Blood
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
BLOOD
Blood is a fluid connective tissue.
Its cells are quite distinct from other connective tissue cells both in structure and functions.
The extracellular material in blood is a fluid devoid of fibres.
Fluids outside the cells are generally called Extracellular Fluids (ECF).
Blood is heavier than water.
The extracellular material in blood is a straw-coloured, slightly alkaline (pH =7.4) aqueous fluid called plasma.
Constituents, having characteristic forms, float in the plasma.
They are collectively called the Formed Elements of blood.
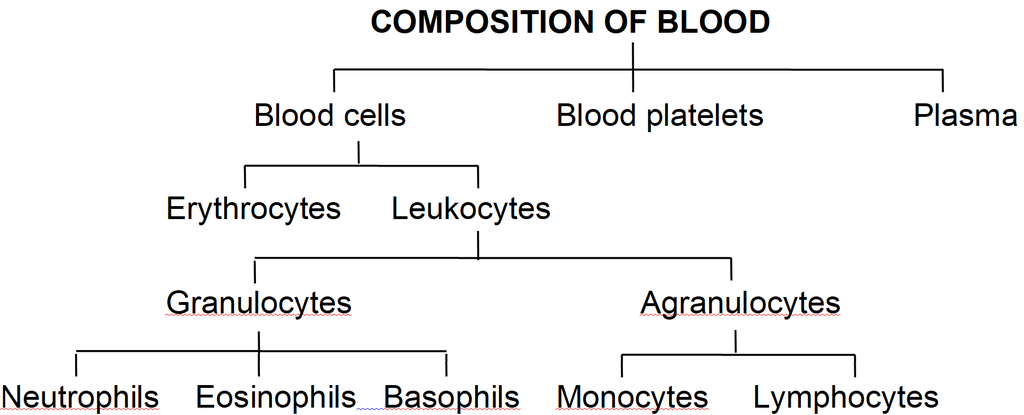
They include the blood cells and blood platelets.
Blood cells are of two types-Erythrocytes and Leukocytes.
Blood circulates within blood vessels in higher animals.
But other extracellular fluids such as cerebrospinal fluid, interstitial fluid, lymph and aqueous humour occur outside blood vessels.
PLASMA
Plasma contains three major classes of plasma proteins viz. serum albumin, serum globulins and fibrinogen.
Plasma proteins serve as a source of proteins for tissue cells.
Tissue cells may utilise plasma proteins for forming their cellular proteins.
Additionally, albumin and globulins retain water in blood plasma by their osmotic effects.
A fall in plasma proteins leads to movement of excessive volumes of water from blood to tissues.
That is why hands and feet get swollen with accumulated fluid (oedema) in persons suffering from dietary deficiency of proteins.
Albumins and globulins also transport many substances such as thyroxine and Fe3+ in combination with them.
One class of globulins, called immunoglobulins, act as Antibodies.
Plasma proteins also maintain the blood pH by neutralising strong acids and bases.
Thus, they act as Acid-Base-Buffers.
It is slightly alkaline non-living inter-cellular substance which constitutes about 60% part of the blood.
It is a pale yellow but transparent and clear fluid.
Composition of Plasma. Plasma forms 55-60% by volume of blood.
1.Water-Water alone forms about 90% to 92% of the plasma. Solids form about 8% of the plasma.
2.Mineral Salts -These are chlorides, bicarbonates, sulphates and phosphates of sodium, potassium, calcium, iron and magnesium. All salts constitute about 0.9% of plasma. Buffer of the blood is sodium bicarbonate.
3.Nutrients - These include glucose, fatty acids, phospholipids, cho'lesterol, fats, aminoacids, nucleosides, etc. Mineral salts have been mentioned above.
4.Plasma proteins -They constitute about 7 to 8% of plasma. These mainly include albumin 4.4% , globulin 1.5 to 2%, prothrombin and fibrinogen both 0.3%.
5.Defence proteins - Immunoglobulins which act as antibodies and some other substances, such as lysozyme and properdin (a large protein) are always found in the plasma. They destroy bacteria, viruses and toxic substances that may enter into the blood from outside.
6.Excretory substances - These include ammonia, urea, uric acid, creatinine, etc.
7.Dissolved gases - Water of blood plasma contains oxygen, carbon dioxide and nitrogen in dissolved form.
8.Anticoagulant - Blood plasma contains a conjugated polysaccharide, heparin which prevents coagulation of blood inside blood vessels.
9.Hormones - These are secreted and released in blood by endocrine glands.
10.Vitamins and Enzymes-Different kinds of vitamins and enzymes are present in the blood plasma.
Functions of Blood plasma-
These can be summarised as under (i) transport, (ii) retention of fluid in blood, (iii) maintenance of blood pH, (iv) body immunity, (v) prevention of blood loss, (vi) conducting heat to skin for dissipation and (vii) uniform distribution of heat all over the body.
Blood Glucose
Glucose is mainly absorbed in the small intestine.
Glucose is also absorbed in the stomach.
After absorption glucose reaches the blood.
Excess of glucose is converted into glycogen by insulin hormone in the liver and muscles.
Whenever it is required, glycogen is changed back into glucose by glucagon hormone.
Usually blood glucose level is about 80-100 mg per 100 ml of blood, 12 hours after a normal meal.
But its concentration rises soon after a carbohydrate rich diet.
If blood glucose level exceeds 180 mg per 100 ml, it starts appearing in urine.
This condition is called glucosuria.
Fasting glucose is 70 -110 mg/dl. Glucose PP1 is 110 -140 mg/dl.
If it is higher, it causes diabetes mellitus (hyperglycemia).
If it is less, it causes hypoglycemia (less amount of glucose in blood).
Blood Cholesterol
Usually cholesterol is considered a harmful substance. But it is quite useful in limited amount.
