNEY TRANSPLANTATION
When both the kidneys are completely damaged kidney transplantation is done.
The world's first successful organ transplant was kidney transplantation which was undertaken by David Hume and Joseph Kelly at the Peter Bent Brigham Hospital in Boston in 1954.
The recipient was Richard Heerick who lived for a further eight years. The first kidney transplant in India was performed on Dec. 1, 1971 at the Christian Medical College, Vellore (Tamil Nadu) on a 35 year old patient named Shanmughan.
Most patients need to be dialysed before transplantation to avoid fluid overload and hyperkalaemia after the operation.
Antibiotics and immunosuppressive drugs are given before the operation.
Postoperative care is very essential.
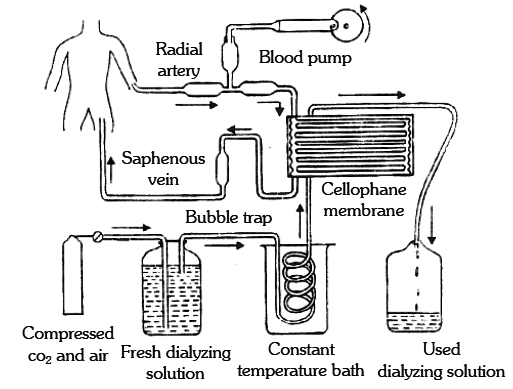
Regulation of Kidney Function
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
REGULATION OF KIDNEY FUNCTION
Control by Antidiuretic Hormone (ADH):
ADH, produced in the hypothalamus of the brain and released into the blood stream from the pituitary gland, enhances fluid retention by making the kidneys reabsorb more water.
The release of ADH is triggered when osmoreceptors in the hypothalamus detect an increase in the osmolarity of the blood above a set point of 300 mosm L–1.
In this situation, the osmoreceptor cells also promote thirst.
Drinking reduces the osmolarity of the blood, which inhibits the secretion of ADH, thereby completing the feedback circuit.
Control by Juxtaglomerular Apparatus (JGA):
Juxtamedullary nephrons help in retaining Na+ ions in high concentration in the interstitial fluid between the nephrons.
JGA operates a multi hormonal Renin-Angiotensin Aldosterone System (RAAS).
The JGA responds to a decrease in blood pressure or blood volume in the afferent arteriole of the glomerulus and releases an enzyme, renin, into the blood stream in the blood, renin initiates chemical reactions that convert a plasma protein, called angiotensinogen, to a peptide, called angiotensin II, which works as a hormone.
Angiotensin II is powerful constrictor of arterioles; one of the most potent vasopressor substances known.
Angiotensin II increases blood pressure by causing efferent arterioles to constrict.
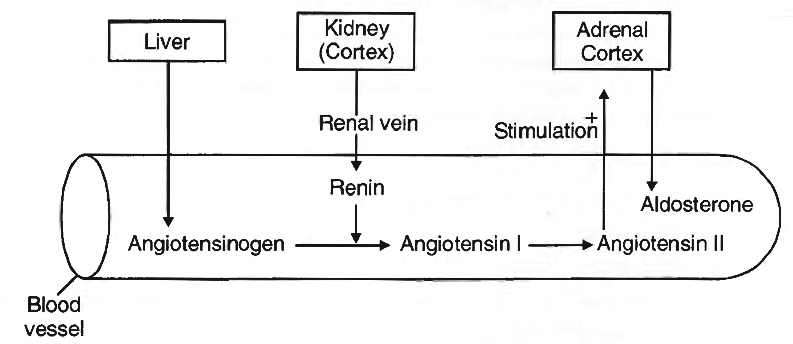
It also increases blood volume in two ways : firstly, by signalling the proximal convoluted tubules to reabsorb more NaCl and water, and secondly, by stimulating the adrenal gland to release aldosterone, a hormone that induces the distal convoluted tubule to reabsorb more Na+ and water.
This leads to an increase in blood volume and pressure, completing the feedback circuit by supporting the release of renin.
Atrial Natriuretic Factor (ANF), opposes the regulation by RAAS. (Renin -Angiotensin -Aldosterone System).
The wall of the atria of the heart release ANF in response to an increase in blood volume and pressure.
ANF inhibits the release of renin from JGA. This inhibits the reabsorption of Na+ by the collecting duct and reduces release of aldosterone from adrenal gland.
It also increases excretion of Na+ in urine.
Micturition
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
Micturition
Voiding or expulsion of urine stored in the urinary bladder is called micturition.
Urinary bladder gets gradually filled up with the urine.
Though the capacity of urinary bladder is above 800 ml, but as the volume is around 500 ml, its wall gets stretched.
Urine formed by nephrons is ultimately carried to the urinary bladder where it is stored till a voluntary signal which is initiated by the stretching of urinary bladder as it gets fill with urine.
Stretch receptors generate nerve impulse that is carried by sensory neuron to brain producing the sensation of fullness.
This initiates the autonomic reflex (parasympathetic involving sacral spinal nerves) resulting in contraction of detrusor muscles of urinary bladder and inhibition of motor impulse of voluntary, striated external sphincter, making it relaxed; and urine comes out.
Micturition can be initiated voluntarily also by contracting the abdominal muscle which applies pressure over urinary bladder, activating the stretch receptors.
Role of other organs in Excretion
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
ORGANS IN EXCRETION
Lungs:
The lungs help in removing CO2 and water. Lungs eliminate around 18 L of CO2 per hour and about 400 ml of water per day in normal resting condition.
Water loss will increase in cold dry climatic condition and will decrease in hot, humid climate. Different volatile material are also readily eliminated through lungs.
Skin:
Skin contains large number of sweat glands richly supplied with blood capillaries, from which they excrete sweat and some metabolic wastes.
Since the skin sends out plenty of water and small amount of salts, hence it serves as an excretory organ.
Sebaceous glands in skin eliminate sebum which contains waxes, sterols, some hydrocarbons & fatty acids.
Liver:
It produces bile pigments which are metabolic wastes of haemoglobin of dead R.B.C's.
Liver is also the main site for elimination of cholesterol, inactivated products of steroid hormones, some vitamins and many drugs.
Large Intestine:
Epithelial cells of large intestine excrete Ca2+, Mg2+, Fe2+ into the lumen of intestine and comes out along with faecal matter.
Disorders of the Excretory System
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
Disorders of the Excretory System
1. Nephritis: The infection is caused by bacteria which results in inflammation of the kidney.
2. Glomerulonephritis: Inflammation of glomeruli.
3. Pyelonephritis: Inflammation of the tissue of kidneys in the pelvis region.
4. Cystitis: Inflammation of the urinary bladder.
5. Renal Calculi: Stone or insoluble mass of crystallized salts (oxalate etc.) formed within kidney.
6. Polyurea: Amount of urine passed out is more.
7. Uremia: The concentration of urea is increased in blood.
8. Alkaptonuria: It is a genetic disease in which homogentisic acid in excreted out with urine.
9. Pyuria: Presence of pus in the urine.
10. Glycosuria: Presence of glucose in urine.
11. Haematuria: Presence of blood in the urine.
12. Inulin is a fructan storage polysaccharide. It is not metabolised in human body and is a readily filtered through kidneys. It is therefore used in testing kidney function, especially glomerular filtration rate.
13. Tubular maxima: The maximum amount of substance that can be retained in blood and beyond which it will be excreted in urine.
Types of Movement
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
TYPES OF MOVEMENTS
Movements can be of 2 categories.
1.Non-Muscular Movements:
These movements persist in the animals in some of their cells.
(i) Protoplasmic Streaming: Streaming of protoplasm called cyclosis, has been seen in most of the cells such as leucocytes, Amoeba and other unicellular organisms.
(ii) Pseudopodial Movements: Leucocytes and macrophages move about in the tissues with the help of pseudopodia in the same manner as of Amoeba.
(iii) Flagellar Movements: The flagella of certain cells (e.g., choanocytes of poriferans) maintain by their ceaseless vibrations a regular current of water through the canal system of sponges. The flagella of certain gastrodermal cells circulate fluid in the coelenteron of Hydra by regular beating. Sperms swim in water or in female genital tract by flagellar movements.
(iv) Ciliary Movements: The cilia of the cells lining the trachea, oviducts and vasa efferentia propel dust particles, eggs and sperms in specific direction. The cilia of flame cells push waste material in excretory canals in flatworms.
The non-muscular ciliary locomotion is retained by some animal larvae such as the planula larva of coelenterates and the trochophore of annelids, and even some adults such as planarians.
2.Muscular Movements:
This depends upon the use of muscle fibres which have ability to exert force by alternate contraction and relaxation.
Most multicellular organisms have muscle fibres for moving different body parts or locomotion.
A muscle contraction does not always result in movement. It may at times maintain status quo, as in a fresh water mussel (mollusc), muscle contract to keep shell closed for safety.
Muscles
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
Muscles
In human, muscular movements are involved.
Types:
There are three types of muscle tissue; striated or striped, nonstriated or unstriped or smooth, and cardiac, according to their location, structure and function.
Structure of Skeletal Muscle
The striated muscle forms 80% or more of the mass of soft tissues in a vertebrate body and found in the body wall and the limbs. It also occurs in the tongue, pharynx and beginning of oesophagus.
Skeletal muscle are having a connective tissue sheath on the outer side and is called epimysium.
A transverse section of it shows a number of bundles or fasciculi.
Each fasciculus is surrounded by connective tissue cover called perimysium.
Within a fasciculus, are present a large number of muscle fibres, each surrounded by connective tissue cover endomysium.
There is a broad band of fibrous connective tissue beneath the skin or around muscles called fascia.
Each muscle fibre is cylindrical, uniform in diameter. Sarcolemma is present on outer side and at places is invaginated to form T or transverse tubules. A skeletal or striated muscle fibre is multinucleated or syncytial.
Ultra Structure of Skeletal Muscle Fibre
Structure:
A striated muscle consists of long, narrow, cylindrical, unbranched fibres with blunt ends.
Each fibre is bounded by an elastic sarcolemma and contains many elongated, flattened nuclei characteristically located near the sarcolemma.
Multinucleate condition results from cell fusion. Hence, a striated muscle fibre is a syncytium.
The striated muscle fibres contain numerous mitochondria and glycogen granules for the supply of adequate energy.
The myofibrils of a striated muscle fibre show alternating dark and light cross bands, the striations, or stripes, hence the name of the muscle.
The dark bands are called anisotropic or A bands.
Each A band has at its middle a light zone termed Henson's line, or H zone.
The light bands are isotropic and are known as the isotropic or I bands.
Each I band is crossed through its centre by a dark membrane, the membrane of Krause, or Z line.
This membrane continues right across the whole fibre and joins the sarcolemma surrounding the fibre.
It seems to hold the myofibrils together and to carry the signals for the contraction of the fibrils inward from the T-tubules (transverse tubules).
The latter are invaginations of sarcolemma into the fibre adjacent to the Z lines.
The part of the myofibril between two successive Z lines functions as a contractile unit termed the sarcomere.
The sarcoplasm also contains a protein pigment myoglobin, which can take up, store, or give up oxygen like haemoglobin.
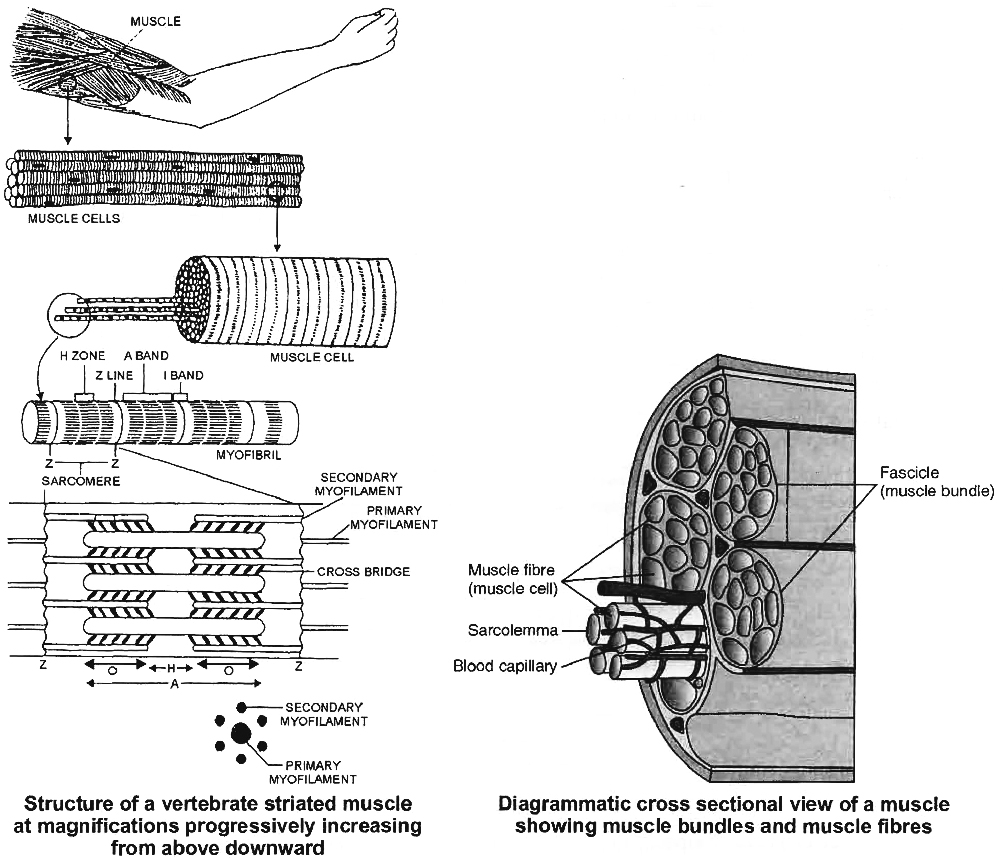
Electron microscope reveals that each sarcomere is a bundle of fine longitudinal myofilaments of two types : primary and secondary.
(i) Primary Myofilaments:
The primary myofilaments are thicker and confined to the A band only.
They are composed of the protein myosin; bear minute projections called cross-bridges of the protein meromyosin; and are free at both the ends.
(ii) Secondary Myofilaments:
The secondary myofilaments are thinner and occur in I bands, but extend for some distance into the A band between the primary myofilaments.
This partial overlapping of the primary myofilaments by the secondary myofilaments imparts dark appearance to the A bands.
The secondary myofilaments are composed of the proteins actin, tropomyosin and troponin; have a smooth surface; and are attached to the Z lines by one end, being free at the other end.
The secondary (actin) myofilaments are more numerous than the primary (myosin) myofilaments.
Six actin myofilaments surround each myosin myofilament and each actin myofilament is surrounded by three myosin myofilaments.
Mechanism of Muscle Contraction
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
MUSCLE CONTRACTION
When a nerve impulse (nerve action potential) reaches the synaptic end bulbs, it triggers exocytosis of synaptic vesicles.
In this process, the synaptic vesicles fuse with the plasma membrane and liberate ACh, which diffuses into the synaptic cleft between the motor neuron and the motor end plate.
When ACh binds to its receptor, a channel that passes small cations, most importantly Na+ opens.
The inrush of Na+ changes the resting membrane potential, which triggers a muscle action potential that travels along the muscle cell plasma membrane and initiates the events leading to muscle contraction.
Hanson and Huxley proposed that skeletal muscle shortens during contraction because thin filaments slide over thick filament.
Their model is known as the sliding filament mechanism of muscle contraction.
Sliding Filament Mechanism
During muscle contraction, myosin heads pull on the thin filaments, causing them to slide inward towards the H zone at the centre of the sarcomere.
The myosin cross bridges may even pull the thin filaments of each sarcomere so far inward that their ends overlap in the centre of the sarcomere.
As the thin filaments slide inward, the Z discs come towards each other, and the sarcomere shortens, but the lengths of the thick and thin filaments do not change.
The sliding of the filaments and shortening of the sarcomeres cause shortening of the whole muscle fibre and ultimately the entire muscle.
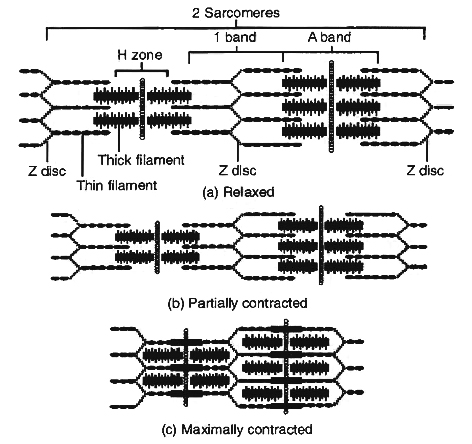
Role of Calcium and Regulator Proteins
An increase in Ca2+ concentration in the sarcoplasm starts filament sliding, while a decrease turns off the sliding process.
When a muscle fibre is relaxed (not contracting), the concentration of Ca2+ in its sarcoplasm is low.
This is because the sarcoplasmic reticulum (SR) membrane contains Ca2+ active transport pumps that move Ca2+ from the sarcoplasm into the SR.
Ca2+ is stored or sequestered inside the SR.
As a muscle action potential travels along the sarcolemma and into the transverse tubule system, however, Ca2+ release channels open in the SR membrane.
As a result, Ca2+ floods into the sarcoplasm around the thick and thin filaments.
The Ca2+ released from the sarcoplasmic reticulum combine with troponin, causing it to change shape.
This shape change moves the troponin -tropomyosin complex away from the myosin-binding sites on actin.
Troponin has 3 units (tri units structure)
1. TpT - tropomyosin binding troponin
2. TpC - calcium binding protein
3. Tpl - Inhibitor i.e., blocks myosin binding site of actin proteins
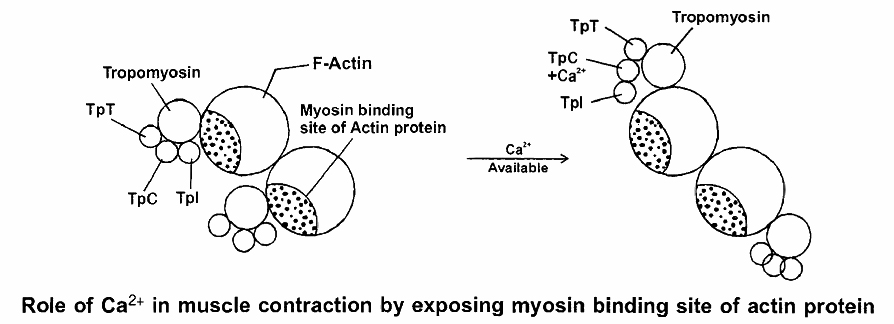
The Power Stroke and the Role of ATP
As we have seen, muscle contraction requires Ca2+ ions and energy in the form of ATP. The sequence of events during sliding of the filaments are
(i) While the muscle is relaxed, ATP attaches to ATP-binding sites on the myosin cross bridges (heads). A portion of each myosin head acts as an ATPase, an enzyme that splits the ATP into ADP + P (phosphate group) through a hydrolysis reaction. This reaction transfers energy from ATP to the myosin head, even before contraction begins. The myosin cross bridges are thus in an activated (energized) state.
(ii) When the sarcoplasmic reticulum releases Ca2+, its level rises in the sarcoplasm. Rise in Ca+2 binds with troponin and change its configuration that moves away tropomyosin from its blocking position.
(iii) The activated myosin heads spontaneously bind to the myosin-binding sites on actin.
(iv) The shape change that occurs as myosin heads bind to actin produces the power stroke of contraction. During the power stroke, the myosin heads swivel toward the centre of the sarcomere, like the oars of a boat during rowing. This action draws the thin filaments past the thick filaments toward the H zone. As the myosin heads swivel, they release ADP.
(v) Once the power stroke is complete, ATP again combines with the ATP-binding sites on the myosin heads. As ATP binds, the myosin head detaches from actin.
(vi) Again, the myosin ATPase splits ATP, transferring its energy to the myosin ATPase splits head, which returns to its original upright position .
(vii) The myosin head is then ready to combine with another myosin-binding site further along the thin filament.
The steps (iii) through (vii) repeats over and over as long as ATP is available and the Ca2+ level near the thin filament is high.
The myosin heads keep rotating back and forth with each power stroke, pulling the thin filaments toward the H zone.
At anyone instant, about half of the myosin heads are bound to actin and are swiveling.
The other half are detached and preparing to swivel again.
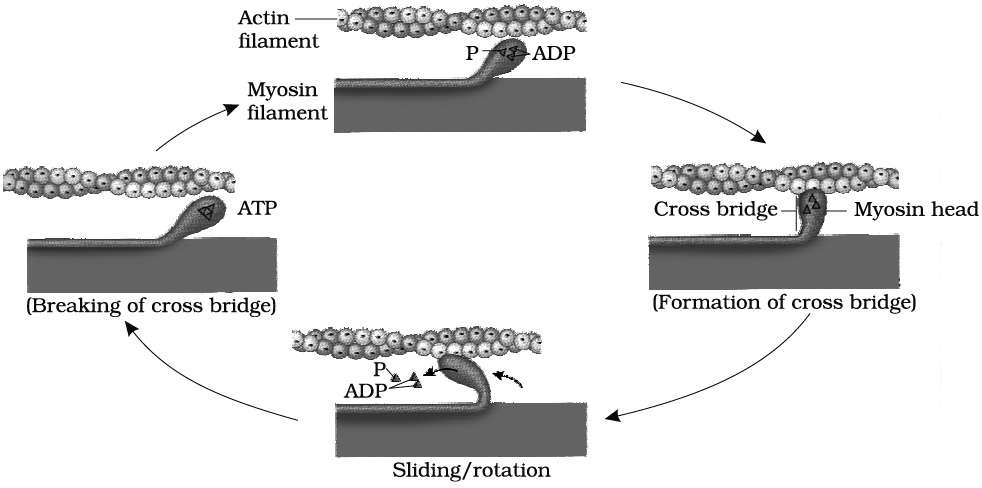
This continual movement of myosin heads applies the force that draws the Z discs toward each other, and the sarcomere shortens.
The myofibrils thus contract and the whole muscle fibre shortens.
During a maximal muscle contraction, the distance between Z discs can decrease to half the resting length.
H-line and M-line disappear, I-band almost disappears, A-band remains constant, but the power stroke does not always result in shortening of the muscle fibres and the whole muscle.
Contraction without shortening is called an isometric contraction, for example, in trying to lift a very heavy object.
The myosin heads (cross bridges) swivel and generate force, but the thin filaments do not slide inward.
Relaxation: Two changes permit a muscle fibre to relax after it has contracted.
First, acetylcholine is rapidly broken down by an enzyme called acetylcholinesterase (AChE).
When action potentials cease in the motor neuron, release of ACh stops, and AChE rapidly breaks down the ACh already present in the synaptic cleft.
This ends the generation of muscle action potentials, and the Ca2+ release channels in the sarcoplasmic reticulum membrane close.
Second, Ca2+ active transport pumps rapidly remove Ca2+ from the sarcoplasm into the sarcoplasmic reticulum, where molecules of a calcium-binding protein, appropriately called calsequestrin, bind to the Ca2+.
With this, the tropomyosin-troponin complex move back over the myosin binding site of actin which prevents further binding of myosin head to actin and the thin filaments slide back to their normal relaxed position.
All or None Principle
A minimal strength of a stimulus required to cause the contraction of a muscle fibre brings about maximum contraction, and no further increase in contraction would occur by increasing the strength of the stimulus.
Single Muscle Twitch
A Single, quick isolated contraction of a muscle fibre to a single stimulus of threshold value is called single muscle twitch in the laboratory experiments.
Energy Source of Muscle Contraction
Energy for muscle contraction is provided by hydrolysis of ATP by myosin ATP-ase enzyme.
This hydrolysis produces ADP, inorganic phosphate and energy (used in muscle contraction).
Phosphocreatine donates its high energy and phosphate to ADP, producing ATP.
Phosphocreatine serves as an energy source for a few seconds for metabolic processes in the muscle cells to begin to produce greater quantities of ATP.
Phosphocreatine is again formed in relaxing muscle by using ATP produced by carbohydrate oxidation.
ATP + H2O ![]() ADP + Pi + Energy
ADP + Pi + Energy
(Inorganic phosphate)
Phosphocreatine + ADP ![]() ATP + Creatine
ATP + Creatine
At the end of muscle contraction, the conversion of ADP into ATP takes place.
The muscle is rich in glycogen which is broken down into lactic acid through a series of reactions (glycolysis) and liberates energy.
Some of this energy is used for the reformation of phosphocreatine and also for the conversion of 4/5th of lactic acid back into glycogen.
The 1/5th of lactic acid is oxidised to water and carbon dioxide.
These reactions taking place in the muscle and liver, are proposed by Cori and Cori, hence known as Cori's cycle.
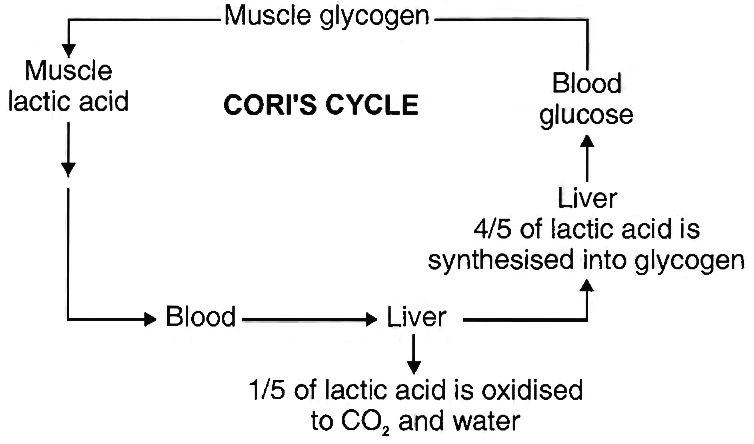
Rigor Mortis
Extreme rigidity of body after death is called rigor mortis. It is due to complete depletion of ATP and phosphocreatine.
Red and White Muscle Fibres
Birds and mammals have two kinds of striated muscle fibres in their skeletal muscles; red or slow muscle fibres and white or fast muscle fibres.
Differences between red muscle fibres and white muscle fibres
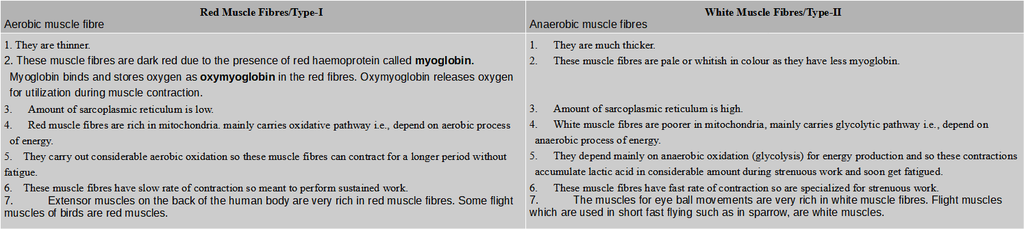
Contraction in Smooth Muscles:
In comparison with contraction in a skeletal muscle fibre, contraction in a smooth muscle fibre starts more slowly and lasts much longer Troponin is absent in smooth muscle so they have regulator protein called Calmodulin that binds to Ca2+ in the cytosol.
Using ATP, myosin head part can bind to actin & contraction can occur.
Most smooth muscle fibres contract or relax in response to action potentials from the autonomic nervous system.
Contraction in Cardiac Muscles:
Cardiac muscle fibres have the same arrangement of actin & myosin and the same bands, zones and Z discs as skeletal muscle fibres.
Gap junctions allow muscle action potential to spread from one muscle fibre to another.
As a consequence, when a single muscle fibre is stimulated, all the other fibres in the network become stimulated as well.
Thus, each network contracts as a functional unit.
Cardiac muscle tissue has a long refractory period and can use lactic acid produced by skeletal muscle fibres to make ATP.
Skeletal System
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
SKELETAL SYSTEM IN HUMAN
The skeletal system is divided into two main parts.
(i) Axial Skeleton. It lies along the principal axis of the body. It includes skull, vertebral column, ribs, sternum and ribs.
(ii) Appendicular Skeleton. It is made up of the girdles and limb bones.
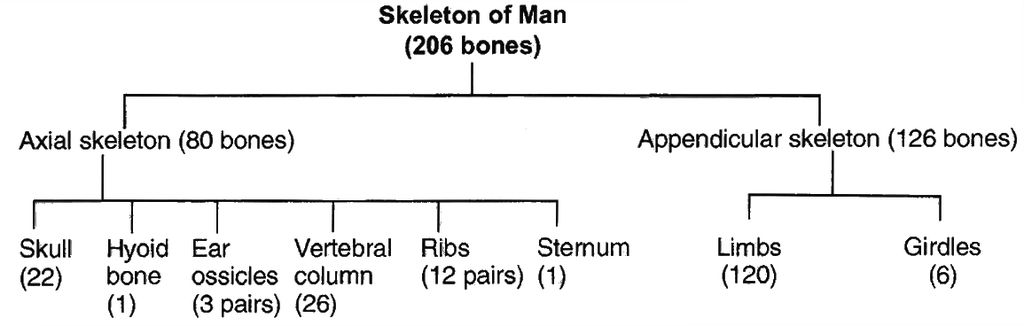
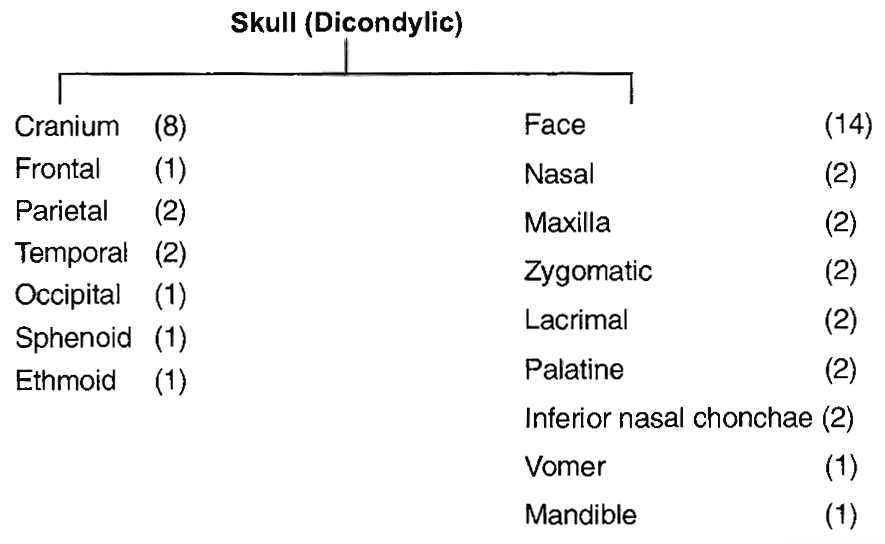
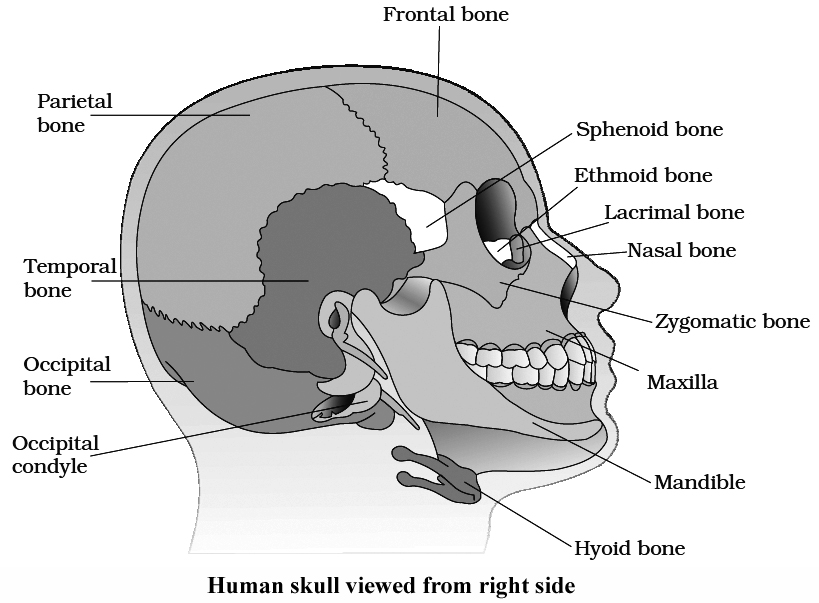


Hyoid
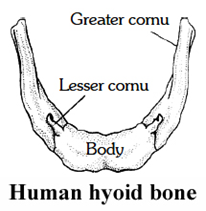
It serves as a point of attachment for some of the muscles of the tongue and floor of the mouth but does not articulate with any other bone.
Ear Ossicle
Ear ossicles are three in number

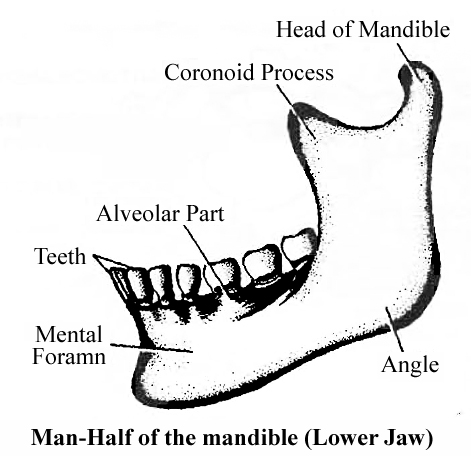
VERTEBRAE
Vertebral column protects the spinal cord, supports the head and serves as the point of attachment for the ribs and musculature of the back.
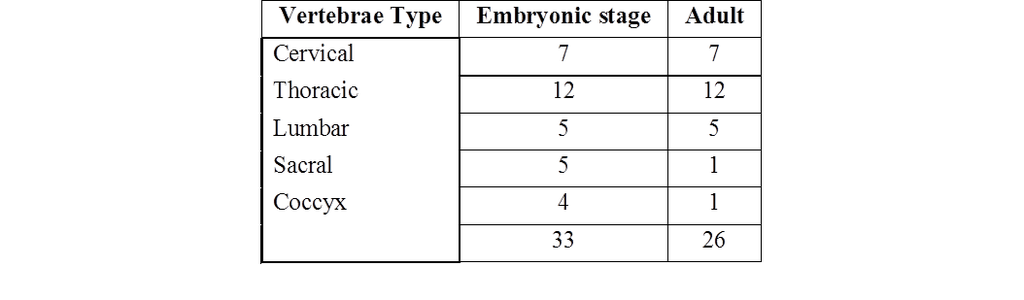
Cervical vertebrae
(i) 1, 2, 7 cervical vertebrae are atypical and 3 to 6 are typical.
(ii) The transverse processes are perforated by foramina (foramen transversarium) for the passage of the vertebral arteries except in VII Vertebrae.
(iii) The first cervical vertebra or atlas supports the head and consists of a complete ring of bone. On its upper surface it presents kidney-shaped facets for articulation with the condyles of the occipital bone, forming a condyloid joint, the atlanto-occipital joint, at which the nodding movements of the head take place. The atlas articulates with the second cervical vertebra.
(iv) The second cervical vertebra or axis is the pivot on which the atlas turns in the rotary movements of the head. From the body of the axis a process of bone rises which is called the odontoid peg which articulates with the back of the anterior arch of the atlas and is held in position by the transverse ligament of the atlas. The lateral masses of the atlas articulate with corresponding facets on the axis placed on each side of the odontoid peg. The atlas moves round the odontoid peg of the axis, forming a pivot joint at which the head rotates.
(v) The seventh cervical vertebra is the first vertebra with an undivided spinous process. This process has a tubercle at its tip. It forms a distinct projection in the neck and can be seen at the lower part of the back of the neck. Because of this characteristic the bone is called the vertebra prominens.
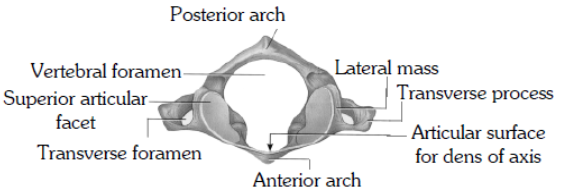
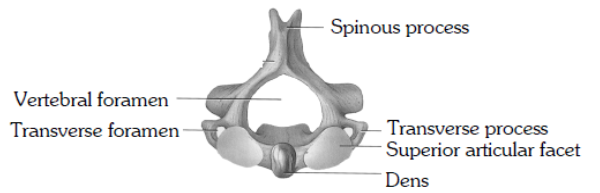
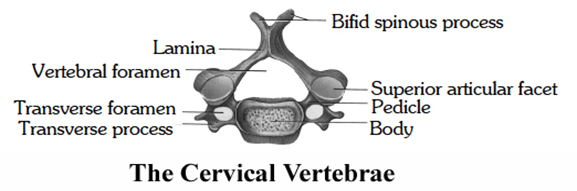
Thoracic Vertebrae
(i) Thoracic 2-8 are typical 1, 9, 10, 11, 12 are atypical.
(ii) These are larger than the cervical and they increase in size as they extend downwards.
(iii) The body is heart-shaped, with facets on each side for attachment of the ribs.
(iv) The neural arch is relatively small, the spinous process is long and is directed downwards.
(v) The transverse processes which help to support the ribs are thick, strong and carry articular facets for the ribs.