Cholesterol is used in the synthesis of biomembranes, vitamin D, bile salts and steroid hormones.
Its normal amount is 80 -180 mg in 100 ml of blood plasma.
Cholesterol comes in the blood plasma either by intestinal absorption of fats or by the synthesis from the liver or by both.
Saturated fats such as ghee and butter increase cholesterol level in the blood.
Increased blood cholesterol may lead to its deposition in the internal wall of the blood vessels like arteries and veins which causes high blood pressure and heart problems.
Functions of Plasma Proteins
1. Prevention of blood loss - Fibrinogen and prothrombin playa role in blood clotting.
2. Retention of fluid in the blood - Albumin helps in osmotic balance.
3. Body immunity - Certain globulins called immunoglobulins (glycoproteins) act as antibodies in blood and tissue fluid. Antibodies belong to a class of proteins called as immunoglobulins.
4. Maintenance of pH - Plasma proteins serve as acid-base buffers. It means they maintain pH of the blood by neutralizing acids and bases.
5. Transport of certain materials - Thyroxine (hormone) is bound to albumin or specific globulin for transport in the plasma.
6. Distribution of heat - Plasma proteins help in uniform distribution of heat all over the body.
7. Enzymes - Some proteins acting as enzymes also occur in the plasma.
BLOOD CELLS
(i) Erythrocytes:
Erythrocytes (red blood corpuscles or RBC) are the most numerous of the formed elements of blood.
Their most important characteristic feature is the presence of hemoglobin, the red oxygen carrying pigment.
The total number of erythrocytes per microlitre (1 µl = 1mm3 =10–6) of blood is known as the Total Count of RBC.
It averages 5 millions and 4.5 millions in adult man and adult woman respectively.
The total count would be low in anaemia and after profuse bleeding.
On the contrary, the abnormal rise in the total count of RBC is called Polycythemia.
Anaemia is caused due to the deficiency of folic acid, vitamin B12 and haemoglobin.
The size and shape of erythrocytes vary in different classes of animals.
In fishes, amphibians, reptiles and birds, erythrocytes are usually nucleated, oval and biconvex. But in mammals they are non nucleated, biconcave and circular.
Only camel and llama possess oval red blood corpuscles.
Human erythrocytes measure 7-8 µm (1µm =10–6 m) in diameter and 2 µm thickness near the rim.
Old and damaged erythrocytes are phagocytosed and destroyed by macrophages.
The pigment part (porphyrin) of hemoglobin is then catabolised to the yellow pigment Bilirubin which is excreted in the bile.
The pale yellow colour of plasma is largely due to bilirubin.
If a sample of blood is rendered non-coagulable by adding potassium or sodium oxalate and then centrifuged at a high speed in a graduated centrifuge tube (hematocrit tube), the centrifugal force rapidly sediments the erythrocytes tothe bottom of the tube.
They become packed into a solid, red, bottom layer while plasma forms a clear, fiuid upper layer.
On the upper surface of the erythrocyte layer, leukocytes form a thin, buff-coloured layer.
From the graduations on the tube, the relative volume of erythrocytes may be read as a percentage of the total blood volume. This is called the Hematocrit Value or Packed Cell Volume.
It normally forms 45 percent of the blood volume.
RBC of mammals are circular, biconcave, non-nucleated except family camelidae. e.g. camel, which has non-nucleated and oval RBC. Largest RBCs are found in amphibia.
Smallest RBCs are found in mammals.
In mammals smallest RBCs are found in 'Musk Deer', Tragulus javanicus (1.5 µm).
In mammals, largest RBCs are found in elephant. (9.4 µJ).
Graveyard of RBC is spleen.
Life Span
Life span of RBC in man =120 days
Life span of RBC in frog = 100 days
Life span of RBC of rabbit = 80 days
Radioactive chromium method (Cr51) is used for estimation of life span of RBC.
Count of RBC
In embryo = 8.5 million/mm3
In Man = 5 to 5.5 million/mm3
In Woman = 4.5 million/mm3
Daily destruction of RBC = 1%
ESR (Erythrocyte sedimentation rate) : It is measured by Wintrobe's method. It is rate of settling down of RBC.
It is also estimated by Westergen's method.
ESR is very useful in diagnosing various diseases including tuberculosis, ESR in men is 0-5 mm/hour and in women it is 0-7 mm/hr in Westergen method.
Haemocytometer: It is instrument for counting the number of both WBCs and RBCs.
Rouleaux: In resting and slow flowing blood, the RBCs aggregate to form rouleaux (the RBCs are piled on top of each other). Fibrinogen favours rouleaux formation.
Bone marrow: It is the main site for formation of RBC. Volume of bone marrow at the time of birth is 70 ml. In adult volume of bone marrow is 4,000 ml.
Structure of RBC of man: Biconcave non-nucleated bounded by Donnan's membrane (plasma membrane of RBC). Haemoglobin is filled in RBC which is respiratory pigment.
Normal Range of Hb
Infants 16.5 ± 3.0 g/dl (dl = deciliter)
Children 3 months 11.0 ± 1.5 g/dl
Children 3 to 6 years 12.0 ± 1.0 g/dl
Children 10 to 12 years 13.0 ± 1.5 g/dl
Men 15.5 ± 2.5 g/dl
Women 14.0 ± 2.5 g/dl
Structure of Haemoglobin:
Each molecule of haemoglobin contains 4 molecules of haem and 1 molecule of globin.
These are attached by co-ordinate bonds.
Haem is protoporphyrin compound and has 4 pyrrole groups jointed together to form ring structure.
In Hb, Fe is present in (Fe++) Ferrous form.
Haem is 5% & Globin is 95%. Globin is made of 4 polypeptide chains.
(ii) Leukocytes:
Leukocytes (white blood corpuscles or WBC) are devoid of hemoglobin and are consequently colourless.
Leukocytes are nucleated blood cells.
They are of two major classes : granulocytes (with cytoplasmic granules) and agranulocytes (without granules).
Granulocytes are of three types, viz. neutrophils, eosinophils and basophils, each with lobed nucleus.
Agranulocytesare of two types, viz. lymphocytes and monocytes.
Neutrophils and monocytes protect the body against microbes by phagocytosing them.
Lymphocytes secrete antibodies in the blood to destroy microbes and their toxins.
The number of leukocytes per microlitre (1 µl = 1 mm3 = 10–6) of blood is called the Total Count of WBC.
It is 6000-8000/mm3 of blood normally.
It may rise abnormally in acute infections (e.g., pneumonia), inflammations (e.g. appendicitis) and malignancies (e.g., leukemia).
In some conditions such as folic acid deficiency, the total count falls abnormally (leukopenia).
The total count of WBC is also of diagnostic value in many diseases.
Monocytes have kidney shaped nucleus.
The process by which monocytes and neutrophils squeeze out through thin capillary walls is Diapedesis.
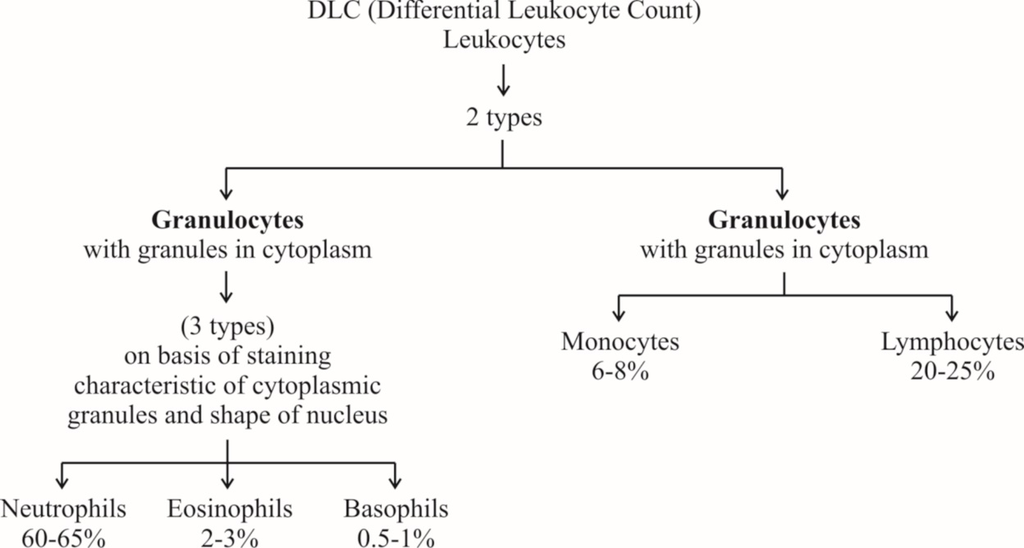
(a) Neutrophils: They are maximum in number, stain equally with both basic and acidic dyes and have many lobed nucleus, granules are in abundance in cytoplasm and help in phagocytosis.
(b) Eosinophils: They have bilobed nucleus, stain with acidic stains. Their number increases during allergic reactions (Eosinophilia).
(c) Basophils: They stain with basic dyes. Their nucleus is 'S' shaped. Coarse granules are few in the cytoplasm. Basophils release heparin and histamine in the blood and have a function similar to the mast cells.
(d) Lymphocytes have large and rounded nucleus. The cytoplasm forms a thin peripheral film. They have their stem cells in the bone marrow and are differentiated in the bone marrow or in the thymus. Lymphocytes are of two types, B-lymphocytes and T-lymphocytes.
B-lymphocytes produce antibodies against antigens and they mature in the bone marrow.
(e) Monocytes are the largest leucocytes (12-15 µm). The nucleus is kidney shaped. They are produced from bone marrow monoblast cells. They help in phagocytosis.
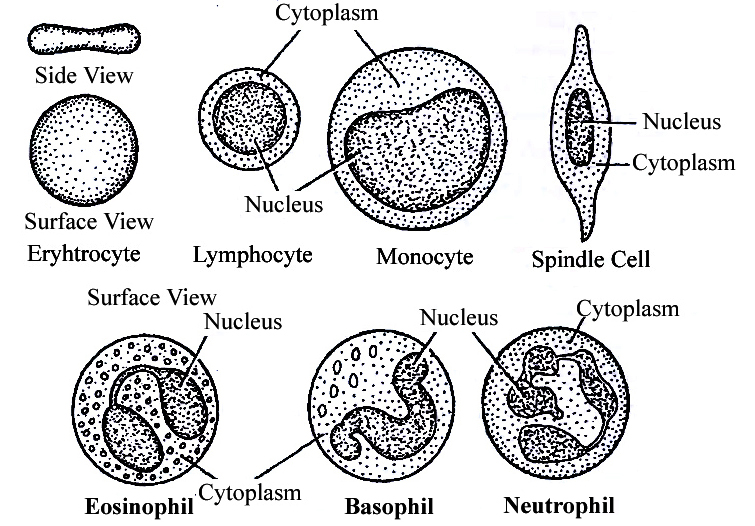
Table: Differences between different types of Leucocytes
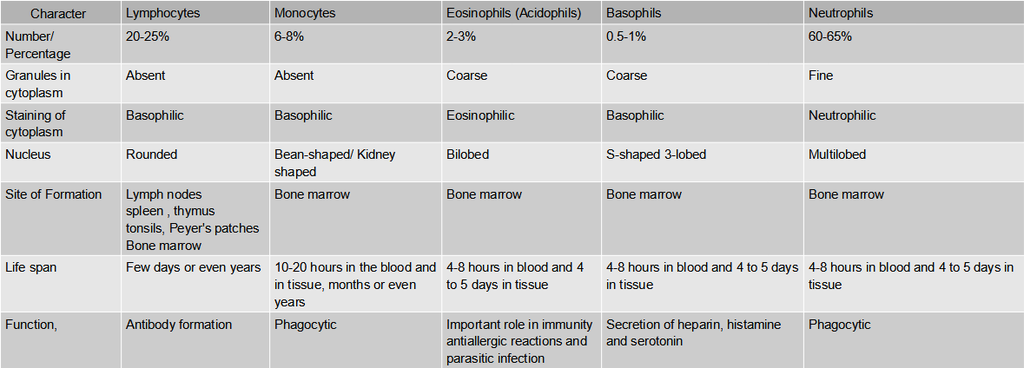
(iii) Blood platelets:
Also called thrombocytes, blood platelets are non-nucleated, round or oval, biconvex disc-like bodies.