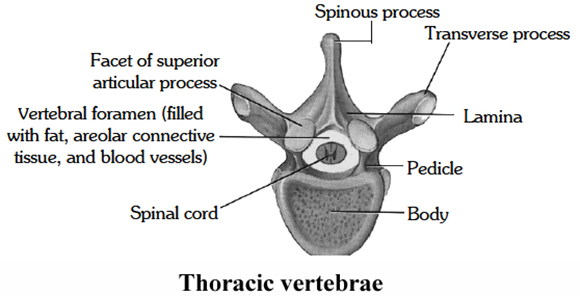
Lumbar Vertebrae
(i) These are the largest vertebrae as compared with the bodies of the other vertebrae and is kidney-shaped.
(ii) The spinous process is broad and hatchet-shaped.
(iii) The transverse processes are long and slender.
(iv) The fifth lumbar vertebra articulates with the sacrum at the lumbo-sacral joint.
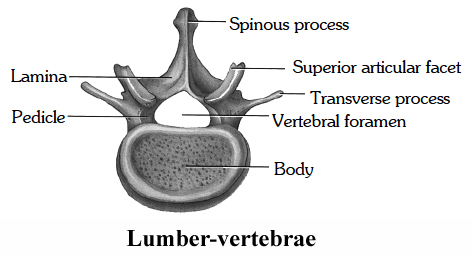
Sacrum
(i) It is a triangular bone situated at the lower part of the vertebral column, wedged in between the two innominate bones and forming the back of the pelvic cavity.
(ii) The base of the sacrum lies above and articulates with the fifth lumbar vertebra, forming a typical intervertebral joint.
(iii) The junction between the fifth lumbar vertebra and the sacrum forms the sacro-vertebral angle.
(iv) At the extremities of transverse ridges, on each side, sacral foramina are present for the passage of nerves. The apex of the sacrum articulates with the coccyx. At the sides the sacrum articulates with the innominate bones, forming the right and left sacro-iliac joint.
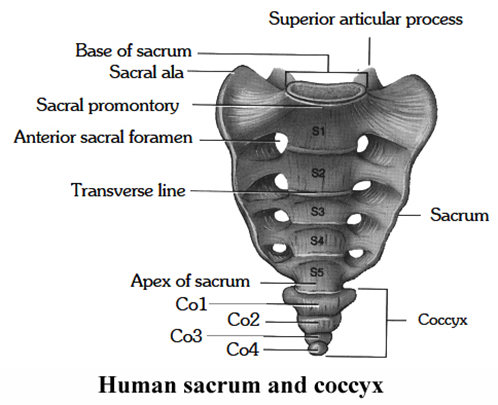
Coccyx
It is composed of four or five rudimentary vertebrae, fused to form one bone. It articulates above with the sacrum.
Joints
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
THE JOINTS
A bone joint or articulation may be defined as the junction of two bones. The study of such joints is known as arthrology.
There are three principal types of bone joints.
(i) Fibrous joints or immovable or fixed joints/synarthrosis
(ii) Cartilaginous joints/Amphiarthrosis
(iii) Synovial joints/Diarthrosis
(i) Fibrous Joints.
These joints are immovable or fixed.
They do not show any movement due to the presence of strong and tough white collagenous fibres and there is no joint cavity.
These joints include:
(a) Sutures: Found between skull bones, articulating bones are held together by white fibrous tissue.
(b) Gomphoses : Teeth in mandibles and in maxillary bones.
(c) Shindylases : One bone fits into slit in another e.g., ethmoid bone in vomer.
(ii) Cartilaginous Joints.
They are slightly movable joints.
Discs of white fibrocartilage, strong but more elastic and compressible than the white fibrous tissue, hold the bones together at the joints between the bodies of the vertebrae, at the symphysis pubis, and between the sternum and ribs.
The bones make some movements at such joints through compression of the discs of the cartilage.
(iii)Synovial Joints.
Synovial joints are of different types depending upon the nature of articulation and degree of movement.
Synovial joints are of the following types:
(a) Ball and socket joints ( = Enarthroses) : The 'head' of one bone fitting with the 'socket' of the other bone and allowing free movement in all planes; e.g. shoulder joint and hip joint.
(b) Hinge joints ( = Ginglymi) : The perfect joints which allow the movements only in a single plane. e.g. elbow joint, knee joint and ankle joint
(c) Pivotal joints (=Rotary joints or rotaria) : One of the two bones is fixed in its place and bears a peg like process over which rotates the other bone; e.g. atlas along with the skull rotating over the odontoid process of axis vertebra in mammals.
(d) Saddle joints : It is similar to ball and socket joints but are poorly developed and movements are comparatively less free, e.g. the joint between the metacarpal of thumb with the carpals below.
(e) Gliding joints: The joints which permit sliding of the articulating bones on each other; e.g. joint between the zygapophyses of successive vertebrae, and between sternum and clavicle.
(f) Angular joints (= or ellipsoid or condyloid) : These joints allow the movements in two directions, i.e., side to side and back and forth; e.g., metacarpophalangeal joints.
Disorder of Muscular and Skeletal System
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
Disorder of Muscular and Skeletal System
1.The rheumatoid arthritis:
It is diagnosed by the presence of rheumatoid factor (a type of immunoglobulin IgM).
It is the primary symptom of inflammation of synovial membrane.
If it is left untreated, then the membrane thickens and synovial fluid increases, exerting pressure that causes pain.
The membrane then starts secreting abnormal granules, called pannus, which after accumulating on the surface of the cartilage, causes its erosion.
As a result, the fibrous tissues are attached with the bones and become ossified, making the joints immovable heat treatment and physiotherapy pain and inflammation and in extreme cases, replacement of the damaged joints is recommended
2. Osteoarthritis:
It is a degenerative joint disease characterised by the degeneration of the articular cartrlage and proliferation of new bones.
Usually, affected joints are of spine, knees and hands.
3. Gouty Arthritis or Gout:
It is caused either due to excessive formation of uric acid, or inability to excrete it.
It gets deposited in joints as monosodium salt.
4. Osteomalacia and Rickets:
Osteomalacia, called rickets when it occurs in childhood.
In this disease disorder this bones contain insufficient amounts of calcium and phosphorus.
The cause of kidney disease, vitamin D deficiency, and an inherited defect.
5. Osteoporosis:
Osteoporosis is a disease in which bone loses minerals and fibres from its matrix.
Individuals taking hydrocortisone for arthritis, allergies, or other disorders are especially prone to bone loss.
6. Bursitis:
The bursae of joints often become inflamed, a condition known as bursitis.
The inflammation can be caused by a physical injury or by constant pressure to the same joint over a long period of time.
7. Dislocation:
A dislocation is a displacement of the articular surfaces of a joint; it usually involves a damage to the ligaments surrounding the joint.
Most dislocations result from falls, blows, or extreme exertion and are most often seen in the joints of the thumb, fingers, knee or shoulder.
Symptoms of dislocation include swelling, pain, and loss of motion.
8. Sprain and Strains:
A sprain is a twisting of a joint without dislocating it.
Such an injury causes damage to ligaments and also often damages tendons, muscles, blood vessels, and nerves.
Severe sprains are quite painful and require immobilization during the healing process.
In contrast to a sprain, a strain is a less severe stretching or twisting of a joint.
Muscles and tendons may be stretched and become somewhat painful, but only minor damage is done to the tissues of the joint.
9. Myasthenia gravis:
Auto immune disorder affecting neuromuscular junction leading to fatigue, weakening and paralysis of skeletal muscle.
10. Muscular dystropy:
Progressive degeneration of skeletal muscle mostly due to genetic disorder.
11. Tetany:
Rapid spasm (wild contraction) in muscle due to low Ca++ in body fluid.
Human Neural System
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
Human Neural System
The neural system of all animals is composed of highly specialised cells called neurons, which can detect, receive and transmit different kinds of stimuli.
The neural organisation is very simple in lower invertebrates. For example, in Hydra it is composed of network of neurons.
Neural system is better organised in insects, where a brain is present along with number of ganglia and neural tissues.
The vertebrates have a more developed neural system.
Human Neural System Human neural system is divided into two parts:
(i) The Central Nervous System (CNS)
(ii) The Peripheral Nervous System (PNS)
The CNS includes the brain and the spinal cord and is the site of information processing and control.
The PNS comprises of all the nerves of the body associated with CNS (brain and spinal cord).
The nerve fibres of the PNS are of two types
(a) Afferent Fibres (b) Efferent Fibres
Afferent fibres transmit impulses from tissues/organs to the CNS and the efferent fibres transmit regulatory impulses from the CNS to concerned peripheral tissues/organs.
PNS is divided into two divisions called somatic neural system and autonomic nervous system.
Somatic neural system relays impulses from the CNS to skeletal muscles while the autonomic neural system transmits impulses from CNS to the involuntary organs and smooth muscles of the body.
The autonomic neural system is further classified into sympathetic neural system and parasympathetic neural system.
structure of neuron
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
A neuron is a microscopic structure composed of three major parts : (i) cell body , (ii) dendrites and (iii) axon . Thell contains cytoplasm , cell organelles and certain granular bodies called Nissl's granules . Dendrites are shon branch repeatedly and project out of the cell body . They also contain Nissl's granules .
Dendrites transmit impulses towards the cell body . The axon is a long fibre , the distal end of which is bra branch terminates into a bulb - like structure called synaptic knob . Synaptic knob possess synaptic vesicle con chemicals called neurotransmitters . The axons transmit nerve impulses away from the cell body to a synapse ar neuromuscular junction.
Types of Neurons
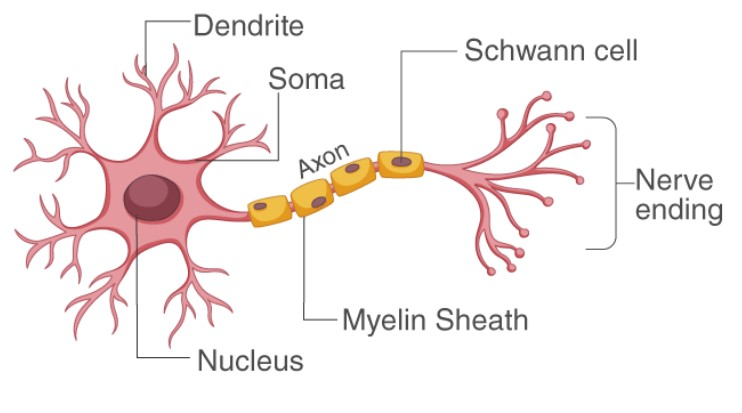
Based on the number of axon and dendrites , the neurons are divided into three types :
Unipolar neurons have cell body with one axon only . They are found usually in the embryonic stage.
Bipolar neurons are with one axon and one dendrite . They are found in the retina of eye .
Multipolar neurons are with one axon and two or more dendrites . These are found in the cerebral cortex
On the basis of function , neurons are of two types :
Afferent neurons : These neurons carry impulses from receptors CNS . They are sensory in nature . The terminals of dendrites become modified to form receptors .
Efferent neurons : They carry impulses from CNS to effectors like muscles or glands . They are motor in nature . The axon terminals come in contact with the motor end plate to form neuromuscular junction .
Types of Axons
There are two types of axons : myelinated and non - myelinated .
The myelinated nerve fibres are enveloped with Schwann cells , which form a myelin sheath around the axon . The gaps between two adjacent myelin sheaths are called nodes of Ranvier . Myelinated
nerve fibres are found in spinal and cranial nerves .
Unmyelinated nerve fibre is enclosed by a Schwann cell that does form a myelin sheath around the axon . It is commonly found autonomous and the somatic neural systems .
generation and conduction of impulse
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
Generation and conduction of impulse
Nerve cell have polarised membrane i.e., have electrical potential difference or membrane potential.
This is because of a variety of ion channels (pores formed by proteins) specific for a particular type of ions.
Some remain open while most ion channels open under one condition, but closes under other condition.
Because of such regulated or voltage gated channel, membrane become excitable as these channels respond to different type of stimuli e.g., Light, touch, sound etc.
When a neuron is not sending any signal, it is said to be at rest and its membrane has resting membrane potential.
Resting Membrane Potential
In the resting nerve fibre, the cytoplasm just beneath its membrane is electronegative relative to the layer of extracellular fluid (ECF) just outside the membrane.
If the two sides of the membrane are connected by galvanometer (double beam cathode ray oscilloscope) the inner side is seen to possess a negative potential of about 70 mV relative to the outerside.
This is called the resting membrane potential. This results from two factors:
(i) The resting membrane has a poor permeability for Na+ although it has a higher permeability for K+. Therefore, K+ can cross more easily while Cl– and Na+ have more difficulty in crossing.
(ii) Negatively charged protein molecule inside the neuron cannot cross the plasma membrane because of its semipermeability.
The differential flow of the positively charged ions and the fact that the negatively charged organic ions within the nerve fibre cannot pass out cause an increasing positive charge on the outside of the membrane and negative charge on the inside of the membrane.
This makes the membrane of the resting nerve fibre polarized (i.e., its outside being positively charged with respect to the inside.)
Such electrochemical gradients are maintained by the active transport of ions involving Na+ – K+ ion transmembrane pump.
It pumps out 3Na+ for every 2K+ ions passed inwardly.
K+ concentration is 30 times more inside neuron than outside and Na+ concentration is 10 times more in interstitial fluid as compared to inside of neuron.
Conduction of Nerve Impulse
It involves initiation of impulse followed by conduction along the axon so as to be transferred to target muscle/tissue.
Initiation of Impulse:
When stimulated, voltage gated Na+ channel open which causes a rapid, very localised, temporary inflow of Na+ into the cell which causes development of net positive charge on the inner side of membrane in that area.
This is called depolarisation.
It occurs at a particular region of neuron called trigger zone.
Voltage gated ion channels are clustered in the area of trigger zone.
Stimulus of threshold value causes stoppage of Na+ – K+ ATP-ase pump.
Continued passage of Na+ ions into inside of neuron creates a reverse potential of +20 mV to +30 mV, rarely to +60 mV.
The total change occurs in spike-like fashion which is also called spike potential.
Na+ ion channels open for about 0.5 m sec.
It creates a potential that sets in a wave of depolarisation through the nerve fibre.
The membrane potential which sets in a wave of depolarisation is called action potential.
For most excitable cells, the threshold is about -55 mV to -60 mV.
Conduction of Impulse:
In the area of depolarisation, the potential difference across the membrane is small while its nearby region has large difference in membrane potential.
This produces a small local current in the area.
The local current becomes a stimulus and causes the gated Na+ channels of next region to open and depolarise the area to produce fresh action potential.
The process will continue till the impulse reaches the end of neuron.
Repolarisation:
As the Na+ channels close after 0.5 m sec the membrane becomes extra permeable to K+ ions due to opening of K+ ion gates.
With the pumping out of K+ ions, the neuron interior becomes negative and the potential falls back to resting potential.
The phenomenon of change of membrane potential from excited state to resting state is called repolarisation.
However, K+ ion channels remain open for a bit longer period so that the membrane potential becomes more negative than -70 mV.
It is called hyperpolarisation.
It takes about 1 -5 m sec for repolarisation.
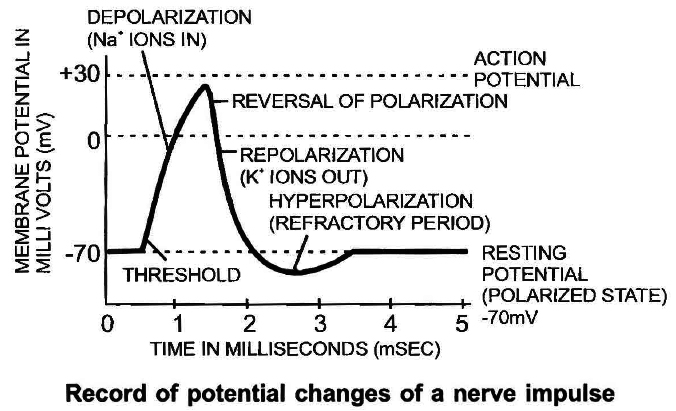
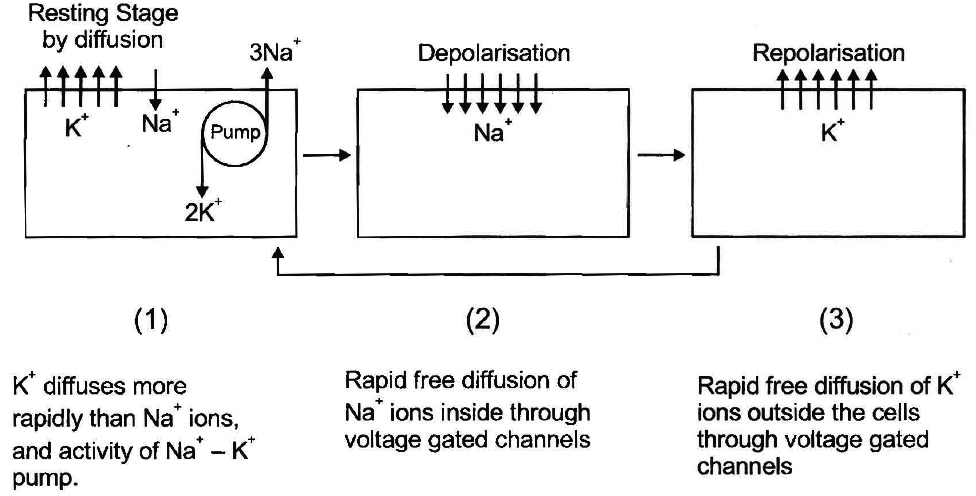
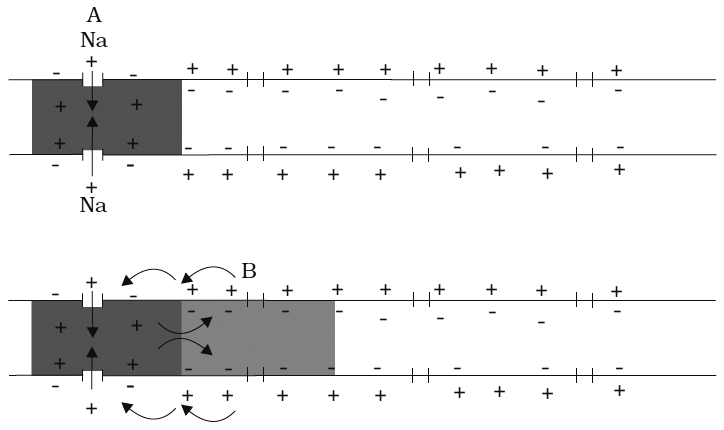
Figure: Diagrammatic representation of impulse conduction through an axon (at points A and B)
transmission of impulse
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
Transmission of impulse
Synapes are the neuroneuronal junctions through which information from one neuron can pass to the other.