They are 2-3 micrometres in diameter and their number normally varies from 0.15 to 0.35 million/mm3 or 150000 -350000 platelets/mm3.
They bud off from the cytoplasm of very large Megakaryocytes of the bone marrow.
Their normal life-span is about a week.
When a blood vessel is injured, platelets get clumped at the injured spot and release certain chemicals called Platelet Factors.
These promote blood coagulation.
Thrombocytopenia is decrease in platelet count and Purpura is a group of bleeding diseases due to thrombocytopenia.
BLOOD COAGULATION
When blood oozes out of a cut, it sets into gel within a few minutes. This is called coagulation.
Coagulation is brought about by hydrolysis of soluble fibrinogen of plasma to insoluble fibrin.
This is catalysed by an enzyme called thrombin.
Fibrin precipitates as a network of fibres.
This network traps many blood cells, particularly RBCs, to form a red solid mass called the Blood Clot.
The clot seals the wound in the vessel to stop the bleeding.
The straw coloured fluid left after clotting of blood, is called Serum.
The serum cannot be coagulated as it lacks fibrinogen.
Thrombin occurs in normal blood as an inactive globulin called Prothrombin.
It must be activated to thrombin before blood coagulation can occur.
In case of injury to a blood vessel, coagulation promoting substances called Thromboplastins are released into the blood from clumped platelets and damaged tissues.
Thromboplastins help in the formation of the enzyme Prothrombinase.
This enzyme hydrolyses prothrombin to thrombin to initiate coagulation.
Ca2+ ions are essential for both activation and action of thrombin.
Blood normally contains an anticoagulant, Heparin which prevents activation of prothrombin, Heparin is released from mast-cell granules.
Blood also contains Antithrombin which inhibits any thrombin formed accidentally.
Blood drawn from a blood vessel can be kept uncoagulated by adding a pinch of oxalate (sodium or potassium oxalate) to it.
Oxalate precipitates Ca2+ and consequently prevents coagulation.
Chilling of blood also delays coagulation because lesser temperature depresses the action of coagulation promoting enzymes.
ABO Blood cloting factor:
Karl Landsteiner reported for the first time ABO blood groups in human beings.
A. B and O blood groups were discovered by Landsteiner (1900) while AS blood group was found out by de Castello and Steini (1902).
Agglutinogens (antigens) are present on the surface of red blood corpuscles and agglutinins (antibodies) are found in the blood plasma. Both antigens and antibodies are proteins.
When two different type of blood are mixed, the red blood corpuscles form a clump.
The clumping of red blood corpuscles is called agglutination.
Clotting Factors:
13 factors help in blood clotting.
These factors are mainly produced in liver.
Vitamin K is required in the synthesis of these clotting factors.
These factors are represented in Roman number.
I – Fibrinogen
II – Prothrombin
III – Thromboplastin
IV – Ca+2 (cofactor in each step of blood clotting)
V – Proaccelerin
VI – Accelerin (Rejected)
VII – Proconvertein
VIII – AHG Anti Haemophelic Globin (Absent in Haemophilia-A)
IX – Christmas factor
X – Stuart factor
XI – PTA (Plasma Thormboplastin Anticedent)
XII – Hagman factor
XIII – FSF Factors (Fibrin stabilizing factor) (Laki Lor and factor).
Other natural anticoagulants are
Hirudin – found in leech.
Anophelin – found in female Anophelese.
Lampredin – found in Peteromyzon (Lamprey)
Cumerin – obtain from plants
Warfarin – obtain from plants
To collect blood in bottle in blood bank artificial anticoagulants are used like
Sodium citrate
Sodium oxalate
EDTA (Ethylene diamine tetra acetic acid)
These chemicals act as Calcium binding units and remove Ca+2 ions from blood.
Blood group
Agglutination is due to the interaction of antigens and antibodies.
There are two kinds of antigens that are named A and B.
There are also two kinds of antibodies which are called a and b.
The antigen A and antibody a are incompatible (antagonistic) and cause self clumping and cannot exist together.
Similarly, the antigen B and antibody b are incompatible and cause self clumping and cannot exist together.
Thus, A and b can exist together and B and a can exist together.
The corpuscle factors A and B can occur together if their antagonistic plasma factors a and b are not present.
The plasma factors a and b can occur together if their antagonistic corpuscle factors A and B are absent.
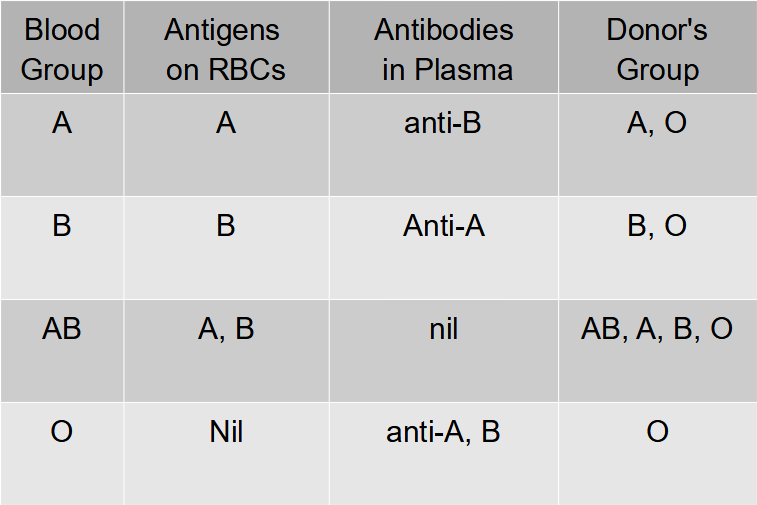
Rh Factor
Another-antigen, the Rh antigen similar to one present in Rhesus monkeys (hence Rh), is also observed on the surface of RBCs of majority (nearly 80 per cent) of humans.
In India % ratio of Rh is
Rh+ – 97%
Rh– – 3%
In World
Rh+ – 80%
Rh– – 20%
Such individuals are called Rh Positive (Rh+ve) and those in whom this antigen is absent are called Rh negative (Rh-ve).
An Rh-ve person, if exposed to Rh+ve blood, will form specific antibodies against the Rh antigens.
Therefore, Rh group should also be matched before transfusions.
A special case of Rh incompatibility (mismatching) has been observed between the Rh-ve blood of a pregnant mother with Rh+ve blood of the foetus.
Rh antigens of the foetus do not get exposed to the Rh-ve blood of the mother in the first pregnancy as the two bloods are well separated by the placenta.
However, during the delivery of the first child, there is a possibility of exposure of the maternal blood to small amounts of the Rh+ve blood from the foetus.
In such cases, the mother starts preparing antibodies against Rh antigen in her blood. In case of her subsequent pregnancies, the Rh antibodies from the mother (Rh-ve) can leak into the blood of the foetus (Rh + ve) and destroy the foetal RBCs.
This could be fatal to the foetus or could cause severe anaemia and jaundice to the baby.
This condition is called erythroblastosis foetalis.
This can be avoided by administering anti-Rh antibodies to the mother immediately after the delivery of the first child.
Lymph (Tissue Fluid)
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
LYMPHATIC SYSTEM
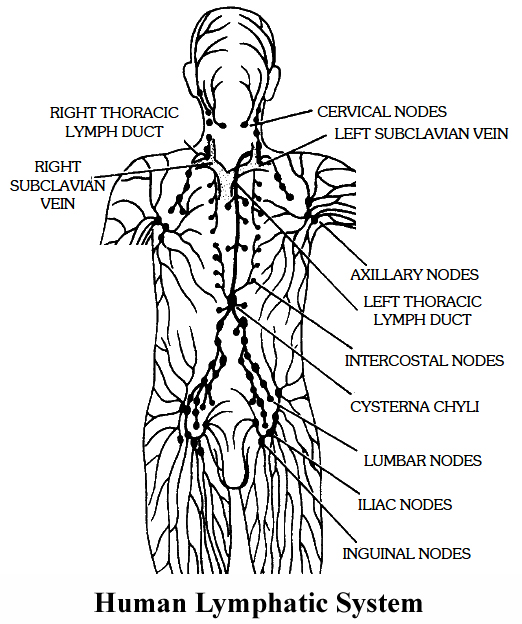
It comprises of lymph, lymphatic capillaries, lymphatic vessels, lymphatic ducts and 'lymphatic nodes.
1. Lymphatic capillaries: They lie close to the blood capillaries but end blindly. They have extremely thin walls. They are composed of a single layer of endothelial cells.
2. Lymphatic vessels : The lymphatic capillaries unite to form larger lymphatic vessels. They are composed of an outer coat of fibrous tissue, middle coat of muscular tissue and an inner lining of endothelial cells. The lymphatic vessels have numerous valves. The lymph vessels of intestinal regions absorb the digested fats. They are milky in appearance and are called lacteals (Iaetos : milk).
3. Thoracic duct: The lymphatic vessel of left side begins at the cisterna chyli , present at the level of (anterior to) the first and second lumbar vertebrae. It discharges its lymph into the left subclavian vein.
4. Right lymphatic duct: The lymphatic vessels of the right side of the thorax, head and neck unite to form the right lymphatic duct. It discharges its lymph into the right subclavian vein .
5. Lymphatic nodes: The lymphatic vessels bear lymph nodes at intervals and are abundant in the neck, armpit and groin. The lymph is filtered through lymph nodes which contain phagocytic white blood corpuscles and macro phages which eat harmful microorganisms and foreign particles from the lymph. Lymph nodes also add lymphocytes and antibodies.
Lymph Movement: The lymph flows slowly and moves from lymphatic vessels, lymphatic ducts to the venous system. Blocking of lymph flow causes oedema.
Lymphoid Organs : The organs which secrete lymph are called lymphoid organs. Besides the lymph nodes, tonsils, thymus gland, Peyer's patches, liver and spleen are the other lymphoid organs that secrete lymph.
Functions of Lymph
1. Lymph acts as a "middle man" which transports various proteins, hormones, etc., to the body cells and brings carbon dioxide and other metabolic wastes, from the body cells and finally pours the same into the venous system.
2. Lymph nodes produce lymphocytes. Lymph takes lymphocytes and antibodies from the lymph nodes to the blood.
3. It absorbs and transports fat and fat soluble vitamins from the intestine. Lymph capillaries present in the intestinal villi are called lacteals which are associated with absorption and transportation of fat and fat soluble vitamins.