There are mainly two types of synapses depending upon the nature of transfer of information across the synapse. (1) Electrical, (2) Chemical
1.Electrical Synapses:
At an electrical synapse, ionic current spreads directly from one cell to another through gap junctions.
Each gap junction contains is hundred or so tubular protein structures called connexons that from tunnel to connect the cytosol of the two cells.
This provides a path for ionic current flow.
Gap junctions are common in visceral (single-unit) smooth muscle, cardiac muscle, and a developing embryo.
They also occur in the CNS.
Electrical synapses have three obvious advantages:
(i) They allow faster communication than do chemical synapses, since impulses conduct across gap junction.
(ii) They can synchronize the activity of a group of neurons or muscle fibers. The value of synchronized action potentials in the heart or in visceral smooth muscles is to achieve coordinated contraction of these fibers.
(iii) They may allow two-way transmission of impulses in contrast to chemical synapses, which function as one way points of communication.
2. Chemical Synapses:
Chemical synapse have 10 to 20 nm gap which is too great a distance for such direct electrical coupling.
Chemical synapses are commonest type of synapse, these consist of a bulbous expansion of a nerve terminal, called synaptic knob, lying in close proximity to the membrane of a dendrite or other part of neuron.
The cytoplasm of the synaptic knob contains numerous tiny, round sacs, called synaptic vesicles.
Each vesicle has a diameter of approximately 50 nm, and contains as many as 10,000 molecules of a neurotransmitter substance responsible for the transmission of nerve impulse across the synapse.
The membrane of the synaptic knob on the axon side, thickened as a result of cytoplasmic condensation, is called presynaptic membrane.
Mechanism of transmission of nerve impulse through chemical synapse
Wave of depolarisation reaches the presynaptic membrane.
3
Voltage-gated calcium channels open, Ca++ ions diffuses into the axon terminal from the surrounding fluid.
3
Ca++ stimulates fusion of synaptic vesicle with pre-synaptic membrane, and release of neurotransmitter by
exocytosis into synaptic cleft.
3
Neurotransmitter bind with specific receptor molecules of post-synaptic membrane.
3
This binding opens sodium ion channels allowing the entry of Na+ ions
which can generate a new potential in the post-synaptic neuron.
3
The new potential developed may be either excitatory or
inhibitory depends upon neurotransmitter.

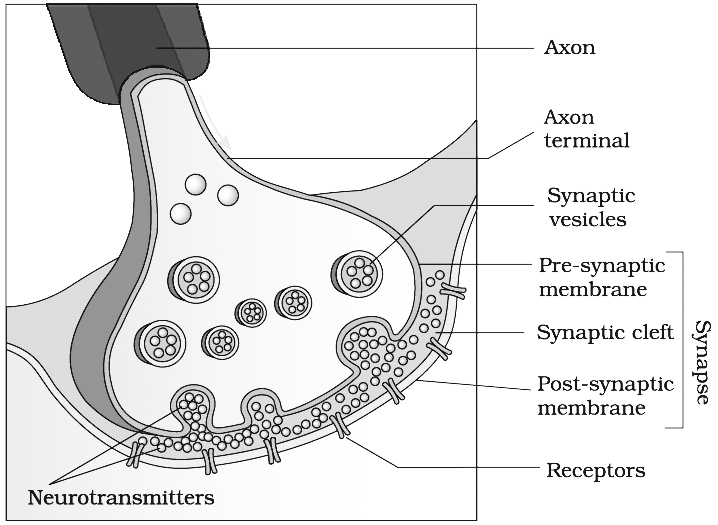
Concept Builder
1. Acetylcholinestrase is present in the muscle cell or post synaptic neuron. It breaks down acetylcholine into acetate and choline and terminate the action of the transmitter.
2. Nor epinephrine secreted by sympathetic neural system and also by some neurons of central neural system is inactivated by enzyme monamine oxidase.
Central Neural System
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
Central Nervous System
The structures of the CNS arise from its embryological components.
Prosencephalon
(i) Becomes the thalamus and hypothalamus (diencephalon) and
(ii) The cerebral cortex, corpus striatum, hippocampus and amygdala (telencephalon).
Mesencephalon
Becomes mid brain.
Rhombencephalon develops into
(i) The medulla (myelencephalon)
(ii) The pons and cerebellum (metencephalon).
BRAIN
Meninges :
The brain is surrounded by three protective coats of connective tissue besides the bony cranium. These are known as meninges (singular, meninx).
(i) Piamater : It is the inner meninx. It is very thin, highly vascular, and closely invests the brain. It is covered by simple squamous epithelium.
(ii) Arachnoid Mater or Membrane: It is the middle meninx. It is also thin but is nonvascular. It is covered with simple squamous epithelium on both (intemal and extemal) surfaces. There is a narrow space between the pia mater and the arachnoid membrane. It is called the subarachnoid space. It contains cerebrospinal fluid and is crossed by a number of connective tissue strands.
(iii) Duramater : It is the outer meninx. It is thick, tough and lines the cranial cavity. Its internal surface is covered with simple squamous epithelium. A very narrow space also exists between the dura mater and the arachnoid membrane. It is called the subdural space. It contains a little fluid which is not the cerebrospinal fluid.
The adult human brain contains more than 100 billion neurons and almost 10 times neuroglia cells. The brain is divided into three main sections:
(i) Fore brain; (ii) Mid brain; (iii) Hind brain
Fore brain: It consists of two main parts, the cerebrum and the diencephalon.
(a) Cerebrum. By far the largest and most highly developed part of the brain is cerebrum. It is divided into two hemispheres by a prominent longitudinal fissure. The two hemispheres are connected by a bundle of transverse fibres called corpus callosum. The anterior part of corpus callosum is curved and is called genu while the posterior part is called splenium. Each cerebral hemisphere is divided into four lobes. These are the frontal at the front, the parietal towards the top of the head, the temporal on the side and the occipital at the rear.
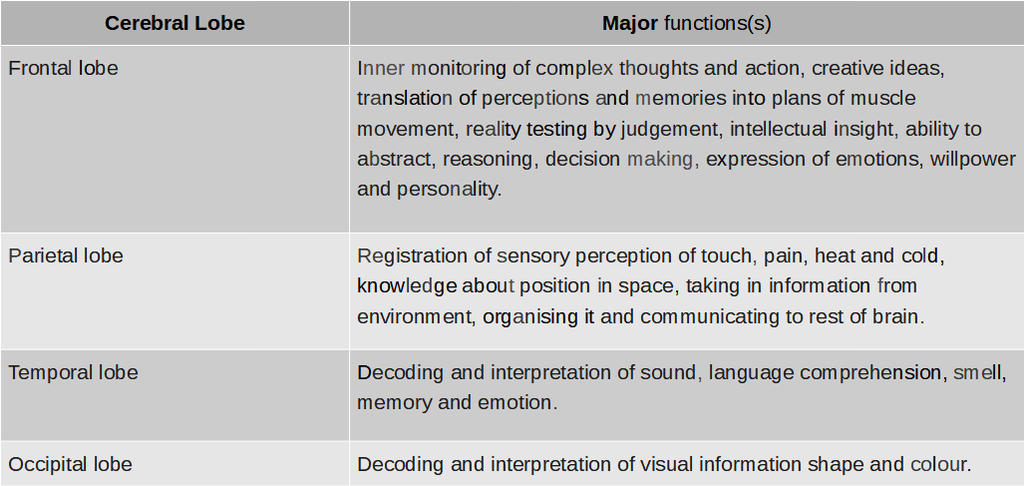
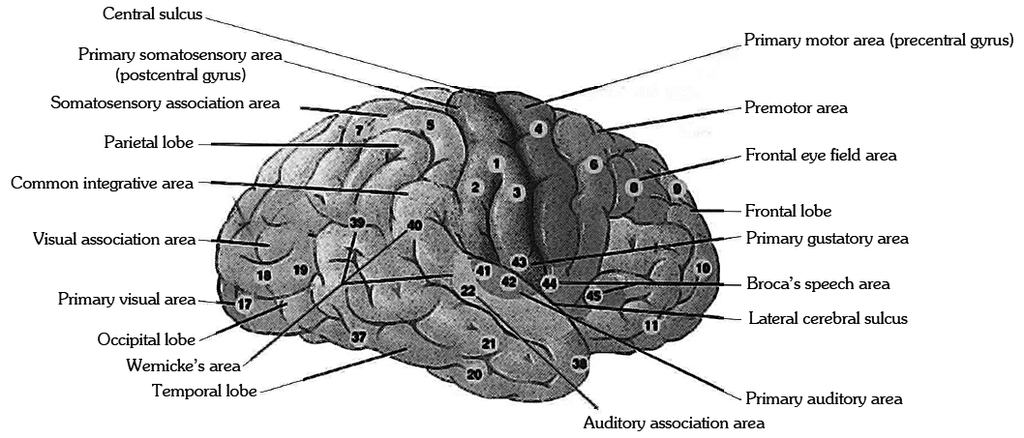
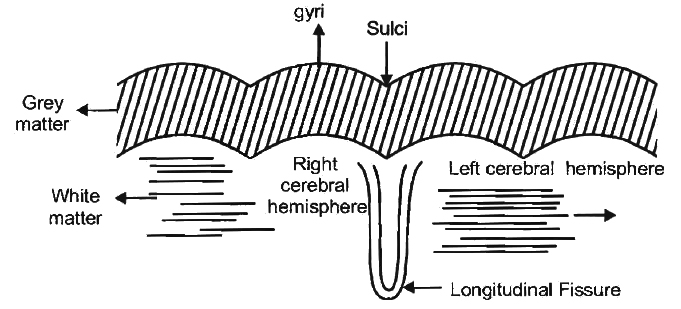
Cerebral cortex :
The outer surface of cerebrum, called the cortex, is a layer only 2-4 millimetres thick.
Because the six layers of it are packed with ten billion (109) pyramidal, spindle and stellate neurons with a greyish brown appearance, it is referred to as grey matter.
The cerebral cortex contains roughly 10 percent of all neurons of brain.
Much of the neural activities occur here, e.g., from the touch of a feature to the movement of an arm.
Unlike mouse brain, human brain is greatly convoluted.
These convolutions or folds consist of sulci (sing. Sulcus : small groove), fissures (large grooves), and gyri (sing. Gyrus : buldge between adjacent sulci or fissures).
These greatly enlarge the surface area of the cortex.
In fact, two-thirds of the surface of the cortex is hidden in the sulci and fissures.
Thus, their presence triples the area of the cerebral cortex.
Beneath this run millions of axons comprising nerve fibre tracts, connecting the neurons of cerebral cortex with those located elsewhere in the brain.
The large concentration of myelin gives this tissue an opaque white appearance.
Hence, they are referred by the term white matter.
By examining the effect of injuries or lesions and the effect of electrical stimulation on the behaviour, it has been possible to map roughly the location of its various associative activities on the cerebral cortex.
Each area is referred to as a specialised cortex.
There are three general kinds of cortex : sensory, motor and associative.
(b) Diencephalon:
The diencephalon contains the epithalamus, thalamus and hypothalamus.
Epithalamus is thin, non nervous roof of diencephalon.
Its anterior region is folded and fused with piamater to form anterior choroid plexus.
This is responsible for formation of CSF.
Above it is present pineal stalk bearing the pineal body at the top of it.
Pineal body is endocrine gland and also taken as vestige of 3rd eye.
The thalamus directs sensory impulses from the lower parts of the brain and spinal cord to appropriate parts of the cerebrum.
Limited sensory awareness of pain, temperature, touch and pressure is provided by the thalamus.
Hypothalamus:
As the name implies, hypothalamus nestles at the base of the thalamus, and so of the brain.
Although relatively small, just 4 grams, about 1/300 of the total brain mass is highly vascularised.
It integrates and controls the visceral activities.
The hypothalamus, through its connection with brain stem, maintains homeostasis and the body's internal equilibrium, specialising in involuntary behaviour control.
The nuclei in it signal the body to eat, drink, get angry, keep cool, and make love and so on.
Hyothalamus organises behaviour related to survival of species: fighting, feeding, fleeing and mating.
It keeps body temperature at roughly 37ºC by means of a complex thermostat system.
It also influences respiration and heartbeat and sends out signals to correct them when they are wrong.
Through connections with the pituitary gland, the hypothalamus controls growth and sexual behaviour.
It also controls many more functions.
Basal Ganglia:
The inside of human brain is not so densely packed, but there are all kinds of different collections of neurons, called nuclei, each with its specific functions.
These control different body activities automatically.
Basal ganglia is a collection of subcortical nuclei in the forebrain, at the base of the cortex.
The largest nucleus in it is the corpus striatum.
It regulates planning and execution of stereotyped movements.
Other basal ganglia perform at subconscious level learned pattern of movements like slow and fast pedalling; slow and fast writing/typing etc.
Destruction of dopamine secreting pars compacta part of basal nucleus called substantia nigra leads to paralysis agitansl parkinson's disease. Huntington's chorea is due to degeneration of GABA secreting neurons of corpus striatum and acetylcholine secreting neurons of other parts.
Limbic System :
Flared like a wish bone a ring or fork, through extensive neural links with the cerebrum and the brain stem below, constitute what is called limbic (meaning lip-like) system.
This system sends out signals to the rest of the brain and the body which have great effect on your behaviour.
Limbic system includes hypothalamus, amygdala, hippocampus, septum, anterior nucleus of thalamus and portion of basal ganglia.
Amygdala :
Above the hypothalamus, attached to the interior lips of both forks, is almond-shaped amygdala.
This bulge of neurons is like a defense castle controlling the moods, especially anger and rage.
Various regions of the amygdala play important role in emotional behaviour, such as aggression and remembering fear.
Hippocampus:
Taking its name from the Greek for "sea horse", whose shape roughly resembles, the hippocampus make the swollen lower lip of the limbic fork.
The remarkable organ deals with a strange mix of signals about smells and memories.
The hippocampus functions as a kind of index for recall of an event with its associated memory.
The hippocampus converts information from short-term to long-term memory, essential in learning.
The septum linked to the hypothalamus contains yet another emotion centre for sexual arousal.
Mid Brain
It has two structures -corpora quadrigemina and cruracerebri.
(a) Corpora Quadrigemina :
It contains 4 lobes, therefore, corpora quadrigemina.
Its principal structures are superior colliculi and inferior colliculi.
The superior pair of colliculi receive sensory impulses from the eyes and muscles of the head and control visual reflexes.
For example, they control and coordinate the movement of the head and eyes, to fix and focus on an object.
The inferior pair of colliculi receive sensory impulses from the ears and muscles of the head and control auditory reflexes such as the movement of the head to locate and detect the source of a sound.
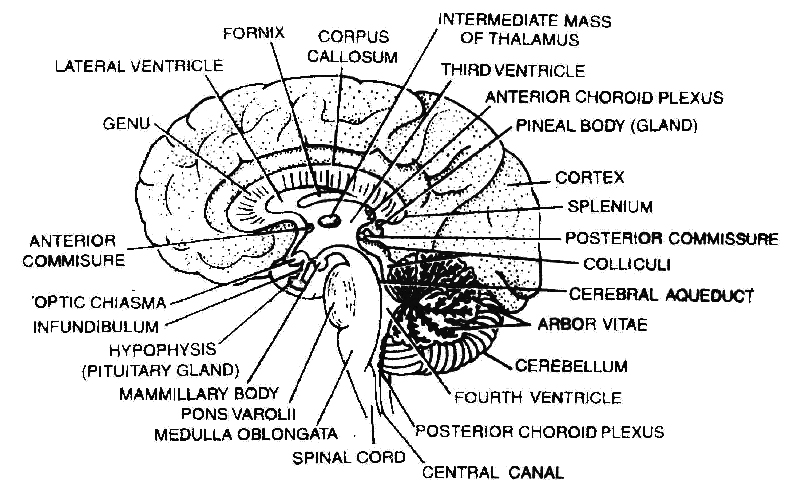
(b) Crura cerebri (Cerebral peduncle) :
These are two heavy fibrous tracts on the inferior side of mid brain and connect hind brain with fore brain.
Crura cerebri is involved in controlling muscle tone and modifying some motor activities.
These relay sensory as well as motor impulses between fore brain and hind brain.
Hind Brain
Consist of cerebellum, Pons and Medulla.
Cerebellum:
To the rear of the brain and placed under the cerebrum, is the second largest part of the brain, called the cerebellum that means simply "little cerebrum".
Wedged between cerebral hemispheres and brainstem, cerebellum is made up of two cerebellar hemispheres.
Like the cerebrum, the cerebellum has its grey matter on the outside, comprising of three layers of cells and fibres.
The middle layer contains characteristically large-flask-shaped Purkinje cells.
Tree-like themselves with myriad of dendrites, purkinje cells rank among the most complex of all neurons.
The white and grey matter form arbor vitae.
Central portion of the cerebellum has worm like appearance as it is narrow and furrowed.
It is called Vermis.
Three paired bundles of myelinated nerve fibres, called cerebellar peduncles, form communication pathways between the cerebellum and other parts of the CNS.
The superior cerebellar peduncles connect the cerebellum to the midbrain, the middle cerebellar peduncles communicate with the pons, and the inferior cerebellar peduncles consist of pathways between the cerebellum and the medulla oblongata, as well as spinal cord.
Cerebellum does not initiate movement but modulates or reorganises motor commands.
Cerebellum's unconscious directions and cerebrum's conscious instructions determine how and when to move body parts.
The cerebellum is vital to the control of rapid muscular activities, such as running, typing and even talking.
All the activities of the cerebellum are involuntary, but may involve learning in their early stages.
Pons, (Latin meaning : the bridge) forms the floor of the brain stem.
It serves as a neuronal link between the cerebral cortex and the cerebellum.
It has pneumotaxic centre, the switch off centre for inspiration.
Medulla oblongata, literally meaning oblong marrow, is the posterior most part that connects the spinal cord and various parts of the brain.
It has with it breathing centre, cardiovascular centre, vomiting centre.
Vagus nerve arises from medulla.
Its roof is thin and non-nervous and constitute posterior choroid plexus.
Below the plexus, the roof has three opening, a pair of lateral apertures called foramina luschka and a single median foramina Magendie.
These apertures connect external and internal components of CSF of brain.
Most of the sensory as well as motor nerve tracts cross over to the other side in medulla, therefore, right half of cerebrum controls left half of body and vice a versa.
Reticular formation that connects to the thalamus and major nerves in the spinal cord, is the gatekeeper to consciousness.
Brain Stem: It is the area of the brain between the thalamus and the spinal cord and includes medulla, pons and midbrain. Diencephalon mayor may not be included.
Ventricles of the Brain and Cerebrospinal Fluid
The ventricles consist of four hollow, fluid filled spaces inside the brain.
A lateral ventricle lies inside each hemisphere of the cerebrum.
Each lateral ventricle is connected to the third ventricle by an interventricular formen (foramen of Monro).
The third ventricle consists of a narrow channel between the hemispheres through the area of the thalamus.
It is connected by the cerebral aqueduct or aqueduct of Sylvius or iter in the midbrain portion of the brain stem to the fourth ventricle in the pons and medulla.
The fourth ventricle continues with the central canal of the spinal cord.
Three openings in the roof of the fourth ventricle, a pair of lateral apertures (foramina of Luschka) and a median aperture (foramen of Magendie) allow cerebrospinal fluid to move upward to the subarachnoid space that surrounds the brain and spinal cord.
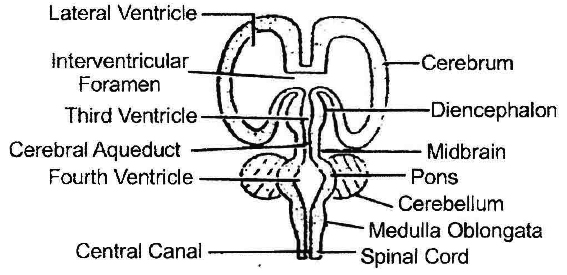
The cerebrospinal fluid is secreted by anterior choroid plexus and posterior choroid plexus and is found inside the ventricles of the brain, the central canal of the spinal cord.
The cerebrospinal fluid acts as a shock absorber for the brain and spinal cord and may also contribute to nourish brain tissue it contains protein, glucose, chloride and water.
Spinal Cord
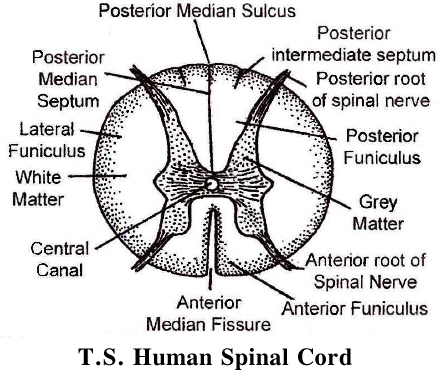
It is an elongated cylindrical structure which lies in the neural canal of the vertebral column and is continued with the \ medulla oblongata through foramen magnum of the skull.
It measures about 45 cm in length.
It extends down upto first lumbar vertebra where it tapers to a point called conus medularis/conus terminalis.
However, the meninges of the spinal cord continues as filum terminale starts from the conus, and runs upto coccygeal region.
The spinal cord shows two enlargements
(i) Brachial swelling -from 4th cervical to 1st thoracic vertebrae.
(ii) Lumbar swelling -from 9th thoracic to 12th thoracic vertebrae.
The spinal cord possesses an anterior and a posterior median fissure running along its length.
The grey matter of spinal cord is internal and present around the central canal.
It is produced into a posterior and anterior pairs of grey columns/roots.
Each dorsal root has a ganglion called dorsal root ganglion.
Dorsal root is sensory and ventral root is motor in nature. Both get combine with each other before coming out of vertebral column through intervertebral foramina.
The white mater is outer, and divided into four funiculi one dorsal, one ventral and two lateral.
Spinal cord conducts impulses to and from the brain.
Dorsal funiculus has ascending nerve tract for conducting sensory impulses towards brain.
Lateral and ventral funiculus conduct motor impulse from brain to spinal cord.
It controls most of the reflex activities.
Reflex Action and Reflex Arc
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
Reflex Action and Reflex Arc
The reflex action is the simplest kind of activity which can be defined as an integrated activity occurring involuntarily in response to a stimulus applied to a receptor.
The reflex arc is composed of the following:
(i) receptor organ; (ii) an afferent neuron; (iii) synapse involving some cells in the CNS (modulator); (iv) an efferent neuron; and (v) an effector organ.
(A) Reflexes can be classified in a number of ways as follows:
(a) Unconditioned reflexes: These are inborn, e.g., knee jerk, salivation on tasting the food, peristalsis, closing of eyes on being approached by an object.
(b) Conditioned reflexes: These are acquired, i.e., developed after birth through conditioning or learning e.g., secretion of saliva after seeing tasty food, playing a musical instrument, knitting without looking, writing as well as reading.
(B) According to the number of synapses in the reflex path
(a) Monosynaptic reflexes: When there is only one synapse in the reflex path. e.g., Knee jerk.
(b) Polysnaptic reflexes: When there are more than one synapse in the reflex path.
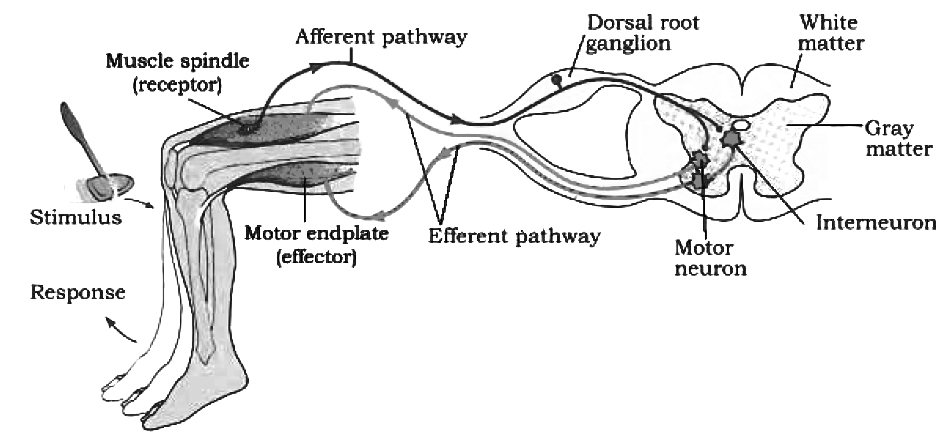
Concept Builder
Salivation on seeing or hearing or smelling delicious food; is an example of cerebral reflex action and withdrawl of legs; when a drop of HCl drop over the sciatic nerve of decapitated frog is an example of spinal reflex action.
Characteristics of Reflexes
Although the reflexes are involuntary functions, they have certain features which make them highly complicated. Some important characteristics are:
(i) Predictability: Once the response of an organ to a specific stimulus is observed, one can predict that the same stimulus will always elicit the same response.
(ii) Purposefulness: Generally all reflex actions are useful to the organism and are performed with a definite purpose.
(iii) Localization : In performing a reflex action, a specific effector is involved in response to the stimulus applied to a specific receptor.
(iv) Delay: Reflex time is the interval between the application of the stimulus to a receptor and the beginning of a response by an effector organ. A synaptic delay occurs due to latent period and reflex time at the synapse. This depends upon the number of synapses in the nerve pathway.
(v) Unlearned: In order to activate spinal effector mechanisms, no experience is needed to bring them in operation.
(vi) Adjustive and Protective: Reflexes serve adjustive and protective purposes and become an important part of the animal behaviour.
(vii) Fatigue: Reflex responses are readily fatigued after prolonged and continuous work. As a consequence, the latent period of contraction becomes longer and the rise of tension smaller and more gradual.
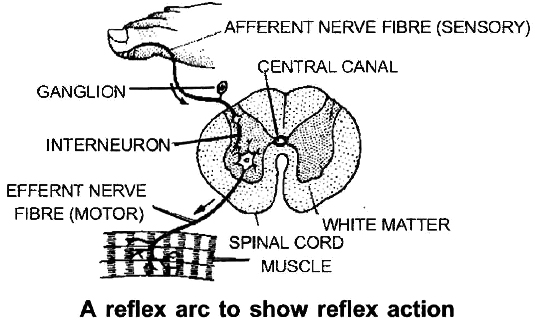
Sensory Reception and processing
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
Sensory Reception and processing
The stimuli are received by certain structures in the body.
These are called receptors or sense organs.
A receptor may be extremely simple, such as those of touch, taste and smell, or they may be highly complex in their structure as well as working e.g., the sense organs of sight and hearing.
CLASSIFICATION OF SENSE ORGANS
(1) According to their position:
(i) Exteroreceptors -The external sense organs which receive the stimuli from outer environment.
(ii) Proprioreceptors -Simple receptors present in joints, skeletal muscles, tendons etc. They are not in direct contact with environment but are affected by the changes in the environment.
(iii) Visceroreceptors or internal receptors -The receptors present within the visGera. They receive stimuli originating within the body itself. They are simple and mostly represented by free nerve endings. Perception is conscious awareness and interpretation of sensation.
(2) According to the form of stimulus they receive, the sense organs are classified into the following types given in the Table.
Tangoreceptors-
These are the sense organs for touch, pressure, pain, heat or cold. They are located in the skin and include:
(i) Meissner's corpuscles : They are present immediately below the epidermis, and receive the stimulus of touch/gentle pressure.
(ii) Pacinian corpuscles : Situated deep in the dermis of skin, joints, tendons and muscles. Each corpuscle has a nerve ending surrounded by connective tissue. They respond to pressure changes.
(iii) Merkel's disc occurs in the epidermis and are responsible for touch.
Skin is often called hypothermio because it has more cold receptors. The regulation of temperature in human body is mediated by hypothalamus which has a 'set point' (96.4°F or 37°C) around which the core temperature ossilates.
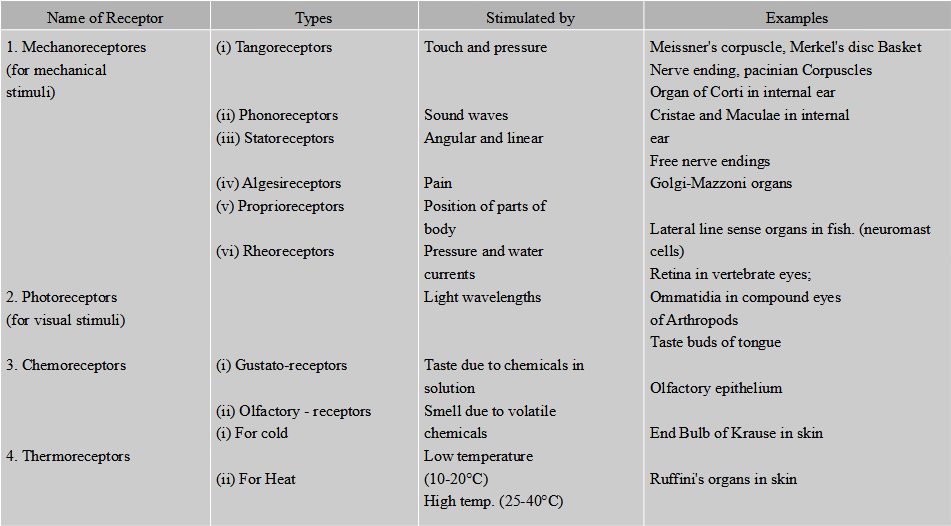
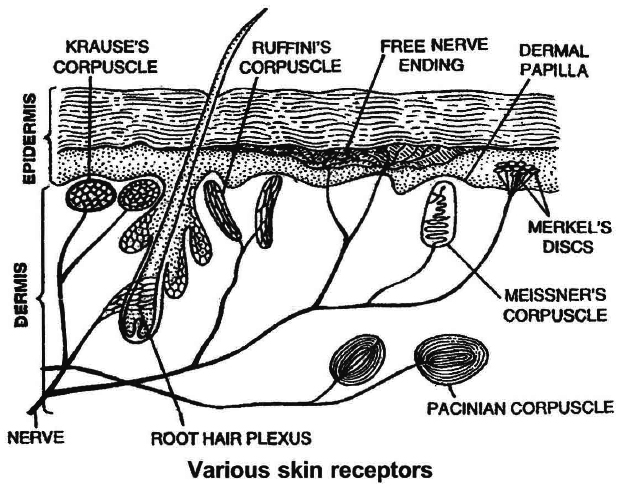
SMELL RECEPTORS (Olfactoreceptors)
Location:The receptors of smell occur in a small patch of olfactory epithelium (pseudostratified epithelium) located in the roof of the nasal cavity.
(i) Olfactory Receptor Cells: They act as sensory receptors as well as conducting neurons. The olfactory receptor cells are "unusual" bipolar neurons. Each cell is spindle shaped and has a thin apical dendrite that terminates in a knob which bears non motile cilia called olfactory hairs. Olfactory receptor cells are unique in that they are the only neurons that undergo turnover throughout adult life.
(ii) Supporting Cells: These are columnar cells which lie between the olfactory receptor cells to support them. They have brownish yellow pigment (similar to lipofuscin) which gives the olfactory epithelium its yellowish colour.
(iii) Basal Cells: These are small cells that do not reach the surface. They give rise to new olfactory receptor cell to replace the worn out ones. This is an exception to the fact that neurons are not formed in the postnatal (after birth) life. The olfactory receptor cells survive only for about two months.
Olfactory glands (Bowman's glands): Many olfactory glands occur below the olfactory epithelium that secrete mucus to spread over the epithelium to keep it moist. The mucus also protects the cells from dust and bacteria.
Working: The dissolved chemicals stimulate the olfactory receptors by binding to protein receptors in the olfactory hairs (cilia) membranes and opening specific Na+ and K+ channels. This leads ultimately to an action potential that is conducted to the first relay station in the olfactory bulb. The fibres of the olfactory nerves synapse with mitral cells (second = order neurons) in complex structures called glomeruli (balls of yarn). When the mitral cells are activated, impulses from the olfactory bulbs via olfactory tracts to main destinations (e.g., temporal lobe of the cerebrum).
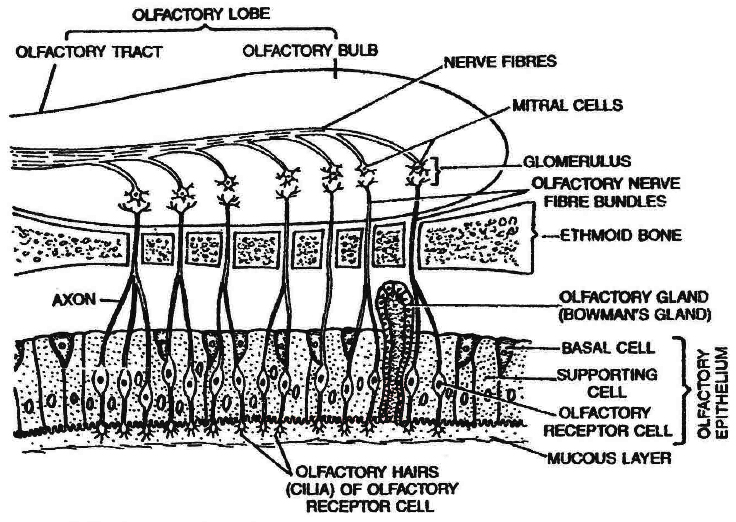
Women often have a keener sense of smell than men, especially at the time of ovulation.
Smoking damages the olfactory receptors.
With ageing the sense of smell deteriorates.
Hyposmia (hypo-less, osmi-smell) is a reduced ability to smell.
Concept Builder
In addition to smell receptors nose, mouth and tongue contain a network of nerves that form trigeminal nerve (fifth cranial nerve) also known as dentist's nerve reacts to message of path.
Brain combines the trigeminal signals with those of smell to identify some odours.
When exposed to irritants such as ammonia or vinegar.
The trigeminal can protect by warning about harmful chemicals in the air. Bowman's glands inside the nose release fluids to get rid of the irritating substances.
TASTE RECEPTORS (Gustatoreceptors)
Location: The receptors for taste are found in the taste buds, mostly located on the tongue but also found on the palate, pharynx and epiglottis and even in the proximal part of oesophagus. The number of taste buds declines with age.
Structures : Each taste bud is an oval body consisting of three kinds of cells.
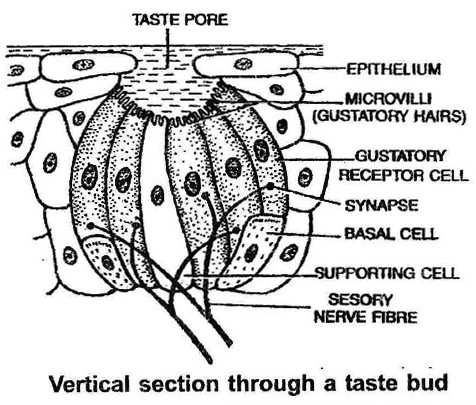
(i) Gustatory Receptor Cells: They bear at the free end microvilli projecting into the taste pore. The microvilli have special protein receptor sites for taste-producing molecules and come in contact with the food being eaten. Nerve fibres of the cranial nerves VII (facial), IX (glossopharyngeal) or X (Vagus) end around the gustatory receptor cells, forming synapses with them. The gustatory receptor cells (taste cells) survive only about 10 days and are then replaced by new cells.
(ii) Supporting cells: These cells lie between the gustatory receptor cells in the taste bud. They bear microvilli but lack nerve endings.
(iii) Basal Cells: These cells are found at the periphery of the taste bud. They produce supporting cells, which then develop into gustatory receptor cells.
Working: Specific chemicals in solution pass into the taste bud through the taste pore to come in contact with the protein receptor sites on the microvilli of the gustatory receptor cells. The latter set up nerve impulses in the sensory nerve fibres. The nerve fibres transmit the impulses to the taste centre in the brain (e.g., parietal lobe of the cerebrum) where the sensation of taste arises.
The facial nerve (VII) serves the anterior two-thirds of the tongue, the glossopharyngeal nerve (IX) serves the posterior one-third of the tongue and the vagus nerve (X) serves the pharynx and epiglottis but not the tongue.
Eye and Ear
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
Eye and Ear
EYE
Organs of sight in man are a pair of eyes located in the eye orbits of the skull.
The exposed part of the eye is protected by a upper and a lower eyelid which are provided with eye lashes.
Each eye is represented in the form of a spherical eye ball which is moved in the eye orbit by the help of six eye muscles namely superior oblique, inferior oblique, superior rectus, inferior rectus, external rectus and internal rectus.
Eyeball measures about 2.5 cm. in diameter and is hollow.
Its wall is formed of three layers or coats-the outermost is called fibrous coat, the middle one as vascular coat and the inner one as retina.
(i) Fibrous coat : The outer coat of the eyeball is thick and tough. It provides form and shape to the eyeball. Fibrous coat consists of two parts, the sclera and cornea.