4. It brings plasma protein macromolecules synthesized in the liver cells and hormones produced, in the endocrine glands to the blood. These molecules can not pass into the narrow blood capillaries but can diffuse into the lymphatic capillaries.
5. Lymph maintains the volume of the blood. As soon as the volume of the blood reduces in the blood vascular system, the lymph rushes from the lymphatic system to the blood vascular system.
Circulatory Pathways
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
BLOOD VESSELS AND COURSE OF CIRCULATION OF BLOOD
Arterioles:
Arterioles are small arteries that deliver blood to capillaries. Arterioles also have smooth muscles on their walls.
Contraction and relaxation of these muscles alter the diameter of arterioles and thereby respectively reduce and increase the blood flow through them.
Capillaries:
Capillaries were discovered by Malpighi in 1661.
Capillaries are the smallest blood vessels in the body.
Capillary has no muscular wall.
Its wall is made of a single layer of flat endothelial cells and is consequently very permeable to water and small solutes, but not to proteins and other macromolecules.
The diameter of lumen of capillaries is from 7.5 µm to 75 µm. Only about 5 to 7% of the total volume of blood is contained in the capillaries.
Venules:
Venules are small vessels that continue from capillaries and merge to form veins. They drain blood from capillaries into veins.
Veins:
Veins have less elastic tissue and smooth muscle than arteries.
One major difference between an artery and vein is that vein has a thin muscular wall.
Veins contain valves to prevent backflow of blood.
Valves are necessary in veins but not in arteries because pressure in veins is low to push the blood.
Weak valves can lead to varicose veins or haemorrhoids.
All veins carry deoxygenated blood except pulmonary veins.
Pulmonary veins carry oxygenated blood from lungs back to heart.
Blood vessels that carry blood from lungs to heart are called pulmonary veins.
Wall of veins is collapsible (non collapsible in arteries).
Lumen of vein is wider and narrow than arteries.
Most veins are located close to skin (deep in body in case of arteries).
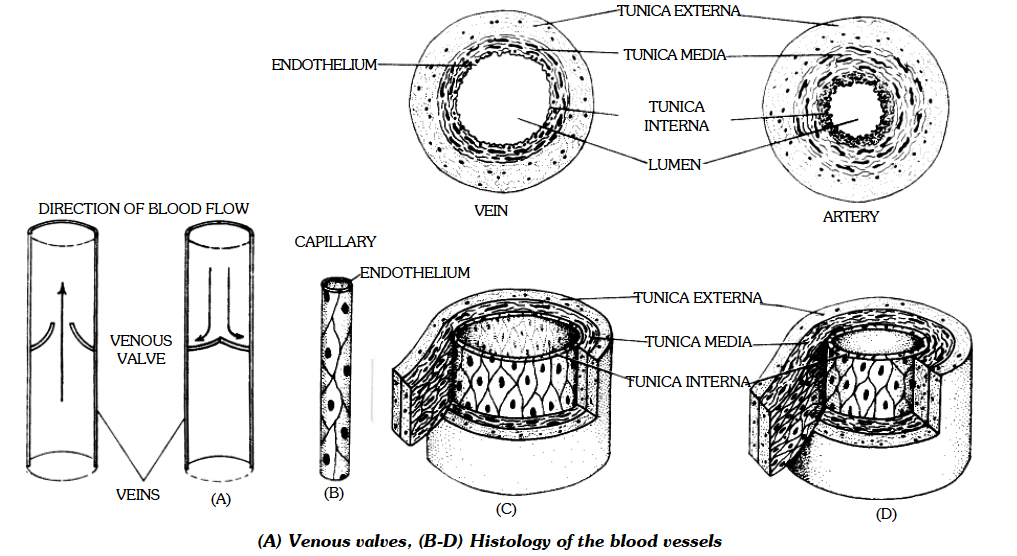
Vasa Vasorum : Blood vessels which supply blood to blood vessel are 'vasa vasorum'.
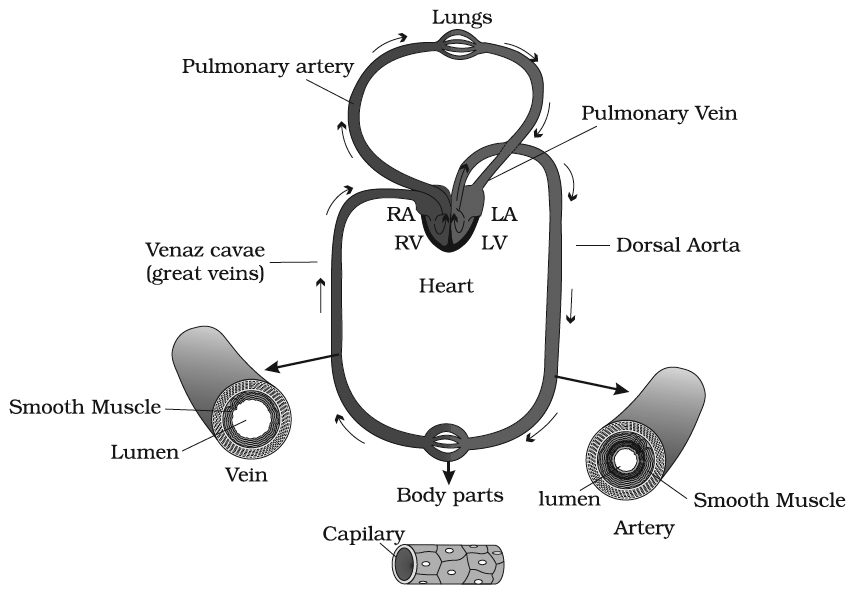
Course of Circulation of Blood
There are three types of circulation :
(a) Pulmonary circulation: from heart to the lungs and back.