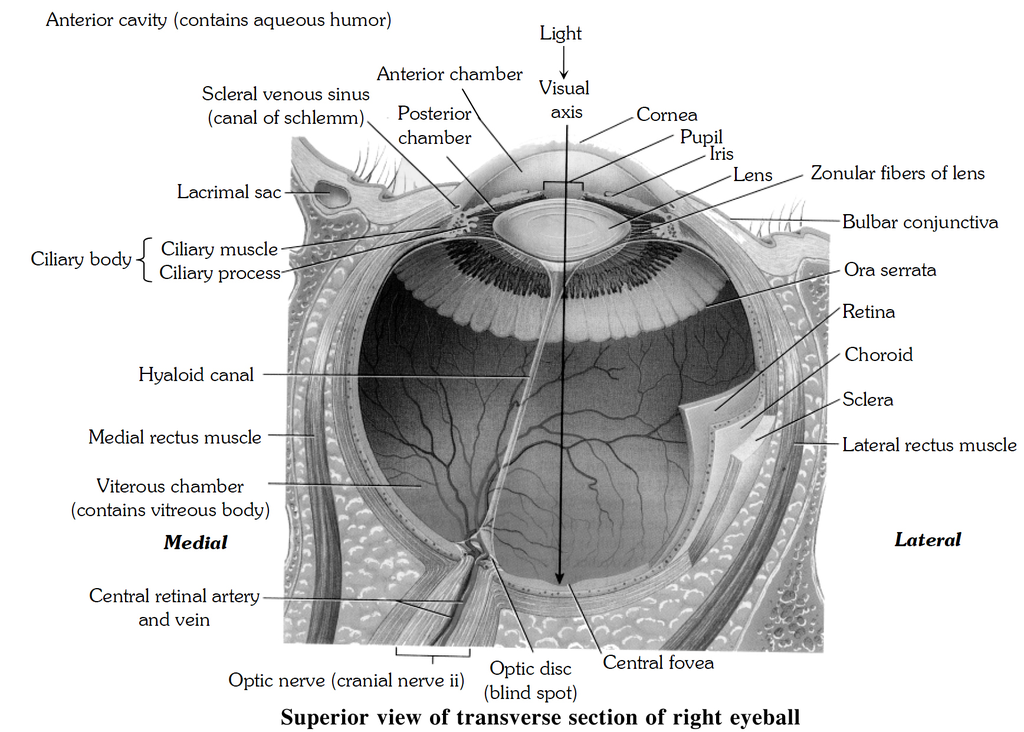
Sclera constitutes about five-sixth of the outer coat. It is white (made up of tough but elastic sheath of fibrous connective tissue containing collagen fibres) and opaque, and popularly called white of the eye. Most part of sclera is concealed in the orbit.
Cornea is the anterior transparent part of sclera and constitutes about 1/6 th of the fibrous coat. It is non-vascular and convex anteriorly. The cornea is covered by a thin and transparent membrane called conjunctiva composed of stratified epithelium and continued over the inner surface of the lids.
(ii) Vascular coat:
The middle coat of the eyeball is differentiated into three regions namely choroid, ciliary body and iris.
(a) Choroid is delicate, highly vascular and pigmented part which lies in contact with the sclera. It provides dark colour to the interior of the eyeball, it is black in colour. It prevents internally reflected light within the eye. The blood vessels of choroid nourish the retina.
(b) Ciliary body. It is the part of vascular coat immediately behind the peripheral margin of the iris. Ciliary body is thicker and less vascular than choroid. Its inner surface is folded to form ciliary processes. Present within the ciliary body are ciliary muscles.
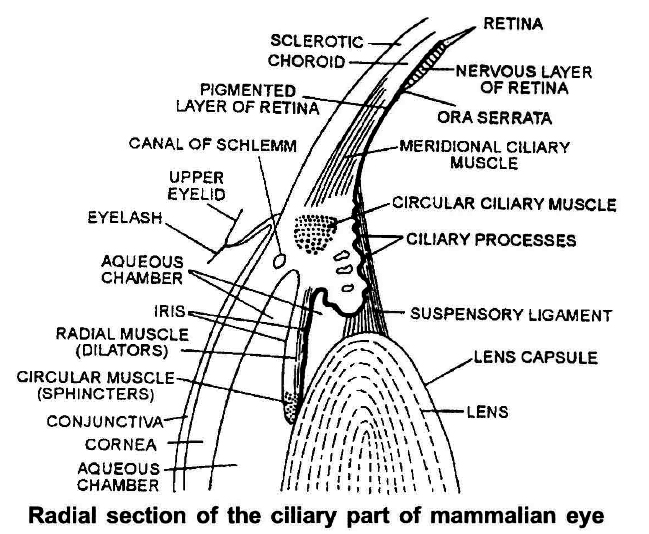
(c) Iris is the anterior part of vascular coat which lies behind the cornea. It is centrally perforated by pupil, the size of which is regulated by the iridial muscles arranged in radial and circular manner. The iris, being pigmented, provides colour to eye.
Concept Builder
Mirror like tapetum layer of carnivores like cats, dogs increases sensitivity by reflecting unabsorbed light back through photoreceptor layer to shine in dark.
(iii) Retina (Nervous Tunic):
The third and inner coat of the eyeball, the retina (nervous tunic), lines the posterior three-quarters of the eyeball and is the beginning of the visual pathway.
The optic disc is the site where the optic nerve exits the eyeball.
Bundled together with the optic nerve are the central retinal artery, a branch of the ophthalmic artery, and central retinal vein.
Branches of the central retinal artery fan out to nourish the anterior surface of the retina.
The central retinal vein drains blood from the retina through the optic disc.
The retina consists of a pigment epithelium (nonvisual portion) and a neural portion (visual portion).
The pigment epithelium is a sheet of melanin-containing epithelial cells that lies between the choroid and the neural portion of the retina some histologists classify it as part of the choroid rather than the retina.
Melanin in the choroid and the pigment epithelium absorbs stray light rays, which prevents reflection and scattering of light within the eyeball.
This enables that the image cast on the retina by the cornea and lens remains sharp and clear.
The pigmented layer is continuous over choroid, ciliary body and Iris while the nervous layer terminates just before ciliary body.
This point is called Orra serrata.
Albinos lack melanin pigment in all parts of the body, including the eye.
The neural portion of the retina is a multilayered out-growth of the brain.
It processes visual data extensively before transmitting nerve impulses to the thalamus, which then relays nerve impulses to the primary visual cortex.
Three distinct layers of retinal neurons, are separated by two zones where synaptic contacts are made, the inner and outer synaptic layers.
The three layer of retinal neurons, in the order in which they process visual input, are the photoreceptor layer, bipolar cell layer, and ganglion cell layer.
Note that light passes through the ganglion and bipolar cell layers before reaching the photoreceptor layer.
Two other types of cells present in the retina are called horizontal cells and amacrine cells. These cells form laterally directed pathways that modify the signals being transmitted along the pathway from photoreceptors to bipolar cells to ganglion cells.
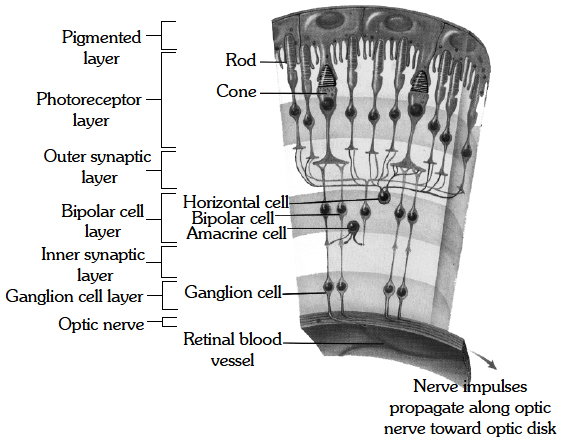
retina and main structures therein.
Photo receptors are specialized to transduce light rays into receptor potentials.
The two types of photoreceptors are rods and cones.
Each retina has about 6 million cones and 120 million rods.
Rods are most important for seeing shades of gray in dim light.
They also allow us to see shapes and movement.
Cones provide color vision in bright light.
The visual pigments for colour vision are: erythropsin (sensitive to red), chloropsin (sensitive to green) and cyanopsin (sensitive to blue).
In moonlight we cannot see colors because only the rods are functioning.
Due to the low light level cones are not functioning.
The macula lutea is in the exact center of the posterior portion of the retina, at the visual axis of the eye.
The central fovea, a small depression in the center of the macula lutea, contains only cone photoreceptors.
In addition, the layers of bipolar and ganglion cells, which scatter light to some extent, do not cover the cones here; these layers are displaced to the periphery of the fovea.
As a result, the central fovea is the area of highest visual acuity or resolution (sharpness of vision).
Rods are absent from the fovea and macula and increase in number towards the periphery of the retina.
From photoreceptors, information flows to bipolar cells through the outer synaptic, layer and then from bipolar cells through the inner synaptic layer to ganglion cells.
The axons of ganglion cells extend posteriorly to the optic disc and exit they eyeball as the optic nerve.
The optic disc is also called the blind spot.
Since it contains no rods or cones.
Accomodation
Accommodation (focussing) is the reflex mechanism by which light rays from objects at various locations in the near visual field are brought to focus on the retina.
Altering the shape of the lens does this. In bright light the circular muscle of the iris contracts, the radial muscle relaxes, the pupil becomes smaller and less light enters the eye, preventing damage to the retina.
In dim light, the opposite muscular contractions and relaxations occur.
In the dark of night", your pupil may become up to 16 times bigger.
The added advantage of reducing the pupil size is that it increases the depth of focus of the eye, so that any displacement of the photosensors in the retina will not impair the focus.
Light rays from distant objects (>6 metres) are parallel when they strike the eye.
Light rays from near objects (<6 metres) are diverging when they reach the eye.
In both cases, the light rays must be refracted or bent to focus on the retina and refraction must be greater for light from near objects.
The normal eye is able to accommodate light from objects from about 25 cm to infinity.
With the involuntary ciliary muscles at rest, the flatter lens has the correct optical properties to focus distant images on the retina, but not close images.
The state of contraction of the ciliary muscles changes the tension of suspensory ligaments.
This acts on the natural elasticity of the lens, which causes it to change its radius of curvature, and thus, the degree of refraction.
As the radius of curvature of the lens decreases it becomes thicker, round up and amount of refraction increases.
It is the tension of the suspensory ligaments applied to the lens which determines the shape of the lens.
When the circular ciliary muscles are relaxed and the suspensory ligament becomes tout, the lens is pulled into a flattened shape suitable for focussing distant objects, decreasing the refraction.
When the tension is decreased, the circular ciliary muscles are contracted and the suspensory ligaments slack, consequently the lens becomes a more spherical shape suitable for focussing objects.
The image produced by the lens of eye on the retina is inverted and reversed.
However, objects are perceived the right way up because of the way in which the brain interprets the images.
The region of the environment from which each eye collects light is called the visual field.
Since both our eyes are frontally placed, there is an overlap between the visual fields of each eye. This is called binocular vision.
Concept Builder
Image formation is refractive process, maximum refraction takes place on cornea.
Extra ocular muscle of eye
Eye is rotated in the orbit by six strap shaped muscles inserted on the sclera. These are arranged in two groups, rectus and oblique.
Rectus: Superior rectus – Oculomotor nerve
Inferior rectus – Oculmotor nerve
Internal (medial) rectus – Oculomotor nerve
External (lateral) rectus – Abducens nerve
Oblique: Superior oblique – Trochlear nerve
Inferior oblique – Oculomotor nerve
CHAMBERS OF EYEBALL
The lens and suspensory ligament divide the interior of eyeball into two chambers, the anterior small aqueous chamber containing a watery fluid, the aqueous humour; and the posterior larger vitreous chamber containing viscous fluid, the vitreous humour.
Aqueous humour maintain intra ocular pressure mainly where as vitreous humour responsible for shaping of eye ball.
Mechanism of Vision
Light rays in visible wavelength focussed on the retina
3
Activation of photopigment of rods and cones
3
Light induces dissociation of the retinal form opsin resulting in the changes in the structure of the opsin.
3
Membrane permeability of rods and cones changes.
3
Potential difference generated in the photoreceptor cell.
3
If generate action potential in the ganglionic cell s through the bipolar cells.
3
Action potentials are transmitted by the optic nerve to the visual cortex of brain.
3
Image formed on the retina is recognised based on earlier memory and experience.
Protective devices of Eye
(1) The Eyebrows: Two arched eminences of skin having numerous hairs project obliquely from the surface of the skin. The function of the eyebrows is to protect the anterior aspect of the eyeball from sweat, dust and other foreign bodies.
(2) The Eyelids (Palpebrae) and Eyelashes: The eyelids are two movable folds and have on their free edges, hairs -the eyelashes. The third eyelid is vestigial and is called plica semilunaris (nictitating membrane). The inner surface of each eyelid and parts of the eyeball are covered with mucous membrane, called the conjunctiva.
(3) Glands of Zeis: These are modified sebaceous glands which are associated with the follicles of eye lashes. They open into the follicles of eye lashes. Meibomian or tarsal glands are also modified sebaceous glands (oil glands) which are present along the edges of the eyelids. They produce an oily secretion which serves to lubricate the corneal surface and hold a thin layer of tears over the cornea. Glands of Moll are modified sweat glands at the edge of the eye lid.
(4) Conjunctiva: The palpebral conjunctiva is very vascular and has numerous papillae. Over the sclera the ocular conjunctiva is loosely connected to the eye ball; here it is thin, transparent, without papillae and slightly vascular. Reaching the cornea it continues as the corneal epithelium. The epithelium of the palpebral conjunctiva near the margin of the lids is non-keratinized squamous stratified epithelium. The conjunctiva helps to protect the eye ball and keeps it moist. It is this membrane that becomes inflamed in conjunctivitis or "pink eye".
(5) The Lacrimal Apparatus: The lacrimal apparatus of each eye consists of a lacrimal gland and its numerous ducts, the superior and inferior canaliculi, a lacrimal sac and nasolacrimal duct. The lacrimal gland secretes tears which are composed of water, salts and bactericidal protein called lysozyme. Lysozyme destroys microorganisms present on the front of the eyeball.
(6) Adipose Tissue (fat):A layer of adipose tissue surrounds the eyeball in the orbit. It serves as soft, shockproof pad.
Disorders of Eye:
(1) Myopia or Nearsightedness : In this case, the eyeball is antero-posteriorly elongated so that the image of distant objects is formed in front of yellow spot. The defect can be removed by using concave glasses.
(2) Hypermetropia or Long sightedness : The person can see distant objects clearly, but not those which are closer. This is due to antero-posterior shortening of the eyeball, so that the image is formed behind the yellow spot. The defect can be overcome by using convex lens.
(3) Presbyopia : A common defect in old age people due to the loss of elasticity of lens and reduced power of accomodation. The disorder can be corrected by convex lenses.
(4) Astigmatism : The disorder due to rough curvature of cornea or lens which can be corrected by the use of cylindrical glasses.
(5) Cataract: The sight is impaired due to the lens becoming opaque (Safaid Motia). The defect can be cured by surgical removal of the defective lens.
(6) Glaucoma: It occurs due to increase in intra-occular pressure as may develop due to blockage of canal of schlemn. It exerts pressure on optic nerve causing its damage. It leads to permanent blindness (Kala Motia)
(THE EARS)
The organs (Phonoreceptors) in man are a pair of ears situated on the head. Apart from their auditory function, the ears are also the organs of balancing.
Each ear has three portions-the external ear, the middle ear and internal ear.
(1) External Ear:
It consists of pinna and external auditory canal.
The latter is a curved passage which is lined by profusion of hair and about 4,000 ceruminous glands.
The glands secrete cerumen, a waxy material which entraps dust and also lubricates tympanum.
Tympanum or ear drum is a circular membrane present on the inner end the external auditory canal and partitions it from the tympanic cavity.
(2) Middle Ear:
The middle ear is represented by air-filled tympanic cavity which communicates with the pharynx by a passage called eustachian canal.
Present in the inner wall of the tympanic cavity are two openings, the upper fenestra ovalis and the lower, fenestra rotunda, each covered by a membrane.
The tympanic cavity contains three small bones, the ear ossicles which from outside to inside include malleus, incus and stapes.
Malleus is hammer shaped; incus is anvil shaped and the stapes is stirrup shaped.
The outer arm of malleus is in contact with inner surface of tympanum, while the inner end of stapes forms contact with the membrane on fenestra ovalis.
Middle ear is responsible for amplification of signal due to leverage system of ossicle (10 times) by ear ossicles and 2.2 times by smaller size of membrane covering fenestra ova lis. The oval window is the door to internal ear.
(3) Internal Ear:
It is also called membranous labyrinth and is surrounded by bony labyrinth of almost similar shape.
The space between the membranous labyrinth and bony labyrinth is filled by a watery fluid, the perilymph.
The membranous labyrinth contains endolymph.
The internal ear is a delicate organ and differentiated into vestibule, semicircular canals and cochlear duct.
The vestibule is the central body and is formed of two chambers, the upper utriculus and the lower sacculus.
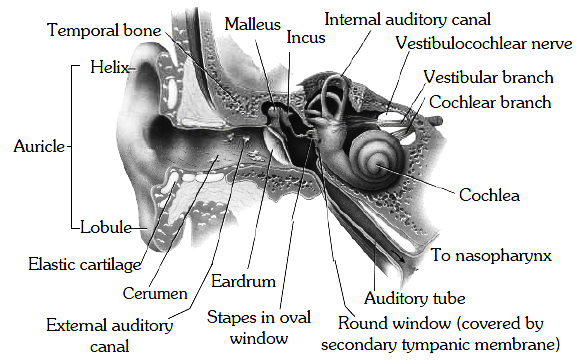
Semicircular canals are three arched structures which emerge from utriculus and open back into it.
They include anterior and posterior vertical canals and a horizontal canal.
The vertical canals join to form a common passage crus commune, before they open into utriculus.
Each semicircular canal is dilated at the base to form ampulla which contains sensory spot called crista formed of receptor cells and supporting cells.
The receptor cells bear sensory hair, which are embedded into a gelatinous cupule above.
The vestibule also contains two sensory spots called maculae, one in sacculus and another in utriculus.
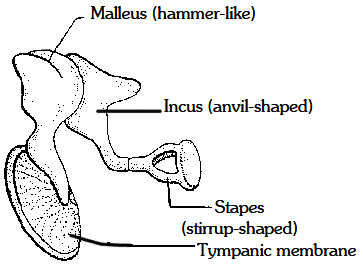
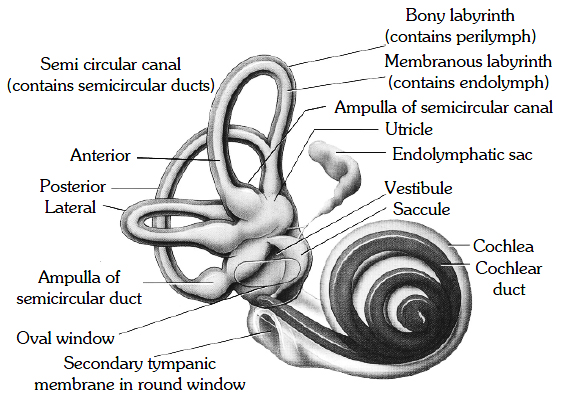
Maculae are similar to cristae, but there is no cupule.
The sensory hair are embedded in otolith membrane containing calcareous bodies called otoliths.
The cristae and maculae are the receptors of balance.
The auditory region of intern al ear is represented by a spirally coiled structure called cochlea.
It consists of cochlear duct arising from the sacculus, which is surrounded by similarly shaped cochlear canal, a part of bony labyrinth.
The cochlear duct is fused with cochlear canal on lateral sides, but is free laterally therefore, in T.S., the cochlea shows three chambers, the upper scala vestibuli, the middle scala media and the scala tympani.
The scala media is partitioned from the scala vestibuli by Reissner's membrane and from the scala tympani by basilar membrane.
Scala vestibuli and scala tympani contain perilymph while scala media is filled with endolymph.
The upper and lower chambers communicate through helicotrema, a narrow opening present at the distal end of cochlea.
The basilar membrane, sensory hair cells and tectorial membrane make up the smallest unit of the ear, called the organ of Corti, first described by Italian microscopist, Alfonso Corti (1822-1888).
Sensory hair cells inside the ear resemble tracts left in the sand by truck tires.
The cochlea contains 16,000 to 24,000 hair cells arranged in four rows.
In three of the rows, the hairs form V-shaped patterns. In the fourth row, the hair stand in a straight line.
Each hair cell has up to 100 hairs.
When sound vibrations pass through the oval window, they create waves in the lymph fluid of the cochlea, like sea wave in a tidal current.
The waves cause the basilar membrane to ripple.
This movement bends the hair cells, pressing against the tectorial membrane and setting off nerve impulses in their associated afferent neurons.
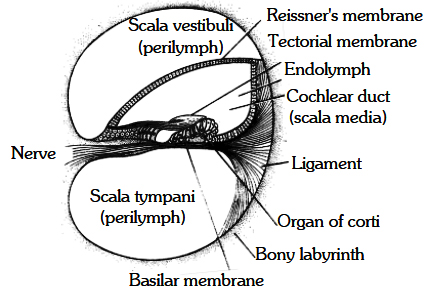
More than 30,000 neurons and nerve fibres emerging from these, convey the electrical Signals to the brain, just 2 cm away via auditory (vestibulocohlear) nerve.
The basal ends of hair cells synapse with fibres of cochlear branch.
When the waves reach the round windows of the cochlea, they die away.
Mechanism of Hearing
External ear receives sound waves
3
Directed towards the ear drum
3
When the waves strike the tympanicmembrane the alternate compression and
decompression of the air causes the membrane to vibrate
3
Vibrations are transmitted through the ear ossicles (M -7 I -7 S) to oval window
3
The movement of the oval window set up wave in the perilymph of scala vestibuli
3
Vibration of endolymph of scala media
3
The waves in the endolymph induced a ripple in the basilar membrane
3
Basilar movements bend the hair
cells pressing them against the tectorial membrane
3
Nerve impulse generated in the associated afferent neurons
3
Impulse transmitted to auditory region of brain via auditory nerve
3
Impulse get analysed and sound is recognised
Concept Builder
The high frequency resonance of the basilar membrane occurs near the base, where the sound waves enter the cochlea while low frequency resonance occurs near the apex mainly because of stiffness of fibres of basilar membrane.
The three internal ossicles of ear are malleus incus and stapes.
In case of non-mammals (amphians, reptiles, birds) there is just one bone called columella auris.
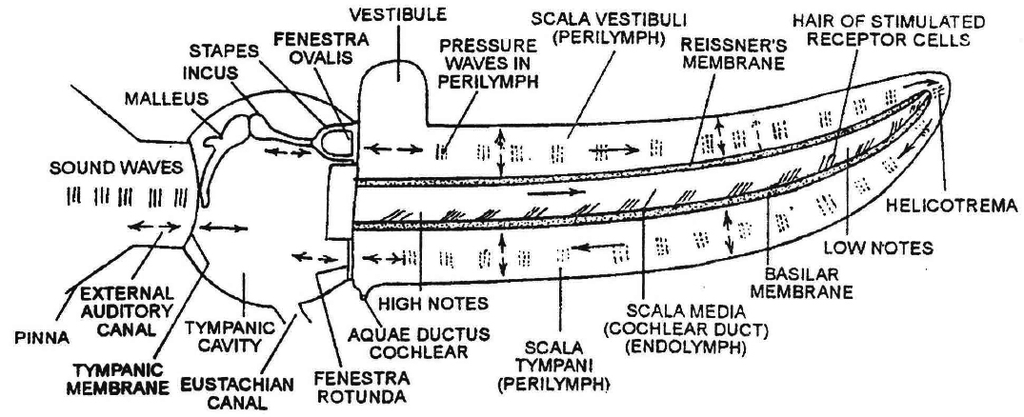
Physiology of Equilibrium
There are two kinds of equilibrium (balance).
One, called static equilibrium, refers to the maintenance of the position of the body (mainly the head) relative to the force of gravity.
The second king, dynamic equilibrium, is the maintenance of body position (mainly the head) in response to sudden movements such as rotation, acceleration, and deceleration.
Collectively, the receptor organs for equilibrium are called the vestibular apparatus, which includes the saccule, utricle, and semicircular ducts.
Static Equilibrium
The wall of both the utricule and saccule contains a small, thickened region called macula (Pleural maculae).
The maculae are the receptors for static equilibrium and also contribute to some aspects of dynamic equilibrium.
For static equilibrium they provide sensory informations on the position of head and essential for maintaining appropriate posture and balance.
For dynamic equilibrium they linear acceleration and deceleration.
For example the sensation you feel while in an elevator or a car that is speeding up or slowing down.
Dynamic Equilibrium
Vestibular apparatus contains three semicircular canals positioned at right angles to one another.
The dilated portion of each duct, ampulla, contains a small elevation called the crista.
Each crista is composed of a group of hair cells, supporting cells covered by a mass of gelatinous material called the cupula.
The cristae in the three semicircular canals maintain dynamic equilibrium.
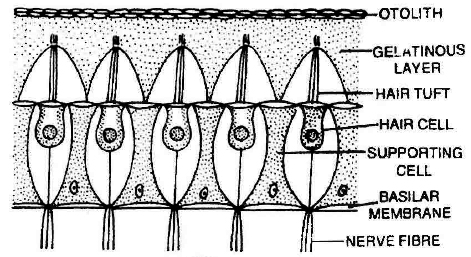
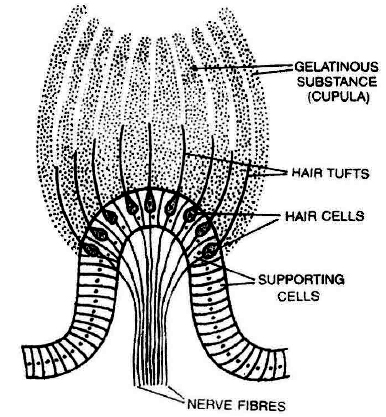
Diseases of the Ear
1. Meniere's diseases: due to increased amount of the fluid of internal ear, loss of hearing.
2. Myringitis: Inflammation of tympanic membrane.
3. Otitis media: Acute infection in middle ear.
4. Vertigo: Type of dizziness where there is feeling of motion when one is stationary.
5. Cobyrinthine diseases: Improper functioning of internal ear.
Some Important Points
1. Most domestic mammals and sharks lack colour vision.
2. Tapetum lucidum. It is a part of choroid adjacent to the retina in the eyes of large number of elasmobranchs (cartilaginous fish). It possesses cells containing light-reflecting guanine crystals. It reflects light and causes the eyes to shine in dark. It also reflects additional light on the retinal cells to enable the fish to see in water where light is poor.
3. Accommodation : Fishes are able to see objects at different distances by changing the size of eyeball.
4. Pecten. It is a remarkable, highly vascular and pigmented structure projecting into the vitreous chamber from the blind spot normally. The pecten occurs in all birds except Kiwi (Apteryx). It is also found in some reptiles (e.g. Uromastix) but is absent in mammals. In Uromastix it is like cushion however, in pigeon it is comb-like and folded like a fan. The actual function of pecten is unknown but possibly it aids in the nutrition of the eye ball. In birds, it also helps in accommodation which is remarkably will developed in birds, by pressing the lens forward.
5. Phaco-emulsification technique in cataract surgery -"stitchless" technique. Foldable IOL (intraocular lens) is used.
6. Most birds have only day vision as their retina has mainly cones.
7. Owls have much better night vision as they contain a large number of rods and few cones in their retina.
8. Taste of chillies, is not true sensation. It is mainly sensation of burning pain produced by the stimulation of pain receptors of the tongue.
9. Hordeolum. Inflammation of sebaceous glands of eye lid.
10. Owls and cats see only with the help of available light from the stars or moon at night.
11. Frog is short sighted in air and long sighted in water.
12. Many insects like honeybees possess the gustatory receptors on their feet.
13. Largest cranial nerve-Trigeminal. .
14. Smallest/Thinnest cranial nerve-Pathetic/Trochlear.
15. Other names of various parts of brain
(i) Fore Brain = Prosencephalon
(ii) Mid Brain = Mesencephalon
(iii) Hind Brain = Rhombencephalon
(iv) Olfactory lobes = Rhinencephalon
(v) Cerebrum = Telencephalon
(vi) Diencephalon = Thalamencephalon
(vii) Cerebellum and Pons = Metencephalon
(viii) Medulla oblongata = Myelencephalon
(ix) Fourth ventricle = Metacoel
(x) Third ventricle = Diocoel
(xi) Iter = Mesocoel and aqueduct of sylvius.
(xii) Lateral ventricle = Paracoel
(xiii) Spinat canal = Myelocoel
(xiv) Cavity of olfactory lobe = Rhinocoel (absent in human)
16. Origin of CNS-develops from neural tube that is formed by infolding of ectoderm in early embryo.
17. Neopallium-Dorsal wall of cerebrum/cerebral cortex of brain.
18. Monosynaptic/simple reflex involves a single sensory fibre and a single motor fibre e.g., knee jerk. No interneuron. Polysynaptic/compound reflex involves one (or more) sensory and more than one motor nerve fibres. A number of interneurons are present. Polysynaptic reflexes are more common. All our visceral reflexes are polysynaptic
Endocrine glands and endocrine system
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
Endocrine glands and Endocrine system
Endocrine glands (Gr., endo = within + krinein = to secrete):
These glands lack ducts and pass secretions into the surrounding blood directly. Therefore they called ductless glands. e.g. – Thyroid, parathyroid, adrenal, pituitary, pineal body and thymus.
Endocrine system:
the work of co-ordination by endocrine system is slowly by secretion of some chemical substances.
Hormones are secreted in blood
Virtually all body cells
Change in metabolic rate
Seconds to hours or days generally long.
Pituitary and pineal gland
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
Pituitary and Pineal Gland
PITUITARY GLAND
It is pink coloured pea-sized gland about 1.3 cm in diameter and weighs only 0.5 g.
It is located in a bony cavity called sella turcica of sphenoid bone and is attached to hypothalamus via infundibulum.
The pituitary gland has two anatomically and functionally separate lobes, the much larger anterior lobe or adenohypophysis and posterior lobe or neurohypophysis.
Adenohypophysis consists of two portions pars distalis and pars intermedia.
The pars distalis produces cluster of hormones whereas pars intermedia secretes only one hormone called melanocyte stimulating hormone (MSH).
However in humans the pars intermedia atrophies and merges with pars distalis during foetal development.
Hormones of Pituitary Gland and their Action on Target Organs
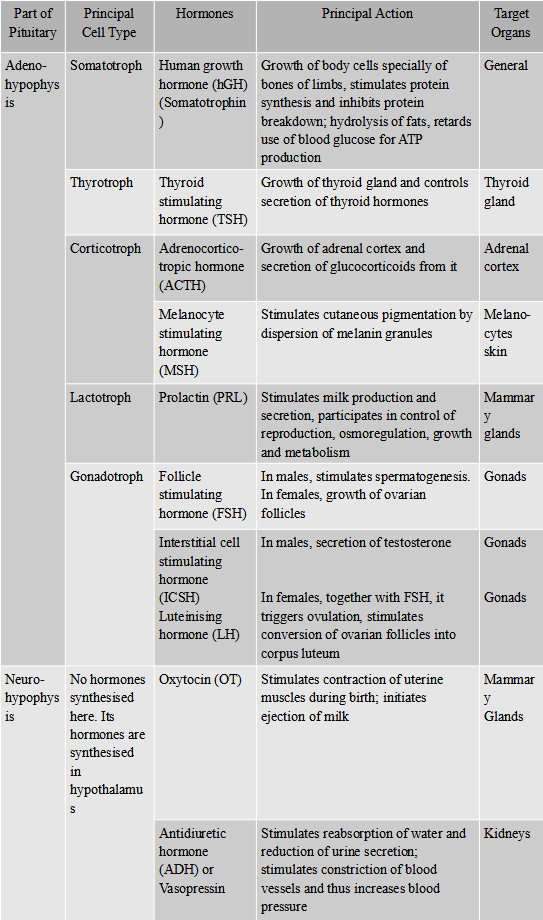
Concept Builder
1. GH is the only adenohyophysis hormone which is linked directly to body whereas other adenohypophysis hormones mostly control other glands.
2. GH stimulates hepatocytes to release glucose into blood. In this respect GH is an insulin antagonist and thus can be related to have diabetogenic effect.
3. Pitocin is synthetic oxytocin which is often given to induce labor.
Pineal Gland
Pineal gland is regarded as vestige of third eye as well as functional endocrine gland.
It is attached to the roof of third ventricle in the rear portion of brain, ectodermal in origin is known as the pineal gland, named for its resemblance to a pine cone.
It has no direct connection with central nervous system.
It is variable in size and weighs about 150 mg, but is richly vascularised and secretes several hormones, including melatonin.
In humans, it has no light-sensitive cells, like lower vertebrates, where pineal is eye-like and responds to light.
Pineal gland functions as a biological clock and a neurosecretory transducer, converting neural information.
More melatonin is produced during darkness.
Its formation is interrupted when light enters the eyes and stimulates the retinal neurons.
They transmit impulses to the hypothalamus, and finally to the pineal gland.
The result is inhibition of melatonin secretion.
In this way, the release of melatonin is governed by the diurnal dark-light cycle.
Melatonin also influences body temperature, metabolism, pigmentation, menstrual cycle and defense capability.
Thyroid gland and Parathyroid gland
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
Thyroid Gland and Parathyroid Gland
THYROID GLAND
It is larget butterfly shaped endocrine organ situated in the neck close to the trachea.
The gland consists of two elongated oval lobes joined by a narrow band called isthmus.
It is a highly vascular organ and contains many spherical or oval sac-like follicles.
Cells lining the thyroid follicle; secrete, two thyroid hormones, thyroxine or tetraiodothyronine (T4) and triiodothyronine (T3).
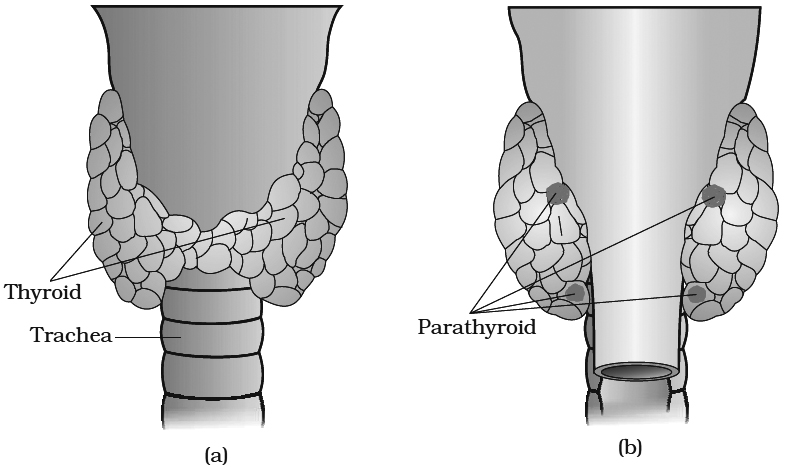
(a) Dorsal side (b) Ventral side
Both are iodinated forms of an amino-acid called tyrosine and remain stored in the jelly like semifluid material (colloid) in the lumen of follicles.
T3 is more active and several times more potent than T4.
From the thyroid mainly T4 is secreted and converted to T3 in peripheral tissues e.g., Liver.
Thyroid is the only endocrine gland which stores its secretory product in large quantity also involve in iodine metabolism.
When necessary, the hormones are released from the colloid to the blood.
In between thyroid follicle are present C-cell or parafollicular cells which release calcitonin (TCT) or parafollicular hormone.
It is involved in calcium homeostasis.
It is hypocalcemic and hypophosphatemic.
Both parathormone and calcitonin help in the maintenance of calcium ions in blood plasma.
Functions:
1.Thyroid hormones greatly increase the metabolic rate of the body and consequently, enhance heat production (Calorigenic effect) and maintains BMR (basal metabolic rate).
2.Thyroid hormones also promote growth of body tissues-both physical growth and development of mental faculties are stimulated.
3.They stimulate tissue differentiation. Because of this action, they promote metamorphosis of tadpoles into adult frogs.
4.To enhance some actions of neurotransmitters : adrenaline and nor-adrenaline.
5.Support process of red blood cells formation.
6.Maintenance of water and electrolyte balance is also influenced by thyroid hormones.
Disorders Due to Thyroid Hormone Imbalances
Hypothyroidism
It can develop due to inactivity of thyroid itself or hyposecretion of TRH or TSH or insufficient dietary intake of iodine.
1.Cretinism:
Failure of thyroid secretion from infancy or childhood slows body and mental development and reduces metabolic rate markedly.
The child remains physically stunted and mentally retarded low intelligence quotient, abnormal skin deaf mutism.
The body temperature, heart rate and blood pressure lower than normal.
The patient is pot-bellied and pigeon chested and has a protruding tongue.
Other features include neonatal jaundice, lethargy, respiratory problems and constipation.
This disease is called cretinism.
Normal growth and development may be restored in certain cases by an early administration of thyroid hormones.
2.Myxedema (Gull's diseases):
Deficiency of thyroid hormones produces myxedema in adults.
The patient has a puffy appearance and lacks alertness, intelligence and initiative.
The patient also suffers from low metabolic rate, slow heart rate, low body temperature and reproductive failure.
Administration of thyroid hormones cures the symptoms. it occurs more commonly in females.
3.Simple Goitre:
In mountainous regions, the dietary deficiency of iodine frequently produces thyroid enlargement (Iodine Deficiency Goitre), accompanied by cretinism or myxedema.
Hyperthyroidism
Exophthalmic Goitre:
In Graye's disease or Exophthalmic goitre, a thyroid enlargement (goitre) is accompanied by a bulging of eyeballs (exophthalmos).
The enlarged thyroid is overactive and secretes excessive amount of thyroid hormones.