(b) Systemic circulation: when blood is passed to different parts of the body.
(c) Portal circulation

Regulation of Cardiac Activity
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
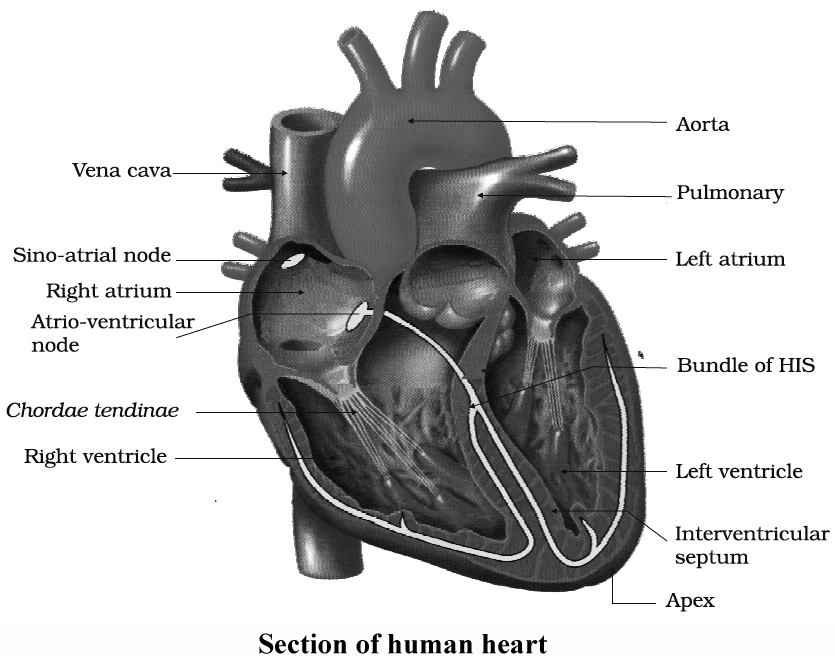
Heart Beat: Regulation
Normal activities of the heart are regulated intrinsically, i.e., auto regulated by specialised muscles (nodal tissue), hence the heart is called myogenic.
A special neural centre in the medulla oblangata can moderate the cardiac function through autonomic nervous system (ANS).
Neural signals through the sympathetic nerves (part of ANS) can increase the rate of heart beat, the strength of ventricular contraction and thereby the cardiac output.
On the other hand, parasympathetic neural signals (another component of ANS) decrease the rate of heart beat, speed of conduction of action potential and thereby the cardiac output.
This happens because these nerves release chemicals (hormones) when stimulated. Adrenal medullary hormones can also increase the cardiac output.
(i) High levels of potassium and sodium ions decrease heart rate and strength of contraction.
(ii) An excess of calcium ions increases heart rate.
(iii) Increased body temperature during fever increases heart rate.
(iv) Strong emotions such as fear, anger and anxiety increase heart rate, resulting in increased blood pressure.
(v) Mental states such as depression and grief decrease heart rate.
(vi) The heart beat is somewhat faster in females.
(vii) The heart beat is fastest at birth, moderately fast in youth, average in adulthood and above average in old age.
Heart Sounds
These are caused due to sudden closure of the valves of heart. There are mainly two sounds.
(i) First Sound : Occurs at the onset of ventricular systole and is caused due to the sudden closure of AV valves and the ejection of blood from the ventricles. It is dull and pronounced as L -U -B.
(ii) Second Sound : Occurs at the onset of ventricular diastole and is caused by sudden closure of the semilunar valves of the aorta and pulmonary artery.
It is short and sharp like the word D -U -P.
The sequence of both these sounds is like this : first sound ® second sound ® pause; first sound ® second sound ® pause; so on. Sometimes if damage occurs as in rheumatic fever, blood may leak out through the valrves and a characteristic sound mur-mur is produced.
Pulse Rate
The blood is pumped from the ventricles of the heart into the aorta to be distributed to all the parts of the body.
This happens during the ventricular systole and is repeated after every 0.8 seconds.
The blood from aorta then goes to other arteries of the body.
This causes a rhythmic contraction of the aorta and its main arteries and is felt as regular jerks or pulse in them.
It can be felt in the regions where arteries are present superficially like wrist, neck and temples.
The pulse rate is, therefore, same as that of heart beat rate.
Electrocardiogram (ECG)
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
ECG (ELECTROCARDIOGRAM)
Electric changes of the cardiac chambers follow a specific sequence.
These changes can be recorded with the help of an apparatus-electrocardiograph.
The record is called ECG.
It is represented as PQRST; where P = depolarisation of atria; QRS = depolarisation of ventricles and T = repolarisation of ventricles.
Defects in cardiac function or structure are recorded in the ECG.
For the purpose of recording, metal electrodes or leads are attached in each arm and leg with the help of straps after cleaning and putting a special jelly, which improves electrical conduction.
An additional electrode is placed on the chest with the help of a rubber suction cup.
Then, the electrocardiograph is switched on.
The electrical current of the heart is detected and amplified by the machine and is transmitted to the recording pen that draws a wavy line, called the deflection waves (electrocardiogram).
A normal electrocardiogram is composed of a P wave, a QRS complex and a T wave.
The QRS complex has three separate Q, Rand S waves.
The P wave is a small upward wave that indicates the depolarisation of the atria or the spread of impulse from the sinus node throughout the atria.
The second wave, i.e., the QRS complex, begins after a fraction of a second of the P wave.
It begins as a small downward deflection (Q) and continues as large upright (R) and triangular wave, ending as downward wave (S) at the base.
This is the expression of the ventricular depolarisation.
The potential generated by the recovery of ventricle from the depolarisation state is called the repolarisation wave.
In electrocardiography, P-Q interval (also called PR interval) is the time taken by the impulse to travel through atria, AV node and the rest of the conducting tissues.
During rheumatic fever and in arteriosclerotic heart disease (i.e., the formation of plaques and calcification), the P-Q interval lengthens.
This is due to the inflammation of atria and atrioventricular node.
The normal PR interval lasts for 0.16 second.
The enlarged Q and R waves are the indication of myocardial infarction.
The ST intervai is the representation of time between the end of the spread of impulse through ventricles and its repolarisation.
The S-T segment is elevated in acute myocardial infarction and depressed in a condition when the heart muscles receive insufficient oxygen.
The ventricular repolarisation is represented as T wave.
When the heart muscles receive insufficient oxygen, then the T wave is flattened.
Disorders of Circulatory System
- Books Name
- ACME SMART COACHING Biology Book
- Publication
- ACME SMART PUBLICATION
- Course
- CBSE Class 11
- Subject
- Biology
Disorders of Circulatory System
High Blood Pressure (Hypertension):
Hypertension is the term for blood pressure that is higher than normal (120/80).
In this measurement, 120 mm Hg (millimetres of mercury pressure) is the systolic, or pumping, pressure and 80 mm Hg is the diastolic, or resting, pressure.
If repeated checks of blood pressure of an individual is 140/90 (140 over 90) or higher, it shows hypertension.
High blood pressure leads to heart diseases and also affects vital organs like brain and kidney.
Coronary Artery Disease (CAD):
Coronary Artery Disease, often referred to as atherosclerosis, affects the vessels that supply blood to the heart muscle.
It is caused by deposits of calcium, fat, cholesterol and fibrous tissues, which makes the lumen of arteries narrower.
Angina:
It is also called 'angina pectoris'.
A symptom of acute chest pain appears when no enough oxygen is reaching the heart muscle.
Angina can occur in men and women of any age but it is more common among the middle-aged and elderly.
It occurs due to conditions that affect the blood flow.
Heart Failure:
Heart failure means the state of heart when it is not pumping blood effectively enough to meet the needs of the body.
It is sometimes called congestive heart failure because congestion of the lungs is one of the main symptoms of this disease.
Heart failure is not the same as cardiac arrest (when the heart stops beating) or a heart attack (when the heart muscle is suddenly damaged by an inadequate blood supply).
Concept Builder
1. Lowest level of glucose is in hepatic vein.
2. Highest levels of amino acids are present In hepatic vein.
3. Highest level of urea is in hepatic vein and towest in renal vein.
4. Largest vein in human body-Inferior vena cava.
5. Largest Artery-Aorta.
6. Smallest blood vessel in the body-Blood capillary.
7. The giraffe's blood pressure may be the highest of all animals because it has to pump the blood to the head through long neck.
8. One species of Antarctic fish is the only fish known to have white blood. It has no red pigment in its blood.
9. Frog has two pairs of lymph hearts to pump lymph back into veins.
10. Thrombopenia: Decrease in biood platelet count.
11. Erythropoietin: Hormone secreted by the juxta-glomerular cells of the kidneys.
12. Circulatory shunts in foetus.
Foetus bypasses pulmonary system through two shunts-foramen ova Ie (opening in interatrial septum) and ductus arteriosus (connection between dorsal aorta and pulmonary arCh). Shunts are sealed after birth.
13. Lung fish has 3 chambered heart: two auricles and one ventricle.
14. Crocodiles, alligators and gavialis have four chambered heart (two auricles and two ventricles).
15. The heart of fish is called venous heart because it receives and pumps deoxygenated blood.
16. In human heart, auricles are called atria (Sing. atrium).
17. Nereis and Amphioxus do not have heart. Heart of prawn contains oxygenated blood.
18. There is single blood circulation in fish heart. Hearts of amphibians, reptiles, birds and mammals have double blood circulation. Foramen of Panizzae is present in between two systemic arches (they arise from the heart) of the heart of lizard and crocodiles. Average human heart is about 12 cm. Average weight of human heart-male 300g, female 250 g. The opening of the coronary sinus into the right atrium is guarded by Thebesian valve. The opening of inferior vena cava into the fight atrium has I:ustachian valve. Fossa ovalis is a depression on the interatrial septum.
19. Coronary angiography : When the contrast medium dye is injected in coronary arteries (arteries of heart) and pictures are taken, it is known as coronary angiography.
20. Excess calcium ions cause increased heart beat.
21. RBCs fail to mature if there is a deficiency of vitamin B12 and folic acid.
22. Papillary muscles are found in heart of mammals.
23. Keber's organs or pericardial glands discharge excretory products into the pericardial cavity in the fresh water mussel.
24. A "Blue baby" is the name given to an abnormal human baby who has a hole in the auricular or ventricular septum so that oxygenated and deoxygenated blood mixing take place.
25. An insect larva has red blood. The larva of genus Chironomusis called 'Blood worm'. The red colour of this larva is due to haemoglobin, which has the power of attracting and storing oxygen and giving it off to the tissues as they require it. Such larva are able to live in burrows constructed by it in the mud.
26. Vasa Vasorum are blood vessels which supply blood to the blood vessels itself.
27. Blue Whale has the largest heart.
28. Cardiomegaly is heart enlargement.
29. Angiology: Study of blood vascular and lymphatic systems.
30. Venoms of Bee and Cobra contain lecithinases which when injected into the blood stream by sting or bite break down lecithins and produce lysolecithins which in turn cause rupturing of RBC cell-membrane (cell-lysis).
31. Marey's law: Heart rate is inversely related to the systemic B.P.

 ACME SMART PUBLICATION
ACME SMART PUBLICATION