So, the goitre is associated with symptoms of thyroid overactivity such as high metabolic rate, rapid heart rate, rise in body temperature, emaciation, nervousness, irritability, tremor and restlessness.
It also occurs more often in females.
It is an autoimmune disorder in which the person produces antibodies that mimic the action of TSH, but are not regulated by normal negative feed back control.
PARATHYROIDS GLAND
These are four small pea sized glands situated very close to the thyroid.
They secrete a hormone called parathormone (Collip's hormone).
They are under the feedback control of blood calcium level.
A fall in blood calcium stimulates them to secrete parathormone, a rise in blood calcium inhibits parathormone secretion from them.
Parathormone increases the concentration of calcium ions in the blood plasma, because it mobilises more calcium from the bones to the plasma and reduces urinary elimination of calcium.
It is secreted whenever the plasma Ca2+ concentration falls and restores the Ca2+ concentration to normal in the plasma.
On the other hand, it increases phosphate elimination in the urine and consequently lower the phosphate concentration in the plasma.
Thus, parathormone regulates the metabolism of calcium and phosphorus.
Calcium Homeostasis:
(i) A higher than normal level of calcium ions (Ca2+) in blood stimulates parafollicular cells of the thyroid gland.
(ii) They release more calcitonin as blood Ca2+ level rises.
(iii) Calcitonin promotes deposition of blood Ca2+ into the matrix of bone tissue. This decreases blood Ca2+ level.
(iv) A lower than normal level of Ca2+ in blood stimulates principal cells of the parathyroid gland.
(v) They release more parathyroid hormone (PTH) as blood Ca2+ level falls.
(vi) PTH promotes release of Ca2+ from bone matrix into the blood and retards loss of Ca2+ in the urine. These actions help raise the blood level of Ca2+.
(vii) PTH also stimulates the kidneys to release another hormone called calcitriol.
(viii) Calcitriol stimulates increased absorption of Ca2+ from foods in the gastrointestinal tract, which helps increase the blood level of Ca2+.
DISORDER OF PARATHYROID
Hypoparathyroidism
Parathyroid Tetany:
If the parathyroids fail to secrete sufficient amount of parathormone, the concentration of calcium ions falls abnormally in the plasma.
This increases the excitability of nerves and muscles due to deficiency of Ca2+ which causes depolarisation without usual stimulus.
Consequently, sustained contractions (tetany) of the muscles of larynx, face, hands and feet are produced.
This disease is called parathyroid tetany.
It can also develop due to accidental damage to the parathyroid or their blood supply during thyroidectomy surgery.
Hyperparathyroidism
The parathyroid tumours secrete excessive amount of parathormone, which causes increased mobilisation of bone minerals into the blood, softening of bones, rise in the concentration of calcium iens in the plasma, and deposition of calcium in kidney tubules and other soft tissues.
It may cause Osteitis Fibrosa Cystica.
Pineal and Thymus gland
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
Thymus and Pineal Gland
Thymus Gland
It is soft bilobed structure where the two lobes lie side by side and joined in the middle by connective tissue.
It is pyramidal in children with maximum size reaching at about 15 years of age.
Its size is reduced somewhat later due to decrease of its lymphoid content.
The weight at birth is 15-20 g in children remaining at that level thereafter.
It is deep red in young age becoming thinner and greyer with age and later yellowing due to infiltration of adipose tissue.
Thymus is covered on the outside by a capsule of loose connective tissue which also penetrates the interior of gland forming septa and irregular lobules.
There is an outer cortex of densely packed thymocytes (or T-lymphocyte lineage) and inner medulla having connective tissue with fewer lymphoid cells.
Balls of flattened epithelial cell called Hassal's corpuscles occur here and there in the medulla.
Thymocytes also occur alongwith some B-lymphocytes.
Hormones produced by the thymus gland is called thymosin.
Thymosin released in the bloodstream has a stimulating effect on the entire immune system.
It promotes proliferation and maturation of T-lymphocytes. It is also called "the throne of immunity", or training school of T-lymphocytes.
Concept Builder
Thymosin play major role in differentiation of T-lymphocytes .which provide cell-mediated immunity. These also promote production of antibodies to provide humoral immunity.
Pineal Gland
Pineal gland is regarded as vestige of third eye as well as functional endocrine gland.
It is attached to the roof of third ventricle in the rear portion of brain, ectodermal in origin is known as the pineal gland, named for its resemblance to a pine cone.
It has no direct connection with central nervous system.
It is variable in size and weighs about 150 mg, but is richly vascularised and secretes several hormones, including melatonin.
In humans, it has no light-sensitive cells, like lower vertebrates, where pineal is eye-like and responds to light.
Pineal gland functions as a biological clock and a neurosecretory transducer, converting neural information.
More melatonin is produced during darkness.
Its formation is interrupted when light enters the eyes and stimulates the retinal neurons.
They transmit impulses to the hypothalamus, and finally to the pineal gland.
The result is inhibition of melatonin secretion.
In this way, the release of melatonin is governed by the diurnal dark-light cycle.
Melatonin also influences body temperature, metabolism, pigmentation, menstrual cycle and defense capability.
Pancreas
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
PANCREAS
Pancreas and its Hormones:
The pancreas comprises both exocrine and endocrine parts. The endocrine part consists of small masses of hormone secreting cells called ISLETS OF LANGERHANS.

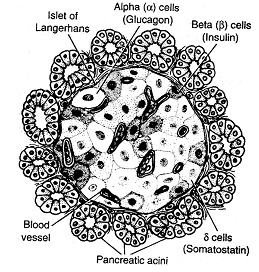
Failure of insulin secretion produces Diabetes mellitus.
In this disease, blood sugar is abnormally high and exceeds the renal threshold for glucose.
Consequently, glucose appears in the urine (glucosuria).
The utilisation of glucose is decreased; instead, catabolism of fats and proteins are enhanced.
Increased oxidation of fat produces ketone bodies such as acetoacetate and acetone.
Also the blood cholesterol rises.
The osmotic effect of glucose in the urine considerably increases the volume of urine (polyuria).
Thirst is enhanced due to urinary loss of water.
Injuries take a long time to heal and may turn into gangrenes.
In extreme cases, the patient suffers from coma and may die.
Administration of insulin reduces the blood sugar and checks other symptoms of diabetes.
Concept Builder
Diabetes Mellitus (Type–I): It is insulin dependent diabetes mellitus (IDDM) and also known as juvenile onset diabetes because it most commonly develops in people younger than 20. It is an autoimmune disorder in which immune system destroys β cells.
Diabetes mellitus (Type–II): It is non insulin dependent diabetes mellitus (NIDDM). It is also known as maturity onset diabetes because it occurs later in life. It arises not from shortage of insulin but because of target cells became less sensitive to insulin.
Testes and ovary
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
Testes and ovary
Testes in males and ovaries in females secrete sex hormones at puberty.
Hypogonadism:
Defects in, or injury to, the hypothalamus, the pituitary, or the testes or ovary, result in hypogonadism.
Male hypogonadism can consist of deficient androgen production (hypofucntion of Leydig cell), deficient sperm formation (hypofunction of sertoli cell), or both, before puberty.
It results in the lack of development of secondary sexual characteristics and male musculature.
Female hypogonadism results from hyposecretion of estrogen, resulting in cessation of reproductive cycles.
Such hypogonadism can result from a shortage of pituitary gonadotropins (LH, FSH or both) or can represent primary testicular/ovary failure.
Precocious puberty:
True sexual precocity, i.e., early maturation of ovaries and testes with production of ova before the age of 9 years in girls, or sperm before 10 years in boys, occurs without evident cause.
Sexual pseudoprecocity results from excesses of sex hormones from the adrenal cortex, testis, ovary or from other sources, including extragonadal tumours.
Sexual pseudoprecocity in boys occurs as a consequence of excess of testosterone produced by tumours of the testis or adrenals.
In such cases, enlargement of the penis, accelerated appearance of sexual characteristics, such as, pubic and axillary hair, masculinisation, faster body growth, and ultimate stunting are present.
Sexual pseudoprecocity in girls arises from increased supply of estrogen secreted by tumours of the ovaries or adrenals.
The external manifestations of sexual maturation, for example, breast formation and appearance of pubic hair, appear early, but the maturation and discharge of ova do not occur.
Hormones Regulating Reproduction
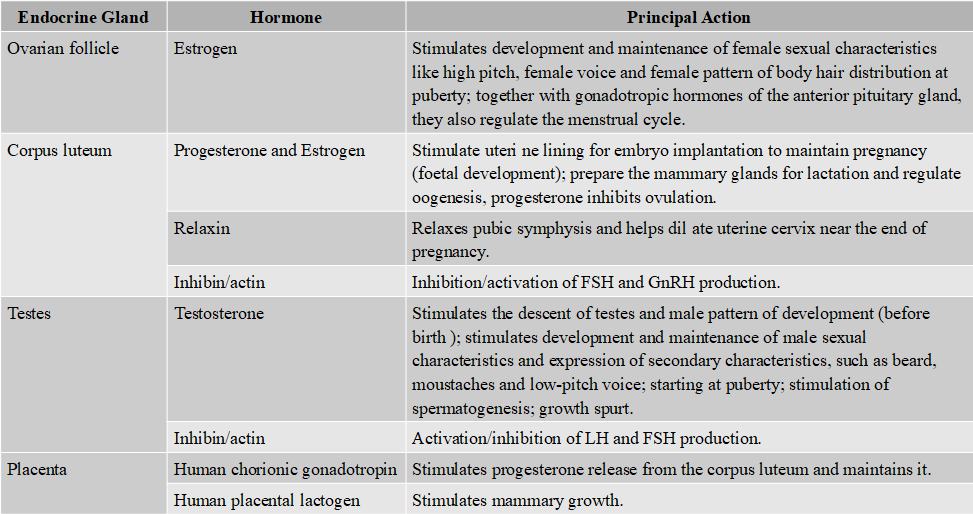
Eunuchoidism:
This results from the failure of testosterone secretion.
For this disorder, secondary sex organs, such as prostate gland, seminal vesicles and penis, remains infantile and small in size and fail to function.
Spermatozoa fail to be produced.
External sex characters like beards, moustaches and low-pitch male voice fail to develop.
Gynaecomastia:
It is the development of breast tissue in males, and is usually due to perturbation of estrogen to androgen ratio.
In the neonatal period and during puberty, gynaecomastia is due to temporary increase in circulating estrogen.
Decreased testosterone in later life may also lead to gynaecomastia.
Removal of testes in male is called castration.
It will lead to decline in the androgen level and secondary characters fail to appear.
It can lead to retention of high pitch juvenile voice in a male.
Hormones of heart, kidney and gastrointestinal tract
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
Hormones of heart, kidney and gastrointestinal tract
In addition to endocrine glands, hormones are also secreted by some tissues which are not endocrine glands.
For example, the atrial wall of heart secretes a very important peptide honnone called atrial natriuretic factor (ANF) which decrease blood pressure.
When blood pressure is increased, ANF is secreted which causes dilation of blood vessels.
This reduces the blood pressure.
Juxta glomerular cells of kidney produces peptide hormone called erythropoietin which stimulates erythropoiesis. (Formation of RBC).
Endocrine cells present in different part of the gastro intestinal tract secrete four major peptide hormones namely gastrin, secretin, cholecystokinin (CCK) and gastric inhibitory peptide (mentioned in animal nutrition).
Mechanism of hormone action
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
Mechanism of Hormone Action
Catecholamines, peptide and protein hormones are not lipid-soluble, and so, cannot enter their target cells through the bilipid layer of plasma membrane.
Instead, these water soluble hormones interact with a surface receptor, usually a glycoprotein, and thus, initiate a chain of events within it.
The hormone insulin provides a well-studied example.
Extracellular Receptor:
The membrane bound receptors of insulin is a heterotetrameric protein consisting of four subunits, two a-subunits protrude out from surface of the cell and bind insulin, and two b-sub-unit that span the membrane and protrude into the cytoplasm.
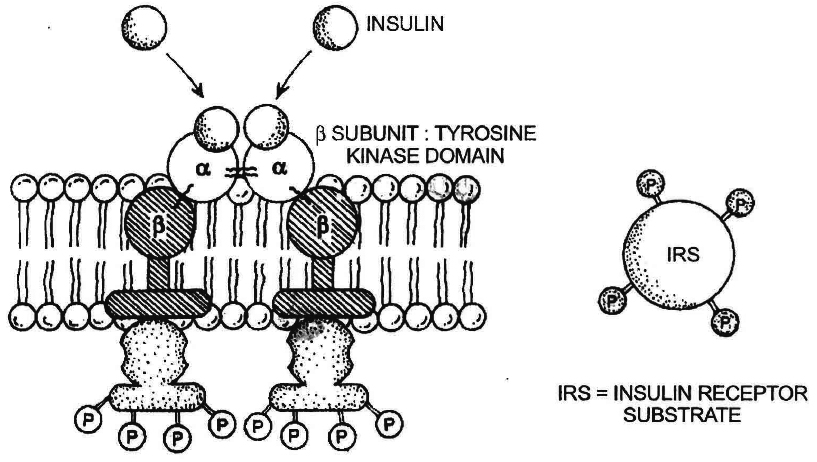
Binding to the receptor:
Binding of insulin to the outer subunits of the receptor causes a conformational change in the membrane spanning b-subunits, which is also an enzyme, a tyrosine kinase.
The activated b-subunits add phosphate groups of specific tyrosine residues located in cytoplasmic domain of the receptor as well as a variety of insulin receptor substrates.
Second messengers-the mediator:
As a result of b-subunit activity, a transducer G-protein activates enzyme phosphodiesterase.
This enzyme breaks phosphatidylinositol 4,5-biphosphate (PIP2) into a pair of mediators: inositoltriphosphate (IP3) and diacylglycerol (DG).
In turn, IP3, which is water-soluble, and so diffuses into cytoplasm and triggers the release of another messenger Ca2+ ions for intracellular calciummediated processes.
While DG remains within the membrane where it activates an enzyme called protein kinase C, which in turn, activates many other enzymes, such as pyruvate dehydrogenase, and so brings about the physiological effects.
Antagonistic effect:
Many cells use more than one second messenger.
In heart cells, cAMP serves as a second messenger, speeding up muscle cell contraction in response to adrenaline, while cyclic guanosine monophosphate (cGMP) serves as another second messenger, slowing muscle contraction in response to acetylcholine.
It is in this way that the sympathetic and parasympathetic nervous systems achieve antagonistic effect on heartbeat.
Another example of antagonistic effect is insulin, which lowers blood sugar level, and glucagon, which raises it.
Synergistic effect:
Another type of hormonal interaction is known as synergistic effect.
Here, two or more hormones complement each other's actions and both are needed for full expression of the hormone effects.
For example, the production, secretion and ejection of milk by mammary gland require the synergistic effect of estrogens, progesterone, prolactin and oxytocin.
Intracellular Receptors:
Unlikely catecholamine and peptide hormones, steroid and thyroid hormones are lipid-soluble hormones and readily pass through the plasma membrane of a target cell into the cytoplasm.
There they bind to specific intracellular receptor proteins, forming a complex that enters the nucleus and bind to specific regulatory sites on chromosomes.
The binding alters the pattern of gene expression, initiating the transcription of some genes (DNA), while repressing the transcription of others.
This results in the production of specific mRNA translation products, proteins and usually enzymes.
The actions of lipid-soluble hormones are slower and last longer than the actions of water-soluble hormones.
These cause physiological responses that are characteristic of the steroid hormones.
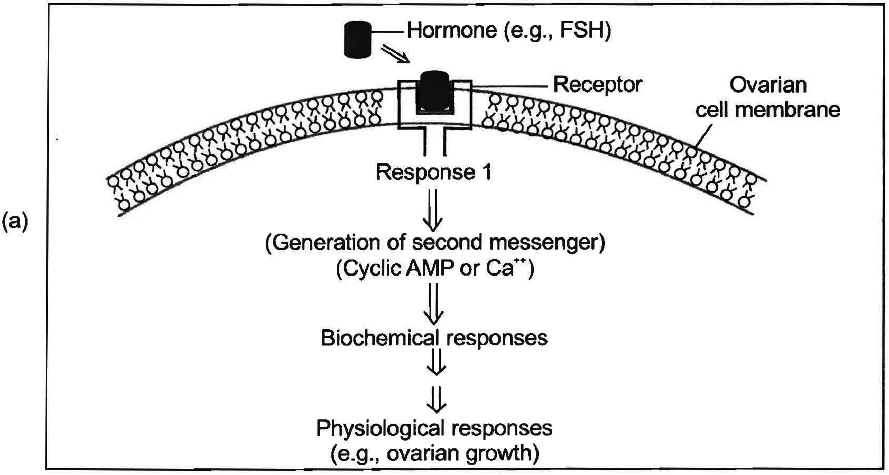
(a) Protein hormone
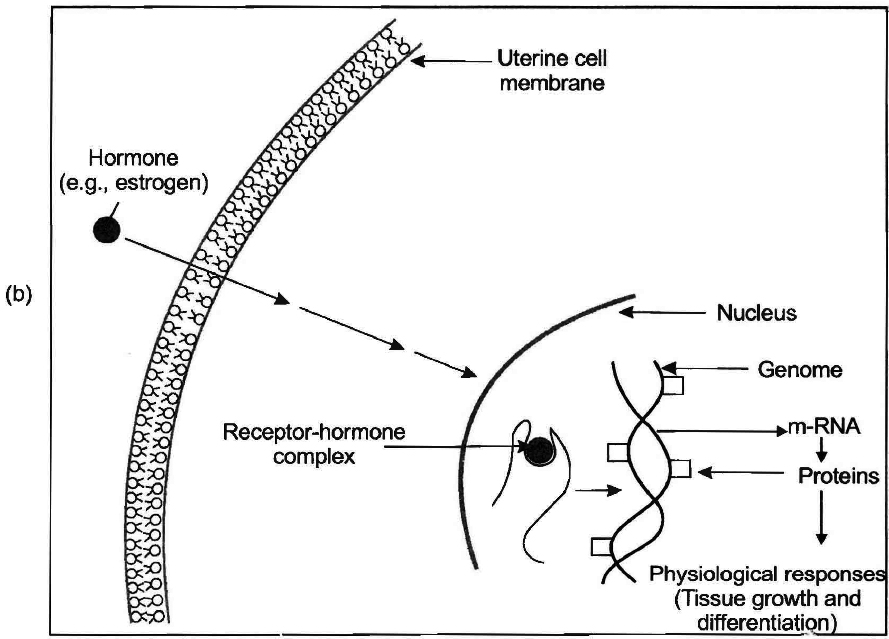
(b) Steroid hormone

 ACME SMART PUBLICATION
ACME SMART PUBLICATION
